CONTEMPORARY MANAGEMENT STRATEGIES FOR ATOPIC DERMATITIS
Faculty:
L. Austin Fredrickson, MD, FACP
L. Austin Fredrickson is an Associate Professor of Internal Medicine at Northeast Ohio Medical University, where he serves as core faculty and teaches diagnostics, therapeutics, clinical skills, and health humanities. He is board-certified in general internal medicine and practices rural primary care.
Liz Fredrickson, PharmD, BCPS, is an Associate Professor of Pharmacy Practice and Pharmaceutical Sciences at the Northeast Ohio Medical University (NEOMED) College of Pharmacy. She has eight years of experience in medical writing and research.
Pamela Sardo, PharmD, BS
Pamela Sardo, PharmD, BS, is a freelance medical writer and licensed pharmacist. She is the founder and principal at Sardo Solutions in Texas. Pam received her BS from the University of Connecticut and her PharmD from the University of Rhode Island. Pam’s career spans many years in retail, clinics, hospitals, long-term care, Veterans Affairs, and managed health care responsibilities across a broad range of therapeutic classes and disease states.
Abstract
Atopic dermatitis (AD), also known as atopic eczema, is a chronic, relapsing inflammatory skin disorder characterized by intense pruritus, xerosis (dry skin), and eczematous lesions. It was historically considered a disease of childhood, but more recent data suggest that AD frequently persists into adulthood and may also present as a new condition in adult patients. Advances in understanding the immunopathogenesis of AD have transformed the therapeutic landscape, and the introduction of biologic therapies and oral Janus kinase (JAK) inhibitors has prompted substantial updates in national and international treatment guidelines. This continuing education activity reviews the etiology, epidemiology, and pathophysiology of AD. Additionally, common clinical presentations, diagnostic strategies, and interprofessional management plans aligned with current evidence-based recommendations will be discussed.
Accreditation Statements
In support of improving patient care, RxCe.com LLC is jointly accredited by the Accreditation CouncilTM for Continuing Medical Education (ACCME®), the Accreditation Council for Pharmacy Education (ACPE®), and the American Nurses Credentialing Center (ANCC®), to provide continuing education for the healthcare team.

This activity was planned by and for the healthcare team, and learners will receive 2 Interprofessional Continuing Education (IPCE) credits for learning and change.
Credits: 2 contact hour(s) (0.2 CEU(s)) of continuing education credit.
Credit Types:
IPCE Credits - 2 Credits
AAPA Category 1 Credit™️ - 2 Credits
AMA PRA Category 1 Credit™️ - 2 Credits
Type of Activity: Application
Media: Computer-Based Training (i.e., online courses)
Estimated time to complete activity: 2 contact hour(s) (0.2 CEU(s)), including Course Test and course evaluation.
Release Date: April 10, 2026 Expiration Date: April 10, 2029
Target Audience: This educational activity is for Physicians and Physician Assistants
How to Earn Credit: From April 10, 2026, through April 10, 2029, participants must:
Read the “learning objectives” and “author and planning team disclosures;”
Study the section entitled “Educational Activity;” and
Complete the Course Test and Evaluation form. The Course Test will be graded automatically. Following successful completion of the Course Test with a score of 70% or higher, a statement of participation will be made available immediately. (No partial credit will be given.)
CME Credit: Credit for this course will be uploaded to CPE Monitor® for pharmacists. Physicians may receive AMA PRA Category 1 Credit™️and use these credits toward Maintenance of Certification (MOC) requirements. Physician Assistants may earn AAPA Category 1 CME credit, reportable through PA Portfolio. All learners shall verify their individual licensing board’s specific requirements and eligibility criteria.
Statement of Need
Atopic dermatitis is a prevalent chronic inflammatory skin disease affecting millions of patients. It remains frequently underdiagnosed, misclassified, and inadequately controlled. Healthcare professionals may rely on body surface area to assess severity, overlooking significant quality-of-life impairments, including sleep disruption, pruritus, and psychosocial burden. Treatment selection is often inconsistent, sometimes overused, delayed, or made without full consideration of the mechanism of action, safety profiles, routes of administration, or patient-specific factors. Gaps remain in recognizing dosage forms, counseling on proper application, and optimizing the interprofessional approach to care. This activity aims to optimize classification accuracy, severity assessment, and patient-centered action plans to improve long-term disease control and adherence.
Learning Objectives: Upon completion of this educational activity, participants should be able to:
Differentiate clinical presentations and severity of atopic dermatitis
Evaluate available treatment options for atopic dermatitis based on disease severity, patient characteristics, and safety considerations
Describe patient-centered management strategies to support long-term disease control, symptom reduction, and quality-of-life improvement
Disclosures
The following individuals were involved in planning, developing, and/or authoring this activity: L. Austin Fredrickson, MD, FACP; Liz Fredrickson, PharmD, BCPS; and Pamela Sardo, PharmD, BS. None of the individuals involved in developing this activity has a conflict of interest or financial relationships related to the subject matter. There are no financial relationships or commercial or financial support relevant to this activity to report or disclose by RxCe.com or any of the individuals involved in the development of this activity.
© RxCe.com LLC 2026: All rights reserved. No reproduction of all or part of any content herein is allowed without the prior, written permission of RxCe.com LLC.
Educational Activity Pre-Test
A 28-year-old patient presents with eczematous lesions involving 6% body surface area. They report severe pruritus with nightly sleep disturbance and a significant impact on work performance. How should this patient’s disease severity be best classified?
Mild
Severe
Cannot determine without a SCORAD score
Moderate
A patient with moderate-to-severe atopic dermatitis has failed optimized topical therapy. Which of the following is considered a first-line systemic option with a favorable safety profile and minimal routine laboratory monitoring?
Cyclosporine
Methotrexate
Dupilumab
Systemic corticosteroids
Which of the following strategies is most effective in reducing flare frequency in patients with atopic dermatitis?
Discontinuing therapy once lesions resolve
Using topical corticosteroids only during severe flares
Proactive intermittent therapy to previously affected areas
Avoiding moisturizers during remission
Educational Activity
Contemporary Management Strategies for Atopic Dermatitis
Introduction
Atopic dermatitis (AD), also known as atopic eczema, is a chronic, relapsing inflammatory skin disorder characterized by intense pruritus, xerosis (dry skin), and eczematous lesions.1,2 It was historically considered a disease of childhood, but more recent data suggest that AD frequently persists into adulthood and may also present as a new condition in adult patients.1,3 This condition is notable for fluctuating severity, periods of remission and exacerbation, and significant impairment in quality of life.1 Atopic dermatitis causes substantial physical and psychosocial burdens, and patients frequently experience sleep disturbance, fatigue, social withdrawal, anxiety, and depression.1,2 Beyond skin involvement, AD is increasingly recognized as part of a systemic atopic phenotype associated with allergic rhinitis, asthma, and food allergies. This is often described as the “atopic march.”2,5
Advances in understanding the immunopathogenesis of AD have transformed the therapeutic landscape, and the introduction of biologic therapies and oral Janus kinase (JAK) inhibitors has prompted substantial updates in national and international treatment guidelines.4,5 This continuing education activity reviews the etiology, epidemiology, and pathophysiology of AD. Additionally, common clinical presentations, diagnostic strategies, and interprofessional management plans aligned with current evidence-based recommendations will be discussed.
Guideline Updates
There have been recent, important updates in AD management guidelines from the American Academy of Dermatology (AAD) and the American Academy of Allergy, Asthma and Immunology/American College of Allergy, Asthma and Immunology (AAAAI/ACAAI) Joint Task Force.3 These updates reflect the use of targeted biologics and small-molecule therapies and, importantly, emphasize shared decision-making, disease severity stratification, and long-term disease control.3 Key revisions include the following.3
Strong recommendations for dupilumab and tralokinumab in moderate-to-severe AD refractory to topical therapy
Strong or conditional recommendations for oral JAK inhibitors (abrocitinib, baricitinib, upadacitinib) in selected patients after risk assessment
Conditional recommendations for traditional systemic immunomodulators such as cyclosporine, methotrexate, azathioprine, and mycophenolate
Recommendations against routine use of systemic corticosteroids for chronic management
Emphasis on proactive maintenance therapy with topical corticosteroids (TCS) or topical calcineurin inhibitors (TCIs) to prevent flares
Clarification that prescription moisturizers offer no clear advantage over well-formulated over-the-counter moisturizers
Conditional use of dilute bleach baths in moderate-to-severe disease
Recommendation against routine elimination diets in the absence of confirmed food allergy
Additionally, the guidelines now emphasize addressing therapeutic inertia, or the failure to escalate therapy when indicated, which has historically contributed to the undertreatment of moderate-to-severe AD.3
Epidemiology of Atopic Dermatitis
Atopic dermatitis affects approximately 20% of children and 10% of adults globally.1,3 In the United States (US), the prevalence is estimated at 18% among school-aged children and approximately 7% among adults.1 While many cases begin in infancy, up to 25% of adults with AD report adult-onset disease.1 AD follows a bimodal age distribution, with peaks in early childhood and middle adulthood.1 Although it has been suggested that most children “outgrow” AD, more recent systematic reviews have found that many individuals experience persistent or recurrent disease into adulthood.1 The disease severity distribution in adults has been reported as follows.1
Mild: ~50%
Moderate: ~40%
Severe: <10% =
Atopic dermatitis is among the leading causes of disability-adjusted life-years (DALYs) for skin diseases worldwide.1 It is associated with a significant economic burden. Direct and indirect costs include physician visits, prescription medications, lost productivity, and out-of-pocket expenses. In severe cases, disease-related costs may account for a substantial proportion of a patient’s household income.1
Etiology, Risk Factors, and Pathophysiology
Atopic dermatitis is a multifactorial disorder that results from an interplay between genetic predisposition, epidermal barrier dysfunction, immune dysregulation, and environmental exposures.1,2,6
Genetic Factors
The strongest known genetic risk factor is a mutation in the filaggrin (FLG) gene, which encodes a structural protein essential for epidermal barrier integrity.2 Filaggrin deficiency leads to the following:2
Reduced ceramide production
Increased transepidermal water loss
Enhanced penetration of allergens and microbes
FLG mutations alone are not sufficient to cause AD. Multiple other genes involved in skin barrier function and immune regulation also contribute to susceptibility.2
Immune Dysregulation
AD is primarily driven by type 2 inflammation.1 In acute lesions, keratinocytes release IL-25, IL-33, and thymic stromal lymphopoietin (TSLP), which activate dendritic cells and promote differentiation of naïve T cells into Th2 cells.1 Th2 cells produce IL-4, IL-5, IL-13, and IL-31, leading to the following:1
Impaired keratinocyte differentiation
Increased IgE production
Eosinophil activation
Intense pruritus
IL-13 appears to be a dominant cytokine in AD and correlates with disease severity.1,6 Chronic disease demonstrates a broader immune profile, with involvement of Th1, Th17, and Th22 pathways contributing to epidermal thickening and lichenification.1,6
Microbiome Alterations
Patients with AD tend to exhibit reduced microbial diversity and increased colonization with Staphylococcus aureus.1,2 This is present in up to 90% of patients.1 Reduced antimicrobial peptides further predispose patients to infection.1,2s
Environmental and Lifestyle Triggers
Several environmental and lifestyle factors can exacerbate AD.3 These include the following:3
Irritants (harsh soaps, detergents)
Temperature changes
Psychological stress
Skin infections
Food allergens in selected pediatric populations
Clinical Presentation and Diagnosis
Atopic dermatitis is a clinical diagnosis based on characteristic morphology, distribution, chronicity, and associated symptoms, most notably pruritus. There is no single diagnostic laboratory test for this condition.1,3 Instead, it is defined by a relapsing course, xerosis, and patterns of eczematous inflammation that vary by patient age.1,3 Classic diagnostic frameworks include the Hanifin and Rajka criteria and other, simplified guidelines that emphasize essential features such as pruritus, chronic or relapsing dermatitis, and typical distribution patterns.3,8 However, clinicians generally rely on clinical recognition rather than strict scoring systems.
Key Clinical Features
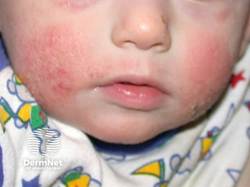
Pruritus is the hallmark of AD and often will occur before visible inflammation. Lesions are typically ill-defined, erythematous patches and plaques with excoriations and lichenification in chronic disease (Figure 1).1,11 Acute flares may include vesicles, oozing, and crusting, whereas chronic disease is characterized by thickened skin with accentuated skin markings.2,3 Xerosis occurs in almost all cases and reflects impaired barrier function.2,3
Figure 110
Distribution varies by age as follows.
Infants: Cheeks, scalp, trunk, and extensor surfaces10
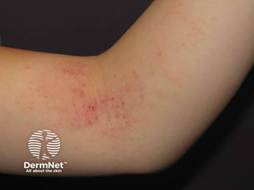
Figure 2
Children: Flexural surfaces (antecubital and popliteal fossae), wrists, ankles, neck10
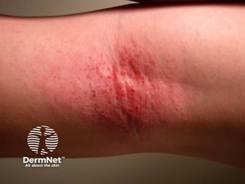
Figure 3
Adolescents and adults: Flexural areas, hands, eyelids, neck, and sometimes head and neck predominance10
Hand dermatitis, nipple dermatitis, and eyelid involvement are common in adults. Chronic scratching can result in prurigo nodularis–like lesions.10
Clinical recognition of atopic dermatitis in patients with darker skin tones (Fitzpatrick types IV–VI) is essential for preventing underdiagnosis and chronic undertreatment.8,11 In these populations, the classic bright "red" erythema seen in lighter skin often appears as violaceous, grayish-brown, or deep purple patches.8,11 There is also a higher prevalence of follicular accentuation and papular AD, particularly on the trunk and extensor surfaces, which can be misdiagnosed if clinicians only look for the classic flexural distribution.8,11 Additionally, patients with darker skin are at significantly higher risk for post-inflammatory hyperpigmentation (PIH), which often causes more psychological distress than the dermatitis itself and requires aggressive early intervention to prevent long-term pigmentary changes.8,11
Severity Assessment
Disease severity should be determined to guide therapeutic intensity and monitor the patient’s response. Clinician-based tools such as the Eczema Area and Severity Index (EASI) and SCORAD (Scoring Atopic Dermatitis) are used in research settings, while simpler global assessments are often used in practice.3,11 Important elements include:11
Body surface area (BSA) involvement
Degree of erythema, edema, excoriation, and lichenification
Frequency of flares
Impact on sleep
Quality-of-life impairment
Patient-reported outcomes are increasingly emphasized, particularly itch severity and sleep disturbance, which correlate strongly with disease burden.1
Table 1
Severity Assessment
| Severity | Clinical Features | Impact on Patient | Typical Management Approach |
| Mild | Limited BSA (<5–10%), mild erythema, minimal lichenification | Minimal sleep disturbance; mild impact on quality of life | Emollients + low- to mid-potency topical corticosteroids (TCS) or topical calcineurin inhibitors (TCIs); proactive maintenance |
| Moderate | More widespread involvement (10–20% BSA), frequent flares, visible inflammation | Moderate itch, sleep disruption, noticeable QoL impairment | Optimized topical therapy, wet wraps, bleach baths; consider phototherapy or escalation to systemic therapy |
| Severe | Extensive BSA (>20%), marked erythema, lichenification, or refractory disease | Severe pruritus, significant sleep loss, major QoL impairment | Systemic therapy (biologics, JAK inhibitors); specialist referral; comprehensive management plan |
| Severity | Clinical Features | Impact on Patient | Typical Management Approach |
| Mild | Limited BSA (<5–10%), mild erythema, minimal lichenification | Minimal sleep disturbance; mild impact on quality of life | Emollients + low- to mid-potency topical corticosteroids (TCS) or topical calcineurin inhibitors (TCIs); proactive maintenance |
Laboratory Evaluation
Routine laboratory testing is not required to diagnose AD.3 However, selected tests may be useful in a specific context.3,11
Serum IgE: often elevated but nonspecific
Peripheral eosinophilia: may be present in moderate-to-severe disease3,9
Allergy testing: considered when food allergy, allergic contact dermatitis, or environmental triggers are suspected3,9
Patch testing: appropriate in refractory disease or when allergic contact dermatitis is suspected
Skin biopsy is rarely necessary but may be considered when the diagnosis is uncertain or when alternative conditions such as cutaneous T-cell lymphoma, psoriasis, seborrheic dermatitis, scabies, or contact dermatitis are suspected.3
Systemic Comorbidities
Chronic systemic inflammation in AD is recognized as an important implicatory for broader health complications. Moderate-to-severe AD is associated with an increased risk of cardiovascular and metabolic comorbidities, including obesity, hypertension, and Type 2 diabetes.1 Chronic inflammation has also been linked to higher rates of osteoporosis and fractures.1 The psychosocial burden is equally severe, and there is a strong correlation with suicidal ideation, depression, and anxiety, necessitating that clinicians move beyond skin assessment to include routine mental health and metabolic screening in their long-term management plans.11
Differential Diagnosis and Evaluation of Comorbidities
The differential diagnosis varies by age and distribution and includes the following.3
Contact dermatitis (allergic or irritant)
Seborrheic dermatitis
Psoriasis
Scabies
Nummular dermatitis
Cutaneous T-cell lymphoma (particularly in adults with refractory disease)
In infants, distinguishing AD from seborrheic dermatitis is important.3 Seborrheic dermatitis typically lacks significant pruritus and involves the scalp and diaper region.3
Atopic dermatitis is also associated with other atopic conditions, including asthma and allergic rhinitis (the “atopic march”).1,2 Aside from physical symptoms, the systemic nature of AD requires a holistic approach to patient care. Screening for sleep disturbance, anxiety, depression, and reduced quality of life is recommended, particularly in cases of moderate-to-severe disease.1,11
Management Overview
The management of AD requires a stepwise, severity-based approach with emphasis on long-term disease control and prevention of flares. The primary goals of atopic dermatitis treatment are to reduce inflammation, relieve pruritus, restore and maintain skin barrier function, prevent flares, and minimize treatment-related adverse effects.3,4 Because atopic dermatitis is a chronic, relapsing condition, management focuses not only on acute symptom control but also on long-term disease stabilization.5,11 Effective treatment also aims to reduce sleep disturbance, improve quality of life, and address psychosocial burden.4,6 In moderate-to-severe disease, systemic or biologic therapies may be necessary to achieve adequate disease control while minimizing cumulative steroid exposure.4,6
The guidelines recommend addressing several foundational elements before escalating therapy, including the following:5
Confirm diagnosis and rule out mimickers
Provide patient education and a written action plan
Identify and minimize triggers
Ensure correct medication use
Encourage consistent moisturization
Atopic dermatitis therapies are available in multiple dosage forms to support individualized treatment selection and patient preference. These include topical formulations such as creams, ointments, lotions, foams, and solutions; oral tablets or capsules for systemic therapies; and subcutaneous injectable biologics. Selection of the appropriate dosage form can significantly influence adherence, tolerability, and treatment success.
Pause and Ponder A 32-year-old patient reports eczema affecting 6% of body surface area but experiences nightly sleep disruption and significant work impairment. Based solely on body surface area, the disease might appear mild. However, when symptom burden and quality-of-life impact are considered, how would you classify this disease severity? Should systemic therapy be considered? |
Treatment Strategies
Topical Therapies
Regular use of moisturizers is essential for all patients with atopic dermatitis, regardless of disease severity.3,4 Emollients should be applied at least twice daily and immediately after bathing to reduce transepidermal water loss and improve barrier function.3 Ointment-based formulations (such as petrolatum-based products) provide greater occlusion and are generally more effective for severe xerosis. However, some patients prefer creams or lotions for cosmetic acceptability and daytime use.3,4 Fragrance-free, dye-free products are preferred to reduce irritation risk. Patients should be counseled that the “best” moisturizer is the one they will use consistently and adequately.3
Topical Corticosteroids (TCS)
Topical corticosteroids are the first-line anti-inflammatory therapy for acute flares.4,5 Potency selection should be guided by several factors, including patient age, body site, and disease severity.4,5 Low-potency agents ( hydrocortisone 1%–2.5%) are preferred for the face, eyelids, neck, and intertriginous areas.4,5 Medium-potency agents (triamcinolone acetonide 0.1%) are commonly used for trunk and extremities.4,5 High-potency agents (clobetasol propionate 0.05%) may be used for thick, lichenified plaques on non-facial areas for short durations, with a typical limit of 1–2 weeks.4,5
Typically, applying these products once a day is sufficient and may improve adherence without reducing efficacy.4,5 Proactive therapy, which involves intermittent application (twice weekly) to previously affected areas after disease control, has been shown to reduce flare frequency.4,5 Adverse effects include skin atrophy, striae, telangiectasias, perioral dermatitis, and, rarely, hypothalamic–pituitary–adrenal axis suppression with extensive or prolonged high-potency use.4,5 Caution is warranted in pediatric patients due to higher surface-area-to-body-weight ratios.4,5
Topical corticosteroid withdrawal, sometimes referred to as “red skin syndrome,” is a controversial and incompletely understood phenomenon noted by erythema, burning, and rebound inflammation after prolonged, inappropriate use of medium- to high-potency topical corticosteroids.4,9 While uncommon, widespread discussion on social media has led to increased patient concerns and may contribute to avoidance of appropriate therapies.1,4 Current evidence suggests that most patients can use topical corticosteroids safely when prescribed at appropriate potency, duration, and anatomical site.4 Clinicians should provide balanced counseling, reinforce safe use practices, avoid prolonged continuous high-potency steroid exposure on sensitive areas, and monitor for signs of misuse. An evidence-informed approach helps prevent both overtreatment and undertreatment.3,5
Topical Calcineurin Inhibitors (TCIs)
Tacrolimus 0.1% for adults and pimecrolimus 1% cream are steroid-sparing agents appropriate for sensitive areas such as the face, eyelids, and intertriginous regions.4,9 They may be applied twice daily during active disease and used intermittently for maintenance therapy. The most common adverse effect is transient burning or stinging at the application site, particularly during early treatment.3 Although boxed warnings regarding theoretical malignancy risk exist, long-term safety data and large observational studies have not demonstrated a causal association when used as directed.4,9 TCIs do not cause skin atrophy and are suitable for long-term use in appropriate patients.3,5
Topical PDE-4 Inhibitor
Crisaborole 2% ointment is indicated for mild-to-moderate atopic dermatitis in patients aged 3 months and older.3 It is applied twice daily to affected areas. Clinical trials have demonstrated modest reductions in inflammation and pruritus.4 The most common adverse effect is application-site burning or stinging, which is typically mild and transient.4,6 It may be particularly useful in patients who want to avoid corticosteroids.4
Topical JAK Inhibitors
Topical ruxolitinib 1.5% cream is approved for short-term, noncontinuous treatment of mild-to-moderate atopic dermatitis in non-immunocompromised patients aged 12 years and older with limited body surface area involvement (typically ≤20%).4,11 It is applied twice daily, and rapid itch reduction is a notable benefit. However, as a Janus kinase inhibitor, it carries boxed warnings for serious infections, malignancy, major adverse cardiovascular events, and thrombosis, although systemic exposure is lower than with oral formulations.4 It should not be used in combination with biologics, systemic JAK inhibitors, or potent immunosuppressants. Current guidelines suggest reserving topical JAK inhibitors for appropriate candidates rather than routine early use.4,5
Adjunctive Measures
Wet wrap therapy can be effective during moderate-to-severe flares, particularly in pediatric populations.3,4 It enhances topical medication penetration and improves hydration, but should be supervised to avoid infection risk.3,4
Dilute bleach baths (typically 0.005% sodium hypochlorite solution, e.g., ¼–½ cup household bleach in a full bathtub of water twice weekly) may reduce Staphylococcus aureus colonization in moderate-to-severe disease.3 When recommending these for moderate-to-severe disease, clinicians must provide precise instructions to avoid the risk of chemical burns or sub-therapeutic dosing.3 Patients should soak for exactly 10 minutes, no more than twice weekly, and must rinse their skin thoroughly with fresh water afterward.3 To maximize the benefit, the "Soak and Seal" method should be followed immediately, applying a thick emollient while the skin is still damp to lock in hydration and maintain the barrier.3
Routine use of topical or systemic antimicrobials is not recommended unless clinical infection is present.4,5 While sedating antihistamines are sometimes used short-term to improve sleep quality by addressing nocturnal scratching, patients should be counseled that they do not directly treat the underlying skin inflammation.1,3
Systemic Therapies
Systemic therapy is indicated for moderate-to-severe atopic dermatitis that is inadequately controlled with optimized topical regimens and adjunctive measures.
Biologic Therapies
Dupilumab, an IL-4 receptor alpha antagonist that inhibits IL-4 and IL-13 signaling, is approved for moderate-to-severe atopic dermatitis in adults and children (age-dependent approvals).4,6 Typical adult dosing is a 600 mg loading dose followed by 300 mg subcutaneously every two weeks.1,6 It significantly improves EASI scores, pruritus, and quality-of-life measures.1,6
Tralokinumab, an IL-13 inhibitor, is administered as a 600 mg loading dose followed by 300 mg every two weeks.4,5 Common adverse effects of biologics include injection-site reactions and conjunctivitis. Routine laboratory monitoring is generally not required.4 Live vaccines should be avoided during therapy.4,5
Oral JAK Inhibitors
Abrocitinib (100–200 mg daily), upadacitinib (15–30 mg daily), and baricitinib (dose varies) provide rapid itch reduction and notable clinical improvement.4,11 They are generally reserved for moderate-to-severe disease following shared decision-making and careful risk assessment.4 Boxed warnings include risks of serious infection (including herpes zoster), malignancy, thrombosis, and major cardiovascular events.4,6 Baseline and periodic laboratory monitoring (CBC, liver enzymes, lipids) is recommended.4 They should be avoided in patients with significant cardiovascular risk factors or prior thromboembolic events unless the benefits outweigh risks.4,5
Traditional Immunosuppressants
Cyclosporine (typically 3–5 mg/kg/day divided doses) may be used as short-term rescue therapy in severe refractory disease, with monitoring for nephrotoxicity and hypertension.5,6 Methotrexate (10–25 mg weekly), azathioprine (1–3 mg/kg/day), and mycophenolate mofetil are conditionally recommended off-label options requiring laboratory monitoring for hematologic and hepatic toxicity.4,5 Systemic corticosteroids are discouraged for long-term management due to rebound flares and significant adverse effects. However, brief courses may be used in select acute circumstances.3,5
Emerging Biologic Therapies: Lebrikizumab and Nemolizumab
Lebrikizumab is a monoclonal antibody that selectively targets interleukin-13 (IL-13), which is a central cytokine in the Th2 inflammatory pathway of atopic dermatitis.11 This agent has demonstrated significant improvements in pruritus reduction and quality-of-life measures in patients with moderate-to-severe disease.4,11 Its mechanism is similar to tralokinumab; however, it binds IL-13 with high affinity and prevents receptor complex formation.4 Lebrikizumab is administered via subcutaneous (SQ) injection following a loading dose, then maintenance dosing every two to four weeks, depending on clinical response.11 Adverse effects are generally mild and include injection-site reactions and conjunctivitis.11 Routine laboratory monitoring is not typically required.11
Nemolizumab is a monoclonal antibody targeting the interleukin-31 (IL-31) receptor A, a pathway strongly associated with pruritus signaling.11 Clinical trials have demonstrated both rapid and meaningful reductions in pruritus scores along with improvements in skin inflammation.1,11 Nemolizumab is administered subcutaneously at intervals determined by labeling and patient response.4 Common adverse effects include injection-site reactions and mild upper respiratory symptoms.4
Table 2
Comparing Biologics to Other Therapies
| Feature | Biologics (e.g., dupilumab, tralokinumab) | Oral JAK Inhibitors (e.g., upadacitinib, abrocitinib) | Traditional Systemics (e.g., cyclosporine, methotrexate) |
| Mechanism | Targeted cytokine inhibition (IL-4, IL-13) | Broad intracellular signaling inhibition (JAK pathways) | Broad immunosuppression |
| Onset of Action | Moderate (weeks) | Rapid (days to weeks) | Variable |
| Administration | Subcutaneous injection | Oral | Oral |
| Monitoring | Minimal routine lab monitoring | Requires CBC, LFTs, lipids | Requires frequent lab monitoring |
| Safety Profile | Favorable overall; conjunctivitis common | Boxed warnings (infection, MACE, thrombosis) | Organ toxicity (renal, hepatic), infection risk |
| Best Use | Long-term control, steroid-sparing | Rapid control or refractory disease | Short-term or select refractory cases |
| Adherence Considerations | Injection training required | Daily oral adherence required | Monitoring burden may limit use |
Biologic therapies generally have a favorable safety profile and require minimal routine laboratory monitoring, which may simplify long-term management. In contrast, oral JAK inhibitors provide more rapid symptom relief but require baseline and ongoing laboratory monitoring and carry boxed warnings that necessitate careful patient selection and counseling. Traditional systemic immunosuppressants are effective but are associated with greater toxicity and monitoring burden, making them less desirable for long-term use. Cost, insurance coverage, and access may significantly influence therapy selection, and primary care physicians may collaborate with pharmacists to help balance efficacy, safety, and affordability while supporting adherence.
Safety Considerations
The initiation of advanced systemic therapies, especially Janus kinase (JAK) inhibitors and biologics, requires a standardized screening and preparation protocol to ensure patient safety. For JAK inhibitors such as upadacitinib or abrocitinib, mandatory pre-screening must include a tuberculosis (TB) test, hepatitis B or C serology, a complete blood count (CBC), liver function tests, and a lipid panel.4 In contrast, while biologics like dupilumab require minimal laboratory monitoring, a thorough clinical eye exam is recommended to identify baseline dry eye or keratitis.4 Regardless of therapy, clinicians should ensure that all age-appropriate live vaccines are administered before the commencement of treatment, as live vaccines are generally contraindicated once these systemic immunomodulators are started.4
Before initiating or dispensing advanced systemic therapy, pharmacists should assess:
Infection risk (active infection, history of recurrent infections)
Tuberculosis (TB) and hepatitis B/C screening status (especially for JAK inhibitors)
Baseline laboratory results (CBC, liver function tests, lipid panel)
Drug–drug interactions
Vaccination status (avoid live vaccines during therapy)
Pregnancy status and reproductive considerations
Patient-specific risks (cardiovascular disease, thromboembolism, and malignancy history)
Phototherapy
Narrowband UVB phototherapy is conditionally recommended for moderate-to-severe atopic dermatitis refractory to topical therapy.4,5 Treatments are typically administered two to three times weekly. Phototherapy can reduce inflammation and pruritus but requires consistent attendance and carries cumulative ultraviolet exposure risks, including photoaging and a theoretical increased risk of skin cancer with prolonged use.3,4
Table 3
Medications for the Management of AD3-6
| Therapy class | Examples | Common AEs / cautions | Practical counseling pearls |
| Moisturizers / emollients | OTC ointments/creams (fragrance-free) | Irritation with fragranced products; adherence is main barrier | “Soak and seal”: moisturize within minutes after bathing; keep it simple and consistent |
| Topical corticosteroids (TCS) | Low potency (face/folds), mid–high potency (body flares) | Skin atrophy/striae/telangiectasia risk increases with potency, duration, and thin skin areas | Provide a simple action plan: which steroid, where + how long; fingertip-unit teaching reduces underuse |
| Topical calcineurin inhibitors (TCI) | Tacrolimus (0.03%, 0.1%), pimecrolimus | Transient burning/stinging; historical boxed warning—JTF cites large linked evidence base showing no credible increased cancer risk with typical use | Warn about initial stinging; using after moisturizer and on calmer skin reduces discomfort |
| Topical PDE-4 inhibitor | Crisaborole 2% ointment | Application site burning/stinging | Good for steroid-avoidant patients; cost/coverage often limits use |
| Topical JAK inhibitor | Ruxolitinib cream (where available/appropriate) | Labeling restrictions; infection risk considerations | If used, emphasize limited BSA, duration, and monitoring per labeling |
| Occlusive therapy (“wet wraps”) | Low–mid potency TCS under wet layer | Folliculitis, discomfort; potential increased absorption of TCS | Teach technique; use for a defined, short burst during flares |
| Topical antimicrobials (routine use) | e.g., mupirocin (only if infection) | Resistance; irritation | Frame clearly: treat infection, not baseline inflammation |
| Therapy | Where it fits | Typical dosing (adult) | Monitoring / key risks |
| Narrowband UVB (NB-UVB) | Consider it for refractory disease when topical therapy is insufficient and systemic therapy is undesirable | Usually 2–3x/week for ~10–14 weeks (logistical burden) | Sunburn-like reactions, heat intolerance; long-term skin cancer risk is less concerning than PUVA, but still UV exposure considerations |
| Cyclosporine | Short-term control for moderate–severe AD, especially as a bridge | 3–5 mg/kg/day PO | BP, renal function, drug interactions |
| Methotrexate | Alternative systemic option in selected patients | 10–25 mg weekly PO/SC | CBC, LFTs; teratogenic; folate supplementation |
| Azathioprine | Less favored; select cases only | 2.5–5 mg/kg/day PO; check TPMT before starting | CBC/LFT; infection risk |
| Mycophenolate mofetil | Selected refractory cases | Up to 3000 mg/day divided BID | CBC, infection risk; teratogenic |
| Systemic corticosteroids | Avoid except in rare, exceptional circumstances | Not preferred | Rebound flares, metabolic/bone effects, infection |
Pause and Ponder
When a patient’s atopic dermatitis fails to improve, do you first question the efficacy of the drug or the patient's comfort in using it?
|
|---|
Treatment Algorithm4
Step 0: The "Good Practice" Foundation (All Severities)
Before escalating therapy, primary care physicians must verify these five pillars:
Confirm Diagnosis: Rule out mimickers (Contact dermatitis, Scabies, CTCL).
Education: Provide a written Eczema Action Plan.
Trigger Management: Identify and minimize irritants, heat, and allergens.
Adherence Check: Ensure the patient is using the medications correctly.
Skin Barrier Support: Encourage liberal, daily use of bland moisturizers.
Step 1: Mild AD (Localized, Limited Impact)
Goal: Rapid symptom control and relapse prevention with minimal treatment burden.
Barrier Optimization: "Soak and Seal": Apply moisturizer immediately after bathing.
Active Inflammation: First-line: Topical Corticosteroids (TCS)
Sensitive Areas: Topical Calcineurin Inhibitors (TCI) for face, neck, and folds
Maintenance: "Proactive Therapy": apply TCS or TCI twice weekly to common flare sites.
Alternatives: Consider Crisaborole (PDE-4 inhibitor) for mild-to-moderate disease
Avoid: Routine topical antibiotics unless clinical signs of infection are present.
Step 2: Moderate AD (Widespread or Quality of Life Impairment)
Goal: Gain control quickly, then simplify for long-term adherence.
Optimize Topicals: Move to once-daily application of higher-potency TCS to improve adherence
Crisis Management: Wet Wrap Therapy: Short-term (3–5 days) during acute flares
Dilute Bleach Baths: Use for moderate-to-severe disease to reduce colonization
Advance Therapy (Shared Decision-Making):
Phototherapy (NB-UVB): If feasible and available
Transition to Systemic: When topicals no longer provide adequate control or cause side effects.
Step 3: Moderate-to-Severe / Refractory AD (High Burden)
Goal: Rapid itch reduction, clear skin, and a sustainable long-term systemic plan.
Preferred Advanced Options (Biologics)
Dupilumab (>/6 months old): Strong recommendation from both AAD and JTF.
Tralokinumab (>/12 years old): Strong recommendation for patients refractory to topicals.
Lebrikizumab / Nemolizumab: Consider as newer Th2-targeted or itch-targeted alternatives.
Advanced Options (Oral JAK Inhibitors)
Abrocitinib / Upadacitinib: Reserved for patients requiring rapid control or those who fail biologics.
Safety: Must perform shared risk-benefit assessment regarding MACE, thrombosis, and infection; requires baseline and periodic blood monitoring.
Alternative Systemic & Warnings
Traditional Agents: Conditional use of cyclosporine (short-term), methotrexate, azathioprine, or mycophenolate.
Critical Warning: Avoid systemic corticosteroids for chronic management due to high rebound rates and cumulative toxicity.
Atopic Dermatitis Action Plan4,5
Atopic Dermatitis (Eczema) Action Plan
Patient Name: ____________________ Date: __________
Provider: ____________________
GREEN ZONE: All Clear (Maintenance)
Skin looks: Clear, no redness, no itching, no rough patches.
Your Goal: Keep the skin barrier strong and prevent flares.
Bathing: Lukewarm bath or shower (5–10 minutes) once daily. Use a soap-free, fragrance-free cleanser.
Moisturizing: Apply thick moisturizer (ointment or cream) within 3 minutes of patting skin dry ("Soak and Seal"). Apply at least twice daily.
Proactive Therapy: Apply [Name of Medication] to common flare sites (e.g., inner elbows, behind knees) twice weekly (e.g., Saturdays and Sundays).
YELLOW ZONE: Caution (Flare-Up)
Skin looks: Red, itchy, rough, or bumpy in specific areas.
Your Goal: Stop the inflammation quickly before it spreads.
Continue: All Green Zone bathing and moisturizing steps.
Face/Folds (Sensitive areas): Apply [Low Potency Steroid or TCI] to red/itchy areas twice daily until clear.
Body (Trunk/Arms/Legs): Apply [Medium/High Potency Steroid] to red/itchy areas twice daily.
When to stop: Once the skin is smooth and no longer itchy (usually 1–2 weeks), return to the Green Zone.
RED ZONE: Emergency (Severe Flare or Infection)
Skin looks: Widespread redness, intense itching that prevents sleep, oozing, "honey-colored" crusting, or painful blisters.
Your Goal: Crisis control and medical evaluation.
Advanced Treatment: Apply [Specific High-Potency Medication] as directed.
Wet Wraps: Apply medicated ointment followed by a damp layer of gauze/pajamas and a dry top layer for [X] hours or overnight.
Call the Office if:
Skin is oozing, crusting, or has painful blisters (signs of infection).
No improvement after 48 hours of Yellow Zone treatment.
Fever or chills develop.
Practical Tips for Success4,5
The Fingertip Unit (FTU): One FTU is the amount of cream squeezed from the tip of the finger to the first crease. This covers an area the size of two adult palms.
Quantity Matters: A standard 30g tube should cover the entire adult body roughly once. If you are treating the whole body, ensure you have an adequate supply.
Steroid Safety: When used as directed in the Yellow Zone, topical steroids are safe and effective. Avoid long-term continuous use of high-potency steroids on the face or skin folds without a provider's supervision.
Treatment Adherence and Therapeutic Failure
Treatment failure in atopic dermatitis is frequently related to inadequate adherence rather than true pharmacologic inefficacy. Multiple studies demonstrate that patients often underuse prescribed topical corticosteroids due to fear of adverse effects, a phenomenon commonly referred to as “steroid phobia.”4,11 Concerns about skin thinning, systemic absorption, and long-term harm may lead patients or caregivers to apply insufficient amounts, prematurely shorten treatment duration, or avoid therapy altogether.
In addition, clinicians frequently prescribe inadequate amounts of medication. For example, approximately 30 grams of topical medication are required to cover the entire adult body once.3,5 Clear instructions using fingertip unit guidance can improve proper dosing. Primary prescription nonadherence, or failure to fill prescribed medications, also contributes significantly to poor disease control.3,5 Addressing adherence requires open discussion of safety, realistic risk framing, proactive follow-up, and shared decision-making.4,5 Emphasizing proactive maintenance therapy and setting expectations that atopic dermatitis is a chronic condition requiring ongoing management can reduce therapeutic inertia and improve long-term outcomes.4,5,11
Clinical Counseling Pearls
Atopic dermatitis is a chronic condition requiring ongoing maintenance therapy—even when skin appears clear
Moisturizers are the foundation of treatment and should be used consistently
Apply topical medications before moisturizers unless otherwise directed
Use the fingertip unit (FTU) guidance to ensure adequate dosing
Mild burning or stinging with TCIs or crisaborole is common and often improves with continued use
Biologic therapies may take several weeks for full effect
JAK inhibitors may provide faster itch relief but require closer monitoring
Fear of topical corticosteroids (“steroid phobia”) often leads to undertreatment and poor outcomes
Interprofessional Considerations
Effective management of atopic dermatitis requires coordinated care among healthcare team members. Physicians and advanced practice providers are responsible for establishing the diagnosis, assessing disease severity, initiating and escalating therapy, and monitoring for complications and treatment response. Pharmacists may play a key role in optimizing medication selection, identifying potential drug interactions, providing detailed counseling on proper use and expected outcomes, and addressing adherence barriers. This interprofessional approach improves treatment adherence, enhances patient education, and supports long-term disease control.
Summary
Atopic dermatitis is a chronic inflammatory disease driven by epidermal barrier dysfunction and type 2 immune dysregulation. It affects millions worldwide and significantly impairs the quality of life for many patients. Recent advances in understanding immunopathogenesis have led to targeted biologic and small-molecule therapies that have reshaped treatment paradigms.
Management requires accurate severity assessment, proactive maintenance strategies, patient education, and shared decision-making. Topical therapies remain foundational, but systemic biologics and JAK inhibitors provide effective options for moderate-to-severe disease. Updated guidelines emphasize individualized care, avoidance of therapeutic inertia, and long-term disease control.
Through interprofessional collaboration, including physicians, pharmacists, and pharmacy technicians, patients with atopic dermatitis can achieve meaningful symptom reduction, improved sleep, enhanced quality of life, and sustained disease stability.
References
Langan SM, Irvine AD, Weidinger S. Atopic dermatitis. Lancet. 2020;396(10247):345-360. doi:10.1016/S0140-6736(20)31286-1
Weidinger S, Novak N. Atopic dermatitis. Lancet. 2016;387(10023):1109-1122. doi:10.1016/S0140-6736(15)00149-X
Sidbury R, Alikhan A, Bercovitch L, et al. Guidelines of care for the management of atopic dermatitis in adults with phototherapy and systemic therapies. J Am Acad Dermatol. 2024;90(2):e43-e56. doi:10.1016/j.jaad.2023.08.029
Boguniewicz M, Fonacier L, Guttman-Yassky E, Ong PY, Silverberg JI. Atopic Dermatitis Yardstick update. Ann Allergy Asthma Immunol. 2023;130(6):811-820. doi:10.1016/j.anai.2023.03.010
Wollenberg A, Flohr C, Simon D, et al. European guideline (EuroGuiDerm) on atopic eczema – part I: systemic therapy. J Eur Acad Dermatol Venereol. 2022;36(9):1409-1431. doi:10.1111/jdv.18345
Kim J, Kim BE, Leung DYM. Pathophysiology of atopic dermatitis: Clinical implications. Allergy Asthma Proc. 2019;40(2):84-92. doi:10.2500/aap.2019.40.4202
Drucker AM, Lam M, Prieto-Merino D, et al. Systemic Immunomodulatory Treatments for Atopic Dermatitis: Living Systematic Review and Network Meta-Analysis Update. JAMA Dermatol. 2024;160(9):936-944. doi:10.1001/jamadermatol.2024.2192
Hanifin JM, Rajka G. Diagnostic features of atopic dermatitis. Acta Derm Venereol Suppl (Stockh). 1980;92:44-47.
Silverberg JI. Atopic dermatitis in adults. J Am Acad Dermatol. 2019;80(3):655-668. doi:10.1016/j.jaad.2018.02.001
Stanway A, Jarrett P. Atopic dermatitis [Atopic eczema]. DermNet New Zealand. Updated Feb 2021. Accessed February 24, 2026. https://dermnetnz.org/topics/atopic-dermatitis
Wollenberg A, Christen-Zäch S, Taieb A, et al. ETFAD/EADV Eczema Task Force 2020 position paper on diagnosis and treatment of atopic dermatitis. J Eur Acad Dermatol Venereol. 2020;34(12):2717-2744. doi:10.1111/jdv.16892
DISCLAIMER
The information provided in this course is general in nature, and it is designed solely to provide participants with continuing education credit(s). This course and materials are not meant to substitute for the independent, professional judgment of any participant regarding that participant’s professional practice, including but not limited to patient assessment, diagnosis, treatment, and/or health management. Medical and pharmacy practices, rules, and laws vary from state to state, and this course does not cover the laws of each state; therefore, participants must consult the laws of their state as they relate to their professional practice.
Healthcare professionals must consult their employer, healthcare facility, hospital, or other organization for guidelines, protocols, and procedures to follow. The information provided in this course does not replace those guidelines, protocols, and procedures, but is for academic purposes only, and this course’s limited purpose is for the completion of continuing education credits.
Participants are advised and acknowledge that information related to medications, their administration, dosing, contraindications, adverse reactions, interactions, warnings, precautions, or accepted uses is constantly changing. Any person taking this course understands that such a person must make an independent review of medication information before any patient assessment, diagnosis, treatment and/or health management. Any discussion of off-label use of any medication, device, or procedure is informational only, and such uses are not endorsed hereby.
Nothing contained in this course represents the opinions, views, judgments, or conclusions of RxCe.com LLC. RxCe.com LLC is not liable or responsible to any person for any inaccuracy, error, or omission with respect to this course or course material.
© RxCe.com LLC 2026: All rights reserved. No reproduction of all or part of any content herein is allowed without the prior, written permission of RxCe.com LLC.
RxCe.com
© RxCe.com LLC 2025: All rights reserved.