ROSACEA: CLINICAL FEATURES AND TREATMENT CONSIDERATIONS
Faculty:
L. Austin Fredrickson, MD, FACP
L. Austin Fredrickson is an Associate Professor of Internal Medicine at Northeast Ohio Medical University, where he serves as core faculty and teaches diagnostics, therapeutics, clinical skills, and health humanities. He is board-certified in general internal medicine and practices rural primary care.
Liz Fredrickson, PharmD, BCPS, is an Associate Professor of Pharmacy Practice and Pharmaceutical Sciences at the Northeast Ohio Medical University (NEOMED) College of Pharmacy. She has eight years of experience in medical writing and research.
Pamela Sardo, PharmD, BS
Pamela Sardo, PharmD, BS, is a freelance medical writer and licensed pharmacist. She is the founder and principal at Sardo Solutions in Texas. Pam received her BS from the University of Connecticut and her PharmD from the University of Rhode Island. Pam’s career spans many years in retail, clinics, hospitals, long-term care, Veterans Affairs, and managed health care responsibilities across a broad range of therapeutic classes and disease states.
Abstract
Rosacea is a chronic, relapsing inflammatory skin condition that primarily affects the central face. This condition is characterized by persistent erythema, telangiectasias, papules, pustules, phymatous changes, and possible ocular involvement. Rosacea was previously classified into rigid subtypes but is now viewed as a spectrum of clinical phenotypes driven by immune dysregulation, microbial influences, inflammation, and environmental triggers. Rosacea can significantly impair patients' quality of life due to its visible facial manifestations and chronic course. Management requires a phenotype-based, multimodal strategy that incorporates recognizing and avoiding triggers, using gentle skin care routines, using topical and systemic pharmacotherapy, and, when indicated, procedural interventions. No single therapy can address all clinical features, and a combination of individualized treatment and long-term maintenance is often necessary. This continuing education activity will review the pathophysiology, clinical presentation, and evidence-based management of rosacea for the healthcare team. Interprofessional collaboration among physicians, physician assistants, nurses, and pharmacy personnel can enhance diagnostic accuracy, optimize pharmacotherapy, support adherence, and improve patient-centered outcomes. The roles of these team members will be discussed.
Accreditation Statements
In support of improving patient care, RxCe.com LLC is jointly accredited by the Accreditation CouncilTM for Continuing Medical Education (ACCME®), the Accreditation Council for Pharmacy Education (ACPE®), and the American Nurses Credentialing Center (ANCC®), to provide continuing education for the healthcare team.

This activity was planned by and for the healthcare team, and learners will receive 2 Interprofessional Continuing Education (IPCE) credits for learning and change.
Credits: 2 contact hour(s) (0.2 CEU(s)) of continuing education credit.
Credit Types:
IPCE Credits - 2 Credits
AAPA Category 1 Credit™️ - 2 Credits
AMA PRA Category 1 Credit™️ - 2 Credits
Type of Activity: Application
Media: Computer-Based Training (i.e., online courses)
Estimated time to complete activity: 2 contact hour(s) (0.2 CEU(s)), including Course Test and course evaluation.
Release Date: April 10, 2026 Expiration Date: April 10, 2029
Target Audience: This educational activity is for Physicians and Physician Assistants
How to Earn Credit: From April 10, 2026, through April 10, 2029, participants must:
Read the “learning objectives” and “author and planning team disclosures;”
Study the section entitled “Educational Activity;” and
Complete the Course Test and Evaluation form. The Course Test will be graded automatically. Following successful completion of the Course Test with a score of 70% or higher, a statement of participation will be made available immediately. (No partial credit will be given.)
CME Credit: Credit for this course will be uploaded to CPE Monitor® for pharmacists. Physicians may receive AMA PRA Category 1 Credit™️and use these credits toward Maintenance of Certification (MOC) requirements. Physician Assistants may earn AAPA Category 1 CME credit, reportable through PA Portfolio. All learners shall verify their individual licensing board’s specific requirements and eligibility criteria.
Statement of Need:
Rosacea is a chronic inflammatory condition that affects millions of people and presents with overlapping phenotypes, including erythema, flushing, papules and pustules, phymatous changes, and ocular involvement, often leading to delayed or missed diagnosis, especially in darker skin phototypes. Many clinicians still rely on informal visual assessment, contributing to under-recognition of quality-of-life impairment and psychosocial distress. Ocular disease remains underdiagnosed. Management gaps include inconsistent use of phenotype-based, severity-stratified treatment algorithms and suboptimal integration of topical, systemic, and procedural options for mild, moderate, and severe disease. Safety concerns, cost barriers, and adherence challenges further limit the optimization of patient outcomes. Interprofessional coordination among prescribers, nurses, pharmacists, primary care, dermatology, and eye care specialists is often fragmented, resulting in variability in diagnostic accuracy, patient education, and long-term control. This activity aims to reinforce recognition, improve diagnostic precision, and promote evidence-based management across the rosacea spectrum.
Learning Objectives: Upon completion of this educational activity, participants should be able to:
Recognize the clinical spectrum of rosacea and its impact on a patient's quality of life
Discuss how diagnostic accuracy improves with phenotype-based assessments
Describe evidence-based management strategies for mild, moderate, and severe rosacea
Disclosures
The following individuals were involved in planning, developing, and/or authoring this activity: L. Austin Fredrickson, MD, FACP; Liz Fredrickson, PharmD, BCPS; and Pamela Sardo, PharmD, BS. None of the individuals involved in developing this activity has a conflict of interest or financial relationships related to the subject matter. There are no financial relationships or commercial or financial support relevant to this activity to report or disclose by RxCe.com or any of the individuals involved in the development of this activity.
© RxCe.com LLC 2026: All rights reserved. No reproduction of all or part of any content herein is allowed without the prior, written permission of RxCe.com LLC.
Educational Activity Pre-Test
Which of the following findings most strongly supports a diagnosis of rosacea rather than acne vulgaris?
Presence of papules and pustules
Central facial distribution
Absence of comedones
Onset during adolescence
Which of the following is an appropriate first-line treatment for mild papulopustular rosacea?
Oral isotretinoin
Topical ivermectin or metronidazole
Oral doxycycline only
Laser therapy
Which of the following symptoms is most characteristic of erythematotelangiectatic rosacea?
Comedones and nodules
Truncal inflammatory lesions
Hyperkeratotic plaques
Persistent facial erythema and flushing
Educational Activity
Rosacea: Clinical Features and Treatment Considerations
Introduction
Rosacea is a chronic inflammatory skin disorder. Rosacea is best managed by team-based, structured, and patient-centered strategies that address inflammatory and vascular components while supporting long-term disease control. Early recognition, appropriate treatment selection, and patient education are all essential to prevent progression and optimize health outcomes and quality of life for patients. Interprofessional collaboration among physicians, physician assistants, nurses, and pharmacy personnel can enhance diagnostic accuracy, optimize pharmacotherapy, and support adherence to treatment. This continuing education activity will review the pathophysiology, clinical presentation, and evidence-based management of rosacea for the healthcare team.
Defining Rosacea
Rosacea is a common, chronic inflammatory skin disorder that affects millions worldwide.1 It predominantly involves the convex surfaces of the central face, including the cheeks, nose, forehead, and chin.1 Rosacea is clinically characterized by persistent centrofacial erythema, episodic flushing, visible telangiectasias, inflammatory papules and pustules, and, in some cases, phymatous tissue hypertrophy or ocular inflammation.1 This condition was previously described using discrete subtypes, but a better understanding recognizes it as a dynamic, phenotype-based condition in which patients frequently exhibit overlapping features.1,2
Current evidence suggests that rosacea results from innate and adaptive immune dysregulation, neurovascular dysfunction, and environmental triggers.1,2 These mechanisms contribute to vascular instability, chronic inflammation, and progressive connective tissue remodeling. Rosacea is also associated with systemic comorbidities and has a genetic component, which further highlights the complexity of this disease.1
Classification of Rosacea
Rosacea affects up to 10% of the global population and occurs more frequently in women, although men are more likely to develop severe phymatous changes, such as rhinophyma, a skin condition that causes an enlarged, bumpy, discolored nose.1,2,3 While the peak incidence and severity occur between ages 30 and 50, rosacea can present at any age and across all skin types.1
Individuals with fair skin are the most commonly affected; however, newer data indicate there is a meaningful prevalence in patients with darker skin phototypes, including a prevalence of approximately 3.9% in Latin American populations and 2.3% in Black/African American populations.5 The "classic" bright red erythema may be masked by melanin and appears as violaceous, dusky, or hyperpigmented patches.5 Delays in diagnosis are common for these patient populations, leading to more advanced disease at presentation and a higher incidence of post-inflammatory hyperpigmentation (PIH).5 Clinicians should look for secondary signs such as warm skin temperature, "stinging" sensations, and persistent edema rather than relying solely on visual redness to establish the diagnosis.5
The most widely adopted classification framework was developed by the National Rosacea Society Expert Committee (NRSEC).4 This system recognizes rosacea as a spectrum of clinical features, and a diagnosis is suggested by the presence of one or more characteristic features in a central facial distribution.4 These form distinct clinical patterns, which were historically referred to as subtypes, and patients frequently exhibited overlapping characteristics.1,2,4,6
Classifications for rosacea are as follows:4
Erythematotelangiectatic rosacea (ETR): Persistent central facial erythema with episodes of flushing and visible telangiectasias6
Papulopustular rosacea: Persistent erythema accompanied by inflammatory papules and pustules without comedones6
Phymatous rosacea: Tissue hypertrophy and irregular surface nodularity, most commonly affecting the nose (rhinophyma)6
Ocular rosacea: Inflammatory involvement of the eyes, including blepharitis, keratitis, iritis, and recurrent chalazia6
Patients will often present with features spanning multiple categories, so rosacea should be viewed as a dynamic inflammatory condition rather than a tightly staged disease.2,4 Recognizing the predominant clinical pattern and associated features is essential for healthcare teams to guide therapy and determine the need for referral to specialists, especially in cases of phymatous or ocular involvement.
Epidemiology
Estimates in mostly fair-skinned populations suggest a prevalence rate ranging from 2% to 22%, depending on study design and diagnostic criteria.7 A prospective German study reported an overall prevalence of 12%, with erythematotelangiectatic rosacea accounting for approximately 9% and papulopustular rosacea for 3%.8 Cutaneous rosacea demonstrates a clear female predominance, except in the phymatous subtype, and is most often diagnosed after age 30.9
A multinational study including over 50,000 individuals across 20 countries estimated a worldwide rosacea prevalence of approximately 5.1%, which aligns with pooled data from earlier population-based studies reporting a prevalence of 5.46%.9
Ocular involvement occurs in a notable proportion of patients, with a reported prevalence ranging from less than 10% to greater than 50%.9 Age distribution patterns vary across studies. While rosacea has traditionally been considered most common in adults over 40 years of age, newer data suggest a notable prevalence in individuals aged 25–39 years, indicating that clinically significant disease may occur earlier than previously recognized.9
Etiology and Pathophysiology of Rosacea
The pathophysiology of rosacea is not fully understood. It has been described as a multifactorial inflammatory process that involves immune dysregulation, vascular hyperreactivity, microbial triggers, genetic susceptibility, and environmental influences.10 Clinical and histopathologic findings support the involvement of both innate and adaptive immune pathways, as well as neurovascular and oxidative mechanisms.10
Rosacea appears to result from an exaggerated inflammatory response in the skin. Patients with rosacea have heightened activity of components of the innate immune system, particularly toll-like receptor 2 (TLR-2).11 This receptor acts as a “danger sensor” in the skin and becomes overactive in response to common triggers, including ultraviolet light, heat, and environmental stress.11 When activated, TLR-2 stimulates skin cells to release pro-inflammatory cytokines, including IL-1, IL-8, and TNF-α, amplifying redness and inflammation.11
This immune activation also increases production of antimicrobial peptides such as LL-37.12 In rosacea, LL-37 is processed into abnormal forms that promote blood vessel growth, leukocyte recruitment, and connective tissue remodeling.12 These changes contribute to persistent erythema, telangiectasias, and, in some cases, tissue thickening.12 Matrix metalloproteinases (MMP-2 and MMP-9) are also elevated and contribute to vascular dilation and dermal matrix breakdown. In parallel, reactive oxygen species (ROS) are increased, further driving inflammation and vascular changes.12 Ultraviolet exposure exacerbates these processes by inducing oxidative stress and activating angiogenic pathways.12
The adaptive immune system also plays a role. Rosacea lesions exhibit increased CD4⁺ T-cell infiltration, with a predominance of Th1 and Th17 cells. Elevated IL-17 and interferon-γ sustain inflammation and promote vascular growth.13 Neutrophil-recruiting chemokines are upregulated, helping explain pustule formation in papulopustular disease.13 In phymatous rosacea, chronic inflammation may stimulate fibrosis through cytokines, such as IL-6 and TGF–β.13
Microbial factors may also contribute in some patients, with increased Demodex mite density observed in affected skin.14 While these mites are common in healthy individuals, higher burdens may trigger immune activation in predisposed patients.14 Other microorganisms, including Staphylococcus epidermidis and Bacillus oleronius, have been implicated. Associations with Helicobacter pylori infection and small intestinal bacterial overgrowth (SIBO) have been reported, although causality remains uncertain.14
Finally, rosacea is strongly influenced by neurovascular dysregulation. Patients exhibit abnormal vascular reactivity to triggers such as heat, alcohol, spicy foods, and temperature changes.15 These stimuli activate transient receptor potential (TRP) channels in sensory nerves, leading to the release of vasoactive neuropeptides.15 The result is vasodilation, flushing, and mast cell activation. Repeated episodes of neurogenic inflammation likely contribute to persistent erythema and telangiectasia over time.15
Genetic Contributions
Familial clustering supports a genetic predisposition to rosacea. Twin studies have found greater concordance and severity among monozygotic twins than among dizygotic twins.16 Genome-wide association studies have also identified susceptibility loci near HLA-DRA and BTNL2 genes on chromosome 6.16 Specific HLA haplotypes (HLA-DRB103:01, HLA-DQB102:01, HLA-DQA1*05:01) have been associated with rosacea and overlap with autoimmune disease risk loci.16 These findings suggest a role for antigen presentation and immune activation in disease pathogenesis.16
Environmental, Dietary, and Lifestyle Factors
Ultraviolet radiation is a common trigger that increases ROS production, TLR-2 activation, angiogenic factors, and dermal matrix degradation.17 Additionally, alcohol and spicy foods activate TRPV1/TRPA1 receptors and promote vasodilation and flushing through histamine release and neuropeptide signaling.14 Psychological stress can increase sympathetic skin nerve activity and cortisol-releasing hormone (CRH)–mediated cytokine production, contributing to erythema and inflammation.18 Poor sleep quality has been associated with increased TLR-2, MMP-9, VEGF, and inflammatory mediator expression, potentially worsening disease severity.19
The increased use of personal protective equipment (PPE) and face masks following the COVID-19 pandemic also highlights the role of the cutaneous micro-environment in rosacea flares.20 The phenomenon, colloquially termed "Maskne," is driven by a combination of mechanical friction (Koebner-like phenomenon), increased humidity, and elevated skin temperature within the retro-mask space.20
Patient Case
A 46-year-old woman presents with a 3-year history of facial redness and intermittent “acne-like bumps” on her cheeks and nose. She reports burning and stinging with many skincare products. Over-the-counter benzoyl peroxide worsened her symptoms. She drinks 1–2 glasses of wine most evenings and notices flushing after exercise and hot showers. She uses a retinol cream nightly for “anti-aging.”
A physical examination reveals the following:
Diffuse centrofacial erythema
Telangiectasias on the nasal bridge and cheeks
Scattered inflammatory papules
No comedones
Mild conjunctival injection
Pause and Ponder Answer the following questions for the Patient Case above What phenotype(s) of rosacea are present? What pathophysiologic mechanisms are likely driving her symptoms? What treatment adjustments would you recommend? |
|---|
Clinical Features of Rosacea
Clinically, rosacea is characterized by persistent centrofacial erythema, telangiectasias, inflammatory papules and pustules, and the absence of comedones, which helps distinguish it from acne vulgaris.21 Unlike with acne, truncal involvement is uncommon.21 Early disease often begins with episodic flushing triggered by heat, emotional stress, alcohol, hot beverages, or spicy foods.21 Over time, flushing episodes may become more prolonged and eventually lead to fixed erythema with superimposed inflammatory lesions.21
Flushing6
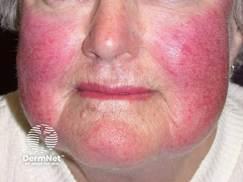
Table 1 lists the clinical manifestations of rosacea, and Table 2 lists important clinical findings.
Table 1
Manifestations of Rosacea21
| Category | Feature | Description |
|---|---|---|
| Core manifestations | Episodic flushing | Recurrent episodes of facial blushing or flushing, often reported as a long-standing tendency |
| Persistent facial redness | Ongoing erythema of the central face; this is the most frequently observed clinical sign | |
| Inflammatory papules and pustules | Red, raised lesions that may contain pus; lesions often appear in clusters and may occasionally progress to nodules | |
| Visible blood vessels | Dilated superficial facial vessels are commonly present, but are not required to establish the diagnosis | |
| Associated manifestations | Sensations of burning or stinging | Patients may experience discomfort such as burning or stinging, sometimes with scaling or dermatitis, particularly over the cheeks |
| Plaque formation | Well-demarcated red plaques that occur without surrounding epidermal abnormalities | |
| Dry or rough skin texture | Central facial skin may appear coarse or scaly, mimicking xerosis; this is often linked to irritation rather than intrinsic disease activity | |
| Facial swelling | Soft tissue edema may develop during or after prolonged flushing or erythema, sometimes creating a sensation of facial fullness and lasting several days | |
| Eye involvement | Ocular symptoms range from irritation and itching to conjunctival redness and eyelid inflammation; complications may include styes, chalazia, or corneal injury | |
| Non-facial involvement | Lesions may extend beyond the face, though the prevalence and significance of extrafacial involvement are not well defined |
Table 2
Clinical Findings of Rosacea21
| Finding | Severity Rating |
|---|---|
| Episodic facial flushing | None / Mild / Moderate / Severe |
| Persistent facial erythema | None / Mild / Moderate / Severe |
| Inflammatory lesions (papules/pustules) | None / Mild / Moderate / Severe |
| Visible superficial vessels | None / Mild / Moderate / Severe |
Telangiectasias6
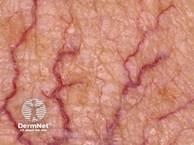
Clinical findings of rosacea should be systematically evaluated and graded by severity, as described below:21
Patients may report burning or stinging sensations, which should be rated as: none, mild, moderate, or severe.
The presence and extent of erythematous plaques should be assessed in a similar manner.
Skin texture changes, including a rough or dry appearance of the affected areas, should be documented and graded by severity.
Facial swelling should be evaluated on a severity scale. When edema is present, clinicians should note whether it is acute or long-standing.
In cases of chronic swelling, further characterization, such as pitting or non-pitting edema, is recommended.
Ocular involvement, which can range from absent to severe, should be assessed and documented.
The presence of extrafacial disease should be recorded as absent or present, with specific anatomic locations noted when applicable.
Evidence of tissue hypertrophy, consistent with phymatous changes, should be evaluated and graded according to severity
Patient-reported overall disease severity should be captured using a global assessment, in which patients rate their perceived disease burden as none, mild, moderate, or severe.21
Diagnosis and Evaluation
Rosacea is a clinical diagnosis based on characteristic cutaneous findings and does not require routine laboratory or histopathologic confirmation.4 The 2017 National Rosacea Society consensus defines diagnostic rosacea as persistent central facial erythema that may fluctuate in intensity or the presence of phymatous tissue changes.4 In the absence of these diagnostic phenotypes, two or more major features, including flushing, papules and pustules, telangiectasia, or ocular manifestations, support the diagnosis.4 A focused history should assess trigger factors (e.g., heat, alcohol, spicy foods, ultraviolet exposure, emotional stress), symptom chronology, prior treatments, and ocular complaints.4
Physical examination should evaluate the distribution (typically central face), severity of erythema, presence of inflammatory lesions without comedones (to distinguish rosacea from acne vulgaris), telangiectasia, tissue hypertrophy, edema, and extrafacial involvement.4 Severity assessment using standardized grading scales or clinician global assessment tools is recommended to guide therapeutic selection and monitor response. Skin biopsy is rarely required but may be considered when alternative diagnoses such as lupus erythematosus, dermatomyositis, seborrheic dermatitis, or cutaneous lymphoma are suspected.4
Ocular involvement is a frequently overlooked component, occurring in up to 50% of patients and sometimes preceding cutaneous symptoms.22 It often presents as blepharitis, conjunctival injection, or a "gritty" foreign body sensation.22 While often mild, chronic inflammation can lead to vision-threatening complications, including keratitis and corneal ulceration, necessitating a high index of suspicion and low threshold for ophthalmologic referral.23 Ocular examinations should screen for conjunctival injection, blepharitis, or meibomian gland dysfunction, with ophthalmology referral for moderate to severe ocular disease.23
Diagnostic accuracy improves with phenotype-based assessment rather than traditional subtyping. Under the current consensus, the presence of persistent centrofacial erythema or phymatous changes is considered diagnostic.4 In their absence, a combination of two or more major features, such as flushing, inflammatory papules, or ocular manifestations, must be present.4 Clinicians must distinguish rosacea from several similar conditions. Unlike acne vulgaris, rosacea is notably absent of comedones, and unlike systemic lupus erythematosus, the erythema of rosacea typically involves the nasolabial folds.4
Pause and Ponder What are the potential long-term consequences of untreated chronic inflammation (e.g., persistent erythema, phymatous change, ocular complications)? |
|---|
The Treatment and Management of Rosacea
The management of rosacea requires a long-term, individualized, and multimodal approach due to the disease's heterogeneity.21 No single therapy addresses all features, and combination treatment is frequently necessary to control erythema, inflammatory lesions, and vascular instability.21 Core components of management include patient education, structured skin care, pharmacologic therapy, and procedural interventions such as laser and light-based therapies.21 Treatment selection should be guided by predominant subtype features, disease severity, tolerability, comorbidities, and patient preferences.21
Topical Therapy
Topical therapy is considered first-line for mild-to-moderate rosacea, particularly erythematotelangiectatic and papulopustular subtypes.2,21 The choice of agent depends on dominant clinical features and skin sensitivity. The vehicle formulation significantly influences tolerability and adherence.2,21 Food and Drug Administration (FDA)-approved topical agents include the following:
azelaic acid
metronidazole
sodium sulfacetamide/sulfur
brimonidine
oxymetazoline
ivermectin
Azelaic acid reduces erythema and inflammatory lesions by inhibiting neutrophil-derived reactive oxygen species. It has demonstrated efficacy equal to or superior to that of metronidazole in papulopustular rosacea.24 Metronidazole exerts anti-inflammatory effects through suppression of neutrophil activity and remains a widely used option with good tolerability across varying dosage strengths.25 Sodium sulfacetamide/sulfur combinations provide additional anti-inflammatory benefit and may be particularly helpful in combination regimens.26
Oxymetazoline 1% cream, an α1-agonist, has demonstrated sustained efficacy and tolerability for persistent erythema with once-daily use.26 Ivermectin 1% cream is particularly effective for papulopustular rosacea due to its combined anti-inflammatory and anti-parasitic activity against Demodex folliculorum and has shown superior efficacy compared to vehicle and metronidazole in reducing inflammatory lesions.2 Calcineurin inhibitors such as tacrolimus and pimecrolimus may be useful in select cases, particularly steroid-induced rosacea, though evidence remains limited.28
For patients with persistent facial erythema, alpha-adrenergic agonists can offer targeted vasoconstrictive effects.29 Brimonidine gel produces rapid improvement in erythema through selective α2-receptor activity, with an onset of action that typically occurs within 30 minutes.29 Transient rebound erythema may occur with this agent.29 Topical brimonidine and oxymetazoline should be used cautiously or avoided in patients with any of the following:
Severe cardiovascular disease
Cerebral or coronary insufficiency
Raynaud phenomenon
Thromboangiitis obliterans
Orthostatic hypotension
Severe peripheral vascular disease
Narrow-angle glaucoma
Scleroderma
Sjögren disease
Brimonidine also warrants caution in patients with major depressive disorder, as systemic alpha-2 agonism may theoretically worsen depressive symptoms. Patients with labile blood pressure, who are of advanced age, or are on multiple medications, should be counseled carefully.29
Rebound erythema has been reported most often with topical brimonidine use. Available data suggest that approximately 10% to 20% of patients may experience worsening erythema, either several hours after application or after discontinuation.29 Although severe transient rebound reactions have been documented, they are uncommon.29 In contrast, oxymetazoline appears to have a substantially lower incidence of rebound erythema, with long-term studies reporting rates of less than 1%.29 Patients should be counseled regarding the potential for rebound flushing and advised to initiate therapy cautiously, such as applying the medication to a small test area initially, to assess tolerability before full-face application.29
Systemic Therapies
Systemic therapy is indicated for moderate-to-severe papulopustular rosacea, refractory disease, ocular involvement, or phymatous changes.2 Use of doxycycline is commonly used because of its anti-inflammatory properties, including inhibition of cytokines, angiogenesis, leukocyte chemotaxis, and matrix metalloproteinases. Modified-release doxycycline (40 mg daily) provides effective control of inflammatory lesions while reducing the risk of antibiotic resistance.30 Ocular rosacea also responds favorably to low-dose doxycycline.30
Combination Therapies
Combination regimens incorporating oral doxycycline with topical azelaic acid or metronidazole may improve both early response and long-term control.21 Macrolides (azithromycin and clarithromycin) can be used as alternatives for patients who do not tolerate tetracyclines.1 Low-dose isotretinoin may be considered in cases of refractory papulopustular or phymatous rosacea, demonstrating sustained efficacy in carefully selected patients with appropriate monitoring.1 Oral metronidazole and other systemic agents have been used in limited contexts, though supporting evidence is less robust.25
Light Therapies
Laser and light-based therapies play an important role in addressing vascular manifestations such as flushing, persistent erythema, and telangiectasia.25 Intense pulsed light (IPL) and pulsed dye laser (PDL) have demonstrated significant improvement in vascular symptoms and patient-reported quality-of-life measures.25 The potassium titanyl phosphate (KTP) laser and Nd:YAG laser are additional options for superficial and deeper vascular lesions, respectively.31,32 Ablative lasers such as carbon dioxide and erbium:YAG are reserved for phymatous rosacea, particularly rhinophyma, where tissue contouring is required.33,34 Surgical modalities, including excision and radiofrequency ablation, may be necessary in advanced cases, although risks of scarring and dyspigmentation must be discussed.35
Cleansing
Interprofessional teams should emphasize barrier restoration as a core therapeutic goal. Patients should use "syndet" (synthetic detergent) cleansers with a pH of 4.0 to 6.5, which mimic the skin's natural "acid mantle" and reduce irritation common with traditional alkaline soaps.36 For the management of acute flushing, practical interventions include the use of a "flushing diary" to isolate idiosyncratic triggers and the application of cool compresses to induce local vasoconstriction.37 For patients with persistent, debilitating flushing, off-label use of beta-blockers like carvedilol has shown efficacy in reducing neurovascular reactivity.38
Emerging Therapies
Emerging and adjunctive therapies continue to be explored. Intradermal botulinum toxin has demonstrated potential benefit in reducing flushing and erythema by inhibiting acetylcholine and neuropeptide release, though its use remains off-label and evidence is limited to small studies.39 Table 3 summarizes medications used in the management of rosacea.
Table 3
Summary of Medications to Treat Rosacea40-56
| Medication | Typical Adult Dose | Primary Indication | Common Adverse Effects (ADEs) |
|---|---|---|---|
| Azelaic acid 15% gel/foam | Apply a thin layer BID | Papulopustular rosacea, erythema | Burning, stinging, pruritus, dryness, hypopigmentation (rare) |
| Metronidazole 0.75–1% (gel/cream/lotion) | Apply once or BID | Papulopustular rosacea | Dryness, irritation, mild burning, rarely contact dermatitis |
| Ivermectin 1% cream | Apply once daily | Papulopustular rosacea | Skin irritation, pruritus, dryness, transient worsening early in therapy |
| Sodium sulfacetamide 10% / sulfur 5% | Apply 1–2 times daily | Inflammatory lesions | Dryness, odor, irritation; avoid in sulfonamide allergy |
| Brimonidine 0.33% gel | Apply once daily | Persistent erythema | Transient rebound erythema, flushing, burning, contact dermatitis |
| Oxymetazoline 1% cream | Apply once daily | Persistent erythema | Application site dermatitis, pruritus, erythema; rare systemic alpha effects |
| Doxycycline (sub-antimicrobial 40 mg MR) | 40 mg PO daily | Moderate inflammatory rosacea | GI upset, photosensitivity, esophagitis (rare), headache |
| Doxycycline (standard dose) | 50–100 mg PO once or BID | Moderate–severe disease | GI upset, photosensitivity, esophagitis, candidiasis |
| Minocycline | 50–100 mg PO once or BID | Alternative tetracycline | Dizziness, hyperpigmentation, drug-induced lupus (rare), hepatotoxicity |
| Minocycline 1.5% Foam | Apply once daily | Inflammatory papules and pustules | First topical minocycline. Avoids systemic ADEs; does not cause skin staining; fragrance-free. |
| Azithromycin | 250–500 mg PO 2–3 times weekly (varies) | Tetracycline intolerance | GI upset, QT prolongation (rare), drug interactions |
| Isotretinoin (low dose) | ~0.25–0.3 mg/kg/day | Refractory or phymatous disease | Xerosis, cheilitis, hyperlipidemia, teratogenicity, mood changes (rare) |
| Topical calcineurin inhibitors (off-label) | Tacrolimus 0.1% ointment BID | Steroid-induced rosacea (select cases) | Burning, pruritus, local irritation |
| Artificial tears (ocular) | 1–4 times daily PRN | Ocular rosacea (mild) | Minimal; blurred vision temporarily |
| Cyclosporine ophthalmic | 1 drop BID | Moderate ocular rosacea | Ocular burning, irritation |
| Encapsulated Benzoyl Peroxide (5%) | Apply once daily | Inflammatory papules and pustules | Silica-shell technology slows drug release to minimize irritation; an effective alternative to antibiotics |
Treatment Algorithm for Rosacea4
Step 1: Identify Dominant Phenotype
Persistent erythema
Telangiectasia
Papules/pustules
Ocular disease
Phymatous change
Step 2: Initiate Targeted Therapy
Persistent erythema (no telangiectasia)
Brimonidine or oxymetazoline
Prominent telangiectasia
IPL/PDL/vascular laser
Papulopustular disease (mild–moderate)
Azelaic acid/ivermectin/metronidazole
Papulopustular (moderate–severe)
Add oral doxycycline
Ocular involvement
Systemic doxycycline + ophthalmology referral
Phymatous disease
Isotretinoin (early) or laser/surgical debulking (advanced)
Step 3: Maintenance
Gentle skin care
Sunscreen
Trigger avoidance
Intermittent topical therapy
Ocular Rosacea Treatment Pathway57,58
| Severity Level | Clinical Considerations | Recommended Management |
|---|---|---|
| Mild Ocular Disease | May present with irritation, mild blepharitis, foreign body sensation, and conjunctival injection | • Lid hygiene (warm compresses twice daily) • Eyelid scrubs • Preservative-free artificial tears • Topical azithromycin ophthalmic (select cases) |
| Moderate Ocular Disease | Persistent symptoms, meibomian gland dysfunction, and inflammatory lid changes | • Oral doxycycline 40 mg modified release daily or 50–100 mg daily • Topical cyclosporine ophthalmic • Continued lid hygiene |
| Severe Ocular Disease | Significant inflammation, keratitis risk, and corneal involvement are possible | • Short-course systemic tetracycline-class antibiotics • Macrolides if tetracyclines are contraindicated • Mandatory ophthalmology referral • Monitor closely for corneal ulceration |
Pediatric Considerations
Tetracyclines are contraindicated in children under 9 years due to tooth discoloration and bone effects. The following are recommended alternative treatments.
Oral erythromycin: 30–50 mg/kg/day in divided doses
Azithromycin: Weight-based dosing
Clarithromycin: Weight-based dosing
Oral metronidazole: 20–30 mg/kg/day
Systemic therapy may be required for several months. Maintenance with topical agents follows remission.
Cost and Access Considerations
Cost and access to therapy are important determinants of adherence and treatment success in rosacea management. While several effective therapies are available, out-of-pocket costs, insurance coverage limitations, and formulary restrictions may influence treatment selection. Generic topical agents such as metronidazole and azelaic acid, as well as oral doxycycline, are generally more affordable and widely accessible. In contrast, newer or branded therapies, including ivermectin cream, oxymetazoline, and combination products, may be associated with higher costs and reduced insurance coverage, potentially limiting patient access.
Cost-related nonadherence is a recognized barrier in dermatologic care, with patients sometimes delaying refills, using medications inconsistently, or discontinuing therapy prematurely due to financial constraints.59 To address these challenges, clinicians and pharmacists should consider cost-effective alternatives, utilize generic formulations when appropriate, and be familiar with manufacturer assistance programs. Simplifying treatment regimens may also improve adherence while balancing cost considerations. Incorporating financial factors into shared decision-making is essential to ensure that treatment plans are both clinically appropriate and sustainable.
Patient Education and Counseling
Effective rosacea management depends heavily on patient education, adherence, and proper product use.4 Patients should be counseled that rosacea is a chronic, relapsing condition requiring long-term management rather than short-term treatment. Improvement with topical therapies is gradual and may take several weeks, and adherence is essential to achieve optimal outcomes.
Patients should also be counseled to identify and minimize individual triggers, including ultraviolet exposure, heat, alcohol, and spicy foods. Daily use of broad-spectrum sunscreen with physical blockers such as zinc oxide or titanium dioxide is recommended year-round.4 Gentle cleansing, avoidance of irritants (e.g., menthol, astringents, sodium lauryl sulfate), and regular moisturization support barrier integrity and improve treatment tolerance. Potent topical corticosteroids should be avoided, as chronic use may induce or exacerbate rosacea.4
Topical medications should be applied as a thin layer to the entire affected area rather than as spot treatment. Patients should avoid known triggers such as heat, alcohol, spicy foods, and ultraviolet exposure, and should use gentle, non-irritating skincare products. Sunscreen use is essential, particularly physical blockers such as zinc oxide or titanium dioxide, to reduce erythema and prevent exacerbations.
Patients using alpha-adrenergic agonists such as brimonidine should be counseled regarding the potential for rebound erythema and advised to test the medication on a small area prior to full-face application. Those receiving doxycycline should be instructed to take the medication with a full glass of water and remain upright for at least 30 minutes to reduce the risk of esophagitis. Early transient worsening of symptoms may occur with some therapies and does not necessarily indicate treatment failure.
Interprofessional (IPE) Approaches to Rosacea Management
Rosacea is a chronic, relapsing inflammatory condition that frequently requires longitudinal care and individualized treatment strategies. An interprofessional model of care enhances clinical outcomes and patient satisfaction.
Patients with mild, intermittent erythema without inflammatory lesions may be managed with nonpharmacologic measures, including trigger avoidance, gentle skin care, and sunscreen use. Limited use of OTC products such as low-irritation cleansers and moisturizers may be appropriate. Patients with persistent erythema, papules or pustules, ocular symptoms (e.g., irritation, redness, foreign body sensation), phymatous changes, or diagnostic uncertainty should see a primary care physician or provider. Patients who fail to respond to initial therapy or experience worsening symptoms should also be referred to a specialist, such as a dermatologist or an ophthalmologist. Early referral to these specialists is particularly important in cases of ocular involvement or suspected rhinophyma, given the risk of complications.
Collaboration among physicians, physician assistants, nurses, pharmacists, and pharmacy personnel strengthens diagnostic accuracy, optimizes pharmacotherapy, improves adherence, and supports comprehensive patient-centered management.
Clinical Pearls for the Care Team
|
|---|
Summary
Rosacea is a chronic, relapsing inflammatory dermatosis characterized by persistent erythema, telangiectasias, papules, pustules, phymatous changes, and ocular involvement. Contemporary understanding recognizes rosacea as a phenotype-based condition driven by immune dysregulation, vascular hyperreactivity, microbial influences, neurogenic inflammation, genetic susceptibility, and environmental triggers. The condition affects millions worldwide and occurs across diverse ethnic groups and skin phototypes. Although not life-threatening, rosacea can substantially impair quality of life because of its visible facial manifestations and chronic course.
Diagnosis is clinical and requires careful assessment of dominant features and disease severity. Recognition of overlapping phenotypes is essential for guiding therapy and determining when specialty referral is appropriate, particularly in cases of phymatous or ocular involvement.
Management requires a structured, individualized, and multimodal approach. An interprofessional approach enhances diagnostic precision, optimizes pharmacologic therapy, supports adherence, and addresses psychosocial burden. Through collaborative care and patient engagement, healthcare teams can improve long-term outcomes and quality of life for individuals living with rosacea.
References
Sharma A, Kroumpouzos G, Kassir M, et al. Rosacea management: A comprehensive review. J Cosmet Dermatol. 2022;21(5):1895-1904. doi:10.1111/jocd.14816
Del Rosso JQ, Thiboutot D, Gallo R, et al. Consensus recommendations from the American Acne & Rosacea Society on the management of rosacea. J Clin Aesthet Dermatol. 2013;6(2):18–28.
Maliyar K, Abdulla SJ. Dermatology: how to manage rosacea in skin of colour. Drugs Context. 2022;11:2021-11-1. Published 2022 May 31. doi:10.7573/dic.2021-11-1
Gallo RL, Granstein RD, Kang S, et al. Standard classification and pathophysiology of rosacea: The 2017 update by the National Rosacea Society Expert Committee. J Am Acad Dermatol. 2018;78(1):148–155. doi:10.1016/j.jaad.2017.08.017
Sangha AM. Diagnosing and Treating Rosacea in Skin of Color Patients. J Clin Aesthet Dermatol. 2023;16(12 Suppl 2):S14-S15.
DermNet. Rosacea. dermnetnz.org. Updated September 2024. Accessed February 23, 2026. https://dermnetnz.org/topics/rosacea
National Rosacea Society. New Study Estimates Rosacea’s Worldwide Prevalence. Rosacea.org. Published May 23, 2024. Accessed February 23, 2026. https://www.rosacea.org/blog/2024/may/new-study-estimates-rosaceas-worldwide-prevalence
Tan J, Schöfer H, Araviiskaia E, et al. Prevalence of rosacea in the general population of Germany and Russia - The RISE study. J Eur Acad Dermatol Venereol. 2016;30(3):428-434. doi:10.1111/jdv.13556
Rainer BM, Kang S, Chien AL. Rosacea: Epidemiology, pathogenesis, and treatment. Dermatoendocrinol. 2017;9(1):e1361574. Published 2017 Oct 4. doi:10.1080/19381980.2017.1361574
Chen C, Wang P, Zhang L, et al. Exploring the Pathogenesis and Mechanism-Targeted Treatments of Rosacea: Previous Understanding and Updates. Biomedicines. 2023;11(8):2153. Published 2023 Jul 31. doi:10.3390/biomedicines11082153
Yamasaki K, Di Nardo A, Bardan A, et al. Increased serine protease activity and cathelicidin promotes skin inflammation in rosacea. Nat Med. 2007;13(8):975-980. doi:10.1038/nm1616
Steinhoff M, Schauber J, Leyden JJ. New insights into rosacea pathophysiology: a review of recent findings. J Am Acad Dermatol. 2013;69(6 Suppl 1):S15-S26. doi:10.1016/j.jaad.2013.04.045
Buhl T, Sulk M, Nowak P, et al. Molecular and Morphological Characterization of Inflammatory Infiltrate in Rosacea Reveals Activation of Th1/Th17 Pathways. J Invest Dermatol. 2015;135(9):2198-2208. doi:10.1038/jid.2015.141
Paichitrojjana A. Demodex: The worst enemies are the ones that used to be friends. Dermatol Reports. 2022;14(3):9339. Published 2022 Mar 23. doi:10.4081/dr.2022.9339
Schwab VD, Sulk M, Seeliger S, et al. Neurovascular and neuroimmune aspects in the pathophysiology of rosacea. J Investig Dermatol Symp Proc. 2011;15(1):53-62. doi:10.1038/jidsymp.2011.6
Chang ALS, Raber I, Xu J, et al. Assessment of the genetic basis of rosacea by genome-wide association study. J Invest Dermatol. 2015;135(6):1548–1555. doi:10.1038/jid.2015.53.
Wilkin J, Dahl M, Detmar M, et al. Standard grading system for rosacea: report of the National Rosacea Society Expert Committee. J Am Acad Dermatol. 2004;50(6):907–912. doi:10.1016/j.jaad.2004.01.048
Hall JM, Cruser D, Podawiltz A, Mummert DI, Jones H, Mummert ME. Psychological Stress and the Cutaneous Immune Response: Roles of the HPA Axis and the Sympathetic Nervous System in Atopic Dermatitis and Psoriasis. Dermatol Res Pract. 2012;2012:403908. doi:10.1155/2012/403908
Maden S. Rosacea: An overview of its etiological factors, pathogenesis, classification and therapy options. Dermato. 2023;3(4):241-262. doi:10.3390/dermato3040019
Damiani G, Gironi LC, Grada A, et al. COVID-19 related masks increase severity of both acne (maskne) and rosacea (mask rosacea): Multi-center, real-life, telemedical, and observational prospective study. Dermatol Ther. 2021;34(2):e14848. doi:10.1111/dth.14848
van Zuuren EJ. Rosacea. N Engl J Med. 2017;377(18):1754-1764. doi:10.1056/NEJMcp1506630
Mayo Clinic Staff. Ocular rosacea: Symptoms & causes. MayoClinic.org. Updated April 6, 2024. Accessed February 23, 2026. https://www.mayoclinic.org/diseases-conditions/ocular-rosacea/symptoms-causes/syc-20375798
Mohamed-Noriega K, Loya-Garcia D, Vera-Duarte GR, et al. Ocular Rosacea: An Updated Review. Cornea. 2025;44(4):525-537. doi:10.1097/ICO.0000000000003785
King S, Campbell J, Rowe R, Daly M-L, Moncrieff G, Maybury C. A systematic review to evaluate the efficacy of azelaic acid in the management of acne, rosacea, melasma and skin aging. J Cosmet Dermatol. 2023;22(10):2650-2662. doi:10.1111/jocd.15923.
van Zuuren EJ, Fedorowicz Z, Carter B, Charland L. Interventions for rosacea. Cochrane Database Syst Rev. 2015;(4):CD003262. doi:10.1002/14651858.CD003262.pub5
Draelos ZD, Gold MH, Weiss RA, et al. Efficacy and safety of oxymetazoline cream 1.0% for treatment of persistent facial erythema associated with rosacea: results from two phase 3 randomized clinical trials. J Am Acad Dermatol. 2018;78(3):591-600. doi:10.1016/j.jaad.2017.10.041
Taieb A, Ortonne JP, Ruzicka T, et al. Superiority of ivermectin 1% cream over metronidazole 0.75% cream in treating inflammatory lesions of rosacea: a randomized investigator-blinded trial. Br J Dermatol. 2015;172(4):1103-1110. doi:10.1111/bjd.13454
Zhang H, Yang L, Wang Y, Zhang D, Tang K, Fang R, Sun Q. Topical calcineurin inhibitors as a double-edged sword in rosacea: a systematic review. J Cosmet Dermatol. 2021;20(12):3772-3780. doi:10.1111/jocd.14315
Fowler J Jr, Jarratt M, Moore A, et al. Once-daily topical brimonidine tartrate gel 0.33% is safe and effective for moderate to severe facial erythema of rosacea: results of two randomized, double-blind, vehicle-controlled studies. J Drugs Dermatol. 2012;11(6):631-638.
Del Rosso JQ, Webster GF, Jackson M, et al. Two randomized phase III clinical trials evaluating anti-inflammatory dose doxycycline (40-mg doxycycline, USP capsules) administered once daily for treatment of rosacea. J Am Acad Dermatol. 2007;56(5):791-802. doi:10.1016/j.jaad.2007.01.020
Clark SM, Lanigan SW. Treatment of rosacea-associated telangiectasia with the potassium titanyl phosphate laser. Br J Dermatol. 2000;142(6):1179-1182. doi:10.1046/j.1365-2133.2000.03489.x
Goldberg DJ, Cutler KB. Nd:YAG laser treatment of facial telangiectasias. Dermatol Surg. 2000;26(2):139-142.
Har-El G, Shapshay SM. The treatment of rhinophyma with the carbon dioxide laser. Arch Otolaryngol Head Neck Surg. 1993;119(6):628-631. doi:10.1001/archotol.1993.01880180042009
Madorsky SJ, et al. Erbium:YAG laser resurfacing for rhinophyma. Dermatol Surg. 2000;26(4):331-336.
Ramos-e-Silva M, da Silva Carneiro SC. Surgical treatment of rhinophyma: excision, dermabrasion, laser and radiofrequency techniques. Clin Dermatol. 2004;22(3):242-246. doi:10.1016/j.clindermatol.2003.12.018
Draelos ZD. The effect of cleansing systems on the skin barrier. Clin Dermatol. 2012;30(3):318-322. doi:10.1016/j.clindermatol.2011.08.021
Lodén M. Role of topical emollients and moisturizers in the treatment of dry skin barrier disorders. Am J Clin Dermatol. 2003;4(11):771-788. doi:10.2165/00128071-200304110-00005
Two AM, Wu W, Gallo RL, Hata TR. Rosacea: part I. Introduction, categorization, histology, pathogenesis, and risk factors. J Am Acad Dermatol. 2015;72(5):749-758. doi:10.1016/j.jaad.2014.08.028
Dayan SH, Arkins JP, Brindise R. Botulinum toxin A for the treatment of facial flushing and erythema. Dermatol Surg. 2012;38(5):733-739. doi:10.1111/j.1524-4725.2011.02279
DailyMed. Azelaic acid gel, 15%. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Metronidazole topical (gel, cream, lotion) 0.75% and 1%. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Ivermectin cream, 1%. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Sodium sulfacetamide 10% and sulfur 5% topical preparations. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Brimonidine tartrate gel 0.33%. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Oxymetazoline hydrochloride cream 1%. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Doxycycline (40 mg modified-release capsules). US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Doxycycline hyclate tablets and capsules (50 mg, 100 mg). US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Minocycline hydrochloride capsules. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Minocycline topical foam 1.5%. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Azithromycin tablets. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Isotretinoin capsules. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Tacrolimus ointment 0.03% and 0.1%. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Pimecrolimus cream 1%. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Artificial tears ophthalmic solution. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Cyclosporine ophthalmic emulsion 0.05%. US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
DailyMed. Benzoyl peroxide topical preparations (5%). US National Library of Medicine. Updated periodically. Accessed February 23, 2026. https://dailymed.nlm.nih.gov/dailymed/
Akpek EK, Merchant A, Pinar V, Foster CS. Ocular rosacea: patient characteristics and follow-up. Ophthalmology. 1997;104(11):1863-1867. doi:10.1016/S0161-6420(97)30077-6
Lin A, Ahmad S, Amescua G, et al. Blepharitis Preferred Practice Pattern®. Ophthalmology. 2024;131(4):P50-P86. doi:10.1016/j.ophtha.2023.12.036
Nekui F, Galbraith AA, Briesacher BA, et al. Cost-related Medication Nonadherence and Its Risk Factors Among Medicare Beneficiaries. Med Care. 2021;59(1):13-21. doi:10.1097/MLR.0000000000001458
DISCLAIMER
The information provided in this course is general in nature, and it is designed solely to provide participants with continuing education credit(s). This course and materials are not meant to substitute for the independent, professional judgment of any participant regarding that participant’s professional practice, including but not limited to patient assessment, diagnosis, treatment, and/or health management. Medical and pharmacy practices, rules, and laws vary from state to state, and this course does not cover the laws of each state; therefore, participants must consult the laws of their state as they relate to their professional practice.
Healthcare professionals must consult their employer, healthcare facility, hospital, or other organization for guidelines, protocols, and procedures to follow. The information provided in this course does not replace those guidelines, protocols, and procedures, but is for academic purposes only, and this course’s limited purpose is for the completion of continuing education credits.
Participants are advised and acknowledge that information related to medications, their administration, dosing, contraindications, adverse reactions, interactions, warnings, precautions, or accepted uses is constantly changing. Any person taking this course understands that such a person must make an independent review of medication information before any patient assessment, diagnosis, treatment and/or health management. Any discussion of off-label use of any medication, device, or procedure is informational only, and such uses are not endorsed hereby.
Nothing contained in this course represents the opinions, views, judgments, or conclusions of RxCe.com LLC. RxCe.com LLC is not liable or responsible to any person for any inaccuracy, error, or omission with respect to this course or course material.
© RxCe.com LLC 2026: All rights reserved. No reproduction of all or part of any content herein is allowed without the prior, written permission of RxCe.com LLC.
RxCe.com
© RxCe.com LLC 2025: All rights reserved.

