BURN CARE ESSENTIALS: A MULTIDISCIPLINARY APPROACH TO ASSESSMENT, TREATMENT, AND RECOVERY
Faculty:
Austin Fredrickson, MD, FACP
Austin Fredrickson is an Associate Professor of Internal Medicine at NEOMED and is a board-certified general internal medicine physician.
Liz Fredrickson, PharmD, BCPS
Liz Fredrickson is an Associate Professor of Pharmacy Practice and Pharmaceutical Sciences at the Northeast Ohio Medical University (NEOMED) College of Pharmacy.
Pamela Sardo, PharmD, BS
Pamela Sardo, PharmD, BS, is a freelance medical writer and currently licensed pharmacist in 3 states. She is the founder and principal at Sardo Solutions in Texas. Pam received her BS from the University of Connecticut and her PharmD from the University of Rhode Island. Pam’s career spans many years in retail, clinics, hospitals, long-term care, Veterans Affairs, and managed health care responsibilities across a broad range of therapeutic classes and disease states.
Topic Overview
Burn injuries occur when the skin comes into contact with a damaging agent, including radiation, chemicals, high temperatures, electricity, or friction. Burn injuries are preventable, yet non-fatal burns remain among the leading causes of morbidity and mortality globally. These injuries, ranging from mild to severe, present unique challenges that necessitate a coordinated healthcare team response. The severity of burns is influenced by factors such as the duration and intensity of exposure and the burn's location on the body. This can lead to significant variability in burn-related morbidity and mortality. Prompt and effective treatment is essential to prevent complications and promote optimal healing. The management of burn injuries benefits significantly from the application of the Interprofessional Education Collaborative (IPEC) competencies, which emphasize team-based care and collaboration. This continuing education activity will provide learners with a comprehensive review of the classification, pathophysiology, and management of burn injuries. Special attention will be given to the roles of the multidisciplinary care team, fostering a deeper understanding of how interprofessional collaboration can enhance outcomes in burn care.
Accreditation Statement

RxCe.com LLC is accredited by the Accreditation Council for Pharmacy Education (ACPE) as a provider of continuing pharmacy education.
Universal Activity Number (UAN): The ACPE Universal Activity Number assigned to this activity is
Pharmacist 0669-0000-24-194-H01-P
Pharmacy Technician 0669-0000-24-195-H01-T
Credits: 2 contact hour(s) (0.2 CEU(s)) of continuing education credit
Type of Activity: Knowledge
Media: Internet/Home study Fee Information: $6.99
Estimated time to complete activity: 2 contact hour(s) (0.2 CEU(s)), including Course Test and course evaluation
Release Date: December 31, 2024 Expiration Date: December 31, 2027
Target Audience: This educational activity is for pharmacists and pharmacy technicians.
Secondary Audiences: Other healthcare professionals, such as nurses, physicians, or others who may be part of a healthcare team, may be interested in this educational topic. Healthcare team roles and approaches to patient care are discussed in this activity. No state board, professional organization, or credentialing body has evaluated this activity to determine whether it meets the continuing education requirements of nurses, physicians, or other professions not listed under the “Target Audience” section above. Always verify with individual employers or supervisors whether they will accept this educational activity upon completion.
How to Earn Credit: From December 31, 2024, through December 31, 2027, participants must:
Read the “learning objectives” and “author and planning team disclosures;”
Study the section entitled “Educational Activity;” and
Complete the Course Test and Evaluation form. The Course Test will be graded automatically. Following successful completion of the Course Test with a score of 70% or higher, a statement of participation will be made available immediately. (No partial credit will be given.)
Credit for this course will be uploaded to CPE Monitor®.
Learning Objectives: Upon completion of this educational activity, participants should be able to:
Recall how to classify burn injuries
Compare and Contrast treatment strategies for minor burns
Recall complications of burn injuries
Describe effective communication strategies within the interprofessional healthcare team to ensure collaborative decision- making and coordinated care plans for burn injury management
Disclosures
The following individuals were involved in developing this activity: Liz Fredrickson, PharmD, BPCS, Austin Fredrickson, MD, FACP, and Pamela Sardo, PharmD, BS. Pamela Sardo, Liz Fredrickson, and Austin Fredrickson have no conflicts of interest or financial relationships regarding the subject matter discussed. There are no financial relationships or commercial or financial support relevant to this activity to report or disclose by RxCe.com or any of the individuals involved in the development of this activity.
© RxCe.com LLC 2024: All rights reserved. No reproduction of all or part of any content herein is allowed without the prior, written permission of RxCe.com LLC.
Educational Activity
Burn Care Essentials: A Multidisciplinary Approach to Assessment, Treatment, and Recovery
Introduction
Burn injuries can range from mild to severe and present unique challenges that necessitate a coordinated healthcare team response. Prompt and effective treatment is essential to prevent complications and promote optimal healing outcomes. The management of burn injuries benefits significantly from the application of the Interprofessional Education Collaborative (IPEC) competencies, which emphasize team-based care and collaboration. By leveraging the IPEC competencies—values and ethics, roles and responsibilities, interprofessional communication, and teamwork— healthcare professionals can ensure a high-quality, patient-centered approach to burn care. This continuing education activity will provide learners with a comprehensive review of the classification, pathophysiology, and management of burn injuries. Special attention will be given to the roles of the multidisciplinary care team, fostering a deeper understanding of how interprofessional collaboration can enhance outcomes in burn care.
Overview of Burn Injuries
Burn injuries occur when the skin comes into contact with a damaging agent, including radiation, chemicals, high temperatures, electricity, or friction. Burn injuries are preventable, yet non-fatal burns remain among the leading causes of morbidity and mortality globally.1,2 These injuries, which can range from mild to severe, present unique challenges that necessitate a coordinated healthcare team response.1 The severity of burns is influenced by factors such as the duration and intensity of heat exposure and the burn's location on the body.1 This can lead to significant variability in burn-related morbidity and mortality.1 Prompt and effective treatment is essential to prevent complications and promote optimal healing outcomes. While minor burns are often managed on an outpatient basis, severe burns typically require
intensive, interdisciplinary treatment due to their potential for long-term physical, psychological, and social impacts.1
Classification of Burn Injuries
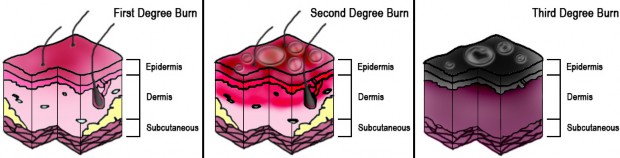
Burns can be distinguished based on several characteristics, including their etiology (discussed in detail below), their depth, and the percentage of body surface area impacted by the burn.1,2 Superficial burns are limited to the epidermis, or outermost layer of the skin, and were previously noted as first- degree burns.2 Partial thickness burns can be deep or superficial and involve the dermis.2 These were previously noted as second-degree burns.2 Superficial partial-thickness burns involve the superficial dermis. Deep partial- thickness burns extend to the deeper dermis and take longer to heal.2 Finally, full-thickness (third-degree) burns extend to the fat layer underlying the dermis.2 The classification of burn injuries is detailed further in Table 1 and illustrated in Figure 1.
Table 1 Classification of Burn Injuries1,2
| Classification | Depth | Characteristic s | Healing Time | Risk of Scarring | Treatment |
Partial-Thickness Burn |
Epidermis | Appendage structures intact, superficial damage |
10–14 days |
Low | May heal without surgical intervention |
Deep Partial- Thickness Burn | Deeper layers of the dermis, greater appendage damage | Damage to deeper dermal layers, fewer intact structures |
3–6 weeks |
High (hypertrophic scarring possible) |
May require specialized wound care |
Full-Thickness Burn | All layers of skin (epidermis, dermis, and subcutaneous tissues) |
Complete destruction of skin layers |
Varies (requires surgical intervention) |
Very High | Typically requires surgery (e.g., skin grafting) |
Figure 1
Classification of Burn Injuries by Depth (with older degree nomenclature used)3
Burn Injury Etiology & Epidemiology
Epidemiology
Burn injuries represent a significant public health issue worldwide, and addressing them requires the coordinated efforts of interprofessional care teams. They account for substantial morbidity and mortality globally. Interprofessional teams, including epidemiologists, public health officials, and clinical care providers, can collaborate to analyze burn injury patterns and target high-risk populations.
In the United States, data from the American Burn Association (ABA) and the Centers for Disease Control and Prevention (CDC) highlight the scope of the issue. The American Burn Association (ABA) is a member-based organization that seeks to improve the lives of individuals affected by burn injuries.4 In 2021, the CDC reported 398,000 fire or burn-related injuries and 252,000 injuries from hot objects or substances.4 The ABA estimated there is one fire-related death in the United States (US) every 2 hours and 17 minutes, and the World Health Organization estimates that burns cause 180,000 deaths every year and remain a significant global public health problem.4,5 Burn injury demographics pertinent to the US are presented in Table 2.4
Table 2 Demographics of Burns Injuries4
| Category | Statistics |
| Burn Admissions | 29,165 admissions/year (88.5 per million people/year) |
| Inpatient Mortality | 2.7% overall (795 deaths) |
Admissions by Burn Severity | 52.4% for minor burns (15,280 cases) 0.36% mortality rate |
4.4% for extensive burns with surgery and ventilation (1,290 cases) 17.8% mortality rate | |
32% for deep burns with surgery, no prolonged ventilation (9,340 cases) 2.6% mortality rate | |
| Hospitals Handling Burn Cases | 94 hospitals with ≥100 burn admissions/year |
| Seasonality of Burn Admissions | 37.5% of admissions occur May-August |
| Geographic Distribution | Most admissions: South Atlantic (26.0%) |
| Fewest admissions: New England (3.0%) | |
Demographics | Gender: 33.3% Female, 66% Male |
Ethnicity: 57.1% White non-Hispanic, 19.6% Black non-Hispanic, 14.5% Hispanic, 2.6% Asian/Pacific Islander, 0.8% Native American | |
Age Distribution |
Children (under 18): Median age 3 years Adults: Median age 49 years |
Risk Factors
Understanding the risk factors for burns enables an interprofessional care team to create targeted prevention and management strategies and mitigate these risks. Certain groups are more vulnerable to burn injuries due to a range of factors related to gender, age, regional disparities, socioeconomic status, and other specific conditions. Females have slightly higher burn-related death rates than males. Males are more likely than females to receive burns globally.5 This increased risk is primarily due to open-
fire cooking and the use of unsafe cookstoves that can ignite loose clothing.4 The use of open flames for heating and lighting further contributes to this risk, as does exposure to self-directed or interpersonal violence.5
Age is another significant factor, particularly for children. Young children, especially those under five, are highly vulnerable to burn injuries, which rank as the fifth most common cause of non-fatal childhood injuries.5 A substantial portion of these injuries stems from a lack of adult supervision and instances of child maltreatment.5
Socioeconomic factors and social drivers of health (SDOH) are critical in influencing burn risks, and addressing these challenges requires an interprofessional, patient-centered approach. Individuals in low- and middle- income countries face more significant hazards, but poverty, overcrowding, and other SDOH contribute significantly to burn risks in any area. By leveraging a team-based approach, interprofessional care teams can develop strategies to mitigate these risks and improve outcomes for vulnerable populations.5 As an example, social workers and public health professionals can collaborate to provide access to safer cooking alternatives and home safety equipment. Nurses and health educators can deliver culturally appropriate safety education tailored to the unique needs of these communities.
Other risk factors include occupational hazards that increase exposure to fire, young girls’ involvement in cooking and child-rearing tasks, and certain underlying medical conditions, such as epilepsy, peripheral neuropathy, and various physical and cognitive disabilities.5 Alcohol abuse and smoking also elevate the risk, as do easy access to harmful chemicals used in assaults, like acid.5 Physicians and rehabilitation specialists can tailor treatment plans that account for these individual vulnerabilities, and nurses can assist patients and caregivers in recognizing and mitigating risks specific to these conditions. Pharmacists can help the team by adjusting medication regimens to reduce side effects that may contribute to falls or accidents.
Understanding these risk factors is essential for effective prevention efforts, especially for vulnerable populations. Safety education, improved supervision, and targeted public awareness initiatives can help reduce the incidence of burns and their associated mortality and morbidity worldwide.
Etiology
The etiology of burns influences treatment decisions, and care teams must integrate their expertise to manage these injuries effectively. The management of burn injuries necessitates a robust, interprofessional approach rooted in the IPEC competencies—Values/Ethics, Roles/Responsibilities, Interprofessional Communication, and Teams/Teamwork. By addressing epidemiological patterns, risk factors, and diverse etiologies collaboratively, healthcare teams can enhance prevention, treatment, and recovery for individuals affected by burns.
Burn injuries can arise from several causes, including thermal, electrical, chemical, and radiation exposures, and these factors play a role in determining the severity of the injury.1 Understanding the causes of burns can assist care team members in determining appropriate treatment strategies and recognizing potential complications that may arise.
Thermal Injuries
Thermal burn injuries are caused by contact with an external heat source, such as a flame or hot liquid.2 The temperature and duration of exposure determine the severity of thermal injuries.1 Types of thermal injuries include the following:
Scalds: These are injuries caused by contact with hot liquids and are the most common type of burn injuries.1 These types of burns often cause partial-thickness burns.1
Dry Heat Injuries: These injuries result from direct contact with flames or radiant heat.1 These types of burns typically result in partial or full-thickness burns.1
Contact Burns: These injuries are caused by prolonged contact with hot objects.1 These types of burns are typically deep.1
For example, during the treatment of a thermal burn, the physician may determine the depth of the injury while the nurse educates the patient on wound care while demonstrating by dressing the wound. The pharmacist ensures appropriate pain management and adjusts fluid resuscitation based on the patient’s condition. Effective communication tools like SBAR (Situation, Background, Assessment, Recommendation) streamline these interactions, ensuring seamless care and enhancing interprofessional collaboration.
Electrical Injuries
The generation of heat and subsequent electroporation of cell membranes results in electrical burns.2 A minority of burn injuries are the result of electrical injuries, and numerous variables play into their severity.1 These include voltage, current type, contact duration, and the pathway of current through the patient’s body.1 Low-voltage injuries can cause localized burns, while high-voltage exposures lead to extensive tissue damage, cardiac arrhythmias, and even limb loss.1 Burns may also result from an electrical arc, causing partial thickness burns on exposed skin.1
Chemical Injuries
Chemical burns also account for a minority of burn injuries (approximately 3%).1 These types of burns involve tissue damage that results from chemical reactions, and they may involve strong acids, strong alkalis (such as lye), phenols, phosphorous, or products like paint thinners.1,2 Factors impacting these types of burns include the concentration, amount, duration of contact, and mechanism of action of the implicated chemical.1
Radiation Injuries
Radiation burns are caused by prolonged exposure to various ultraviolet (UV) radiation sources, including sun and tanning bed exposure.2 Alpha
particles cause significant damage if ingested or inhaled but cannot penetrate the skin.1 Beta particles cause superficial burns similar to sunburns.1 Gamma rays can penetrate deep into the body, damaging internal tissues and causing systemic issues like Acute Radiation Syndrome.1
Pathophysiology of Burns
Burns can result in local and widespread systemic effects for patients.1 The care team should recognize both types of effects to anticipate possible outcomes and devise treatment strategies. The skin plays an important role in mitigating the spread of damage caused by burns, but this will ultimately be determined by temperature and duration of exposure to the causative agent.1,2 Heat from burns causes protein denaturation, leading to coagulative necrosis in the affected tissue.2 The sites of burns have been divided into three zones, which are detailed in Table 3.1
Table 3
Zones of Cutaneous Burn Injuries1
| Zone | Description |
| Zone of Coagulation | The area of maximal damage where irreversible tissue necrosis occurs at the time of injury |
Zone of Stasis | Surrounds the coagulation zone and is moderately damaged Damage results in impaired tissue perfusion, and the zone may recover or progress to necrosis depending on the wound environment |
Zone of Hyperemia | Contains dilated vessels caused by inflammation and is characterized by increased blood flow to healthy tissues Minimal risk of necrosis unless there is severe sepsis or prolonged hypoperfusion |
The systemic effects of burns can be notable, especially when more than 30% of the total body surface area (TBSA) is affected.1 A primary consequence is burn shock, which is characterized by circulatory dysfunction, edema, and microcirculatory damage.1,2 Even with adequate fluid resuscitation, burn shock remains irreversible and often results in multiple organ failure. 1,2 Burns also trigger extensive edema formation, which occurs in two phases: a rapid increase in tissue water content within the first hour and a slower, gradual increase over the next 12–24 hours.1,2 The severity of edema is influenced by fluid resuscitation efforts, with increased blood flow and capillary pressure further exacerbating tissue swelling.1,2
At the cellular level, burns lead to membrane depolarization in various tissues, including skeletal muscles, cardiac cells, and the liver. 1,2 This results in sodium and water accumulation within cells, contributing to cell dysfunction and edema.1,2 These injuries also induce a profound hypermetabolic response, which varies depending on the size of the burn.1,2 In patients with burns covering more than 40% of TBSA, the metabolic rate can more than double, driven by increased secretion of hormones like catecholamines, cortisol, and inflammatory cytokines such as IL-1 and IL-6.1,2
Finally, burns disrupt glucose metabolism, leading to persistent hyperglycemia and insulin resistance.1,2 The heart and kidneys are particularly vulnerable, with burn injuries reducing cardiac output and glomerular filtration rates, potentially causing renal failure if not properly managed. Endocrine disturbances, particularly in the hypothalamic-pituitary axis, further complicate recovery, affecting hormones like thyroid hormones, growth hormone (GH), and insulin-like growth factor (IGF-1).1,2 Overall, the systemic effects of burns involve complex metabolic, hormonal, and inflammatory dysregulation, which pose significant challenges to recovery and rehabilitation, necessitating comprehensive management and monitoring of multiple organ systems.1,2 Table 4 summarizes the complications of burns at local and systemic levels.2
Table 4 Summary of Complications2
| Type | Complication | Description |
Systemic |
Hypovolemia | Fluid loss from burns can lead to hypovolemia, causing reduced blood flow (hypoperfusion) to burned tissue and sometimes leading to shock This results from direct fluid loss in deep burns or burns covering large surface areas, as well as whole-body edema from fluid shifting into the interstitial and cellular spaces. |
Infection | A common cause of sepsis and mortality, infection arises from impaired host defenses and devitalized tissue that fosters bacterial growth Initial pathogens typically include streptococci and staphylococci, with gram-negative bacteria appearing after 5-7 days Mixed flora infections are common | |
Metabolic Abnormalities | Hypoalbuminemia (due to protein loss and hemodilution from fluid replacement) and electrolyte imbalances (such as hypomagnesemia, hypophosphatemia, and hypokalemia) are common Metabolic acidosis may develop from shock, and deep thermal or electrical burns can lead to rhabdomyolysis or hemolysis, potentially causing acute kidney injury | |
Hypothermia | Extensive exposure to body surfaces and administration of cool IV fluids in emergency settings can lead to hypothermia, particularly in patients with large burn areas. | |
Ileus | Paralysis of the intestines (ileus) is common after extensive burns, impairing gastrointestinal function | |
Local |
Eschar | Eschar, or stiff dead tissue from deep burns, can be constricting, particularly if it encircles a limb, neck, or torso |
| Type | Complication | Description |
This constriction prevents tissue expansion, leading to increased tissue pressure, local ischemia, and potential risk to the viability of limbs, digits, or ventilation capacity | ||
Scarring and Contractures | Healing of deep burns can result in scarring and contractures, leading to deformities at joints and potentially impairing function If burns are located near joints (especially in the hands, feet, or perineum), function can be significantly compromised Infection can worsen scarring, and keloids may develop, especially in darker skin. |
Assessment of Burns
Burn assessment requires the combined expertise of an interprofessional team to evaluate depth, extent, and complications. Clear communication, shared decision-making, and role delineation are crucial. Burn assessment involves clinically assessing the depth and extent of the burn.1,2 In some cases, imaging and laboratory testing may be required.1,2 Interprofessional communication and teamwork are critical in recognizing these signs and determining the need for further intervention. A burn infection may be evident by the following signs:6
Wound exudate
Impaired wound healing
Feeding intolerance
Decreased platelet count
Increased serum glucose
Estimating the percentage of total body surface area (TBSA) involved is crucial in managing burn injuries.2 Three common methods for quickly approximating the affected area are the rule of nines, Lund and Browder charts, and the palm method.2 While the rule of nines provides a faster assessment, the Lund and Browder charts are more accurate, especially in children, as they adjust for age-related differences in body surface area.2 The palm method uses the patient’s palm to estimate smaller, scattered burns, with the palm (excluding fingers) representing about 0.5% TBSA and the full palm (including fingers) representing 1% TBSA.2 However, the palm method can overestimate surface area in cases of large burns. Figure 2 illustrates the differences between the rule of nines and Lund-Browder charts. Table 5 details the burn depth assessment.7
Figure 2 Estimating Percent TBSA8
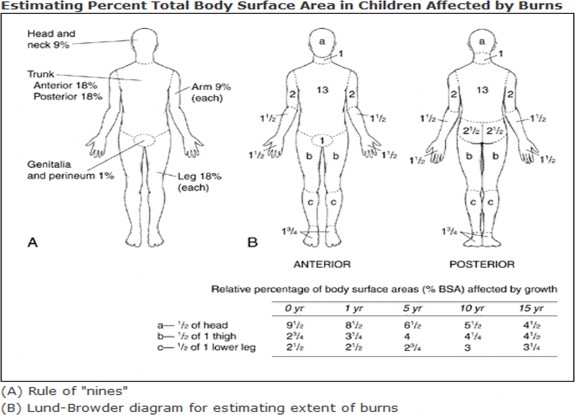
Table 5
Burn Depth Assessment7
Epidermal Burn |
Superficial Dermal/Superficial Partial Burn | Deep Dermal/ Deep Partial Burn |
Full Thickness Burn | |
Pathology |
Involves epidermis only |
Involves the epidermis and upper dermis | Involves the epidermis and most of the dermis | Involves the epidermis and all of the dermis |
Appearance |
Red only |
Pale pink; blanches to pressure | Red or pale pink; non- blanching | Waxy and white; leathery; non- blanching |
Blistering | None or only a few days later | Yes, within hours of the burn | Yes—early blistering |
No |
Patients meeting specific criteria, such as extensive TBSA involvement or burns in high-risk areas (e.g., face, hands, feet), require referral to specialized burn centers. Interprofessional collaboration ensures seamless transitions of care. Some examples include the following:
Care coordinators arrange transportation and communicate referral details with the burn center.
Nurses provide detailed handoffs, including assessments and wound care protocols.
Physicians ensure timely updates to the receiving specialists regarding the patient's condition.
Table 6 provides criteria for referring patients to burn centers.9
Table 6
American Burn Association Criteria for Burn Center Referral9
| Criteria |
| Burns to the face, hands, feet, major joints, genitalia, or perineum |
| Children in health care facilities without staff trained to treat children or appropriate equipment for children |
| Concurrent trauma |
| Electrical or chemical burns |
| Full-thickness (third-degree) burns at any age |
| Greater than 10% of the total body surface area involved |
| Inhalation injuries |
| Need for special support (social, emotional, rehabilitative) |
| Preexisting medical issues that may complicate treatment or recovery or increase mortality risk |
Treatment and Management Strategies
The management of burn injuries benefits significantly from the application of the Interprofessional Education Collaborative (IPEC) competencies, which emphasize team-based care and collaboration.10 By leveraging the IPEC competencies—values and ethics, roles and responsibilities, interprofessional communication, and teamwork—healthcare professionals can ensure a high-quality, patient-centered approach to burn care.
Interprofessional Care Teams
Effective communication and shared decision-making are critical during initial burn assessment and treatment.11 The management of burn injuries exemplifies the need for integrated multidisciplinary care due to the complex nature of these cases. Burn care involves a diverse team of specialists working collaboratively to provide comprehensive care. Research highlights the variability and complexity of multidisciplinary teams in healthcare,
emphasizing the importance of defining team components to optimize the team's functionality.11 Strong communication will be a cornerstone of team success and can assist in fostering coordination within the team and with patients and their families. However, while diverse professional healthcare backgrounds are an asset, they can lead to conflicts, miscommunication, and a loss of patient confidence if members do not communicate well.11
Key challenges include conflicting professional opinions and the potential for patients or families to exacerbate team disagreements inadvertently.11 These issues can be mitigated through frequent, open communication and respect for diverse perspectives.11 Emotional dynamics and conflict resolution are critical for smooth team functioning, and recognizing the value of each member's input is essential. A well-functioning team is characterized by common objectives and aligned values, enabling the delivery of optimal care for burn patients.11 Each team member's primary roles and contributions concerning burn management are summarized in the table below.
Table 7
Team Member's Primary Roles and Contributions in Burn Management11
| Role | Responsibilities |
| Burn Surgeon | Provides overall leadership and care management; delegates tasks; ensures effective communication within the team. |
| Nurses | Delivers continuous patient care; manages critical care needs; supports emotional well-being; and leads patient education. |
| Anesthesiologists | Manages airway, fluid, and circulatory stability during surgery; oversees pain control and critical care interventions. |
| Respiratory Therapists | Manages pulmonary injuries; assists in ventilation and diagnostic procedures; prevents complications like pneumonia. |
| Physical & Occupational Therapists | Designs rehabilitation programs; minimizes scarring and contractures; motivates patients for compliance. |
| Dietitians | Develops nutritional plans to address hypermetabolism; monitors nutritional needs and implements early enteral feeding. |
| Psychosocial Experts | Provides emotional and psychological support to patients and families; addresses grief and long-term adjustment. |
Challenges in this setting have been described in the literature elsewhere. One study examined communication networks within healthcare teams, focusing on the interaction patterns among 71 health professionals in a burn unit across four roles: physicians, nurses, health management/support personnel (dietitians, pharmacists, social workers), and other health professionals (therapists, medical students).12 Using a cross-sectional survey, researchers identified communication ties based on discussions about patient care during shifts.12 Findings revealed that 94% of health management/support personnel’s ties were interprofessional, compared to 60% for nurses. Nurses and other health professionals were less likely than physicians to form ties, and nurses were 1.64 times more likely to communicate with other nurses than non-nurses.12 Physicians and health management/support personnel showed no significant preference for interprofessional communication.12 Understanding these networks is crucial
for improving teamwork in healthcare, with future studies needed to explore the quality and types of interprofessional interactions.12 Barriers for care teams are presented in Table 8.
Table 8
Barriers to Interprofessional Collaboration
| Barrier | Description | Solution |
Communication Challenges | Miscommunication or lack of communication among team members can lead to errors and fragmented care. | Implement structured communication tools like SBAR and schedule routine interdisciplinary meetings. |
Role Ambiguity | An unclear understanding of each team member's roles and responsibilities can cause overlap or gaps in care. | Clearly outline roles and responsibilities and provide interprofessional education to foster mutual respect. |
Hierarchical Structures | Traditional hierarchies can inhibit open communication, with lower-ranking members hesitant to voice concerns or suggestions. | Encourage equality, inclusive discussions, and train leaders to value input from all disciplines. |
Time Constraints | Busy schedules and heavy workloads can limit opportunities for team collaboration and communication. | Utilize brief, focused huddles or bedside rounds, and allocate specific times for interdisciplinary activities. |
Cultural and Professional Differences | Variations in professional cultures, terminologies, and approaches can lead to misunderstandings and conflicts. | Offer cultural competency training and engage in team-building activities to build trust and rapport. |
Lack of Interprofessional Education | Limited training on collaborative practices during professional education can result in inadequate preparation for teamwork. | Incorporate interprofessional education modules into healthcare training and offer continuing education workshops. |
Resource Limitations | Insufficient staffing, facilities, or financial resources can hinder the ability to implement collaborative practices effectively. | Advocate for resources and optimize existing tools and technologies to facilitate communication and coordination. |
Treatment Strategies
Burns to the face or neck, or resulting from enclosed fires or chemicals increase the risk of airway injury and require close monitoring.9 A quick assessment to identify the cause and extent of the burn is critical, though determining burn depth can be difficult initially.9 Deep burns often exhibit slow or absent skin blanching and pain intensity decreases with burn depth.9 Burn injuries are dynamic and can worsen over 24 to 72 hours, with even minor burns potentially deepening due to factors like inadequate treatment or infection.9 Treatment strategies and their related benefits are summarized in Table 7 and discussed in more detail below.
Table 9 Treatment1
| Treatment | Description | Key Benefits |
Cooling of Burned Areas | Immediate cooling of burned tissue at 10–20°C to reduce temperature and pain | Reduces tissue damage, provides relief, avoids frostbite or hypothermia |
Fluid Resuscitation | Uses the Parkland formula to estimate and administer fluids after severe burns | Prevents hypovolemic shock, maintains organ function |
| Treatment | Description | Key Benefits |
Ventilation | Lung-protective ventilation strategies for respiratory burns | Reduces lung damage, improves respiratory outcomes |
Surgical Treatment | Early excision of burn wounds, skin grafting, reconstructive surgery | Lowers infection risk, speeds healing, restores function and appearance |
Sepsis Management | Prevention through antimicrobial dressings, excision, nutritional support | Reduces infection risk, lowers sepsis-related mortality |
Thermoregulation | Raising ambient temperature in care settings to maintain patient body temperature | Reduces hypermetabolism, prevents hypothermia |
Contracture Prevention | Physical therapy, corticosteroids, hydrotherapy, and surgical interventions | Prevents permanent contractures, improves mobility |
Hormonal Regulation | Use of growth hormone, IGF-1, insulin, oxandrolone, and propranolol | Promotes muscle growth, reduces catabolism, improves healing |
Nutrition | Enteral feeding with high- protein, high-carbohydrate diets | Maintains lean body mass, preserves gut function, reduces infection risk |
Minor Burns
The primary goals of treating minor burns are to limit damage, clean the wound, and manage pain.9 For scalds, removing clothing immediately helps minimize injury.9 Chemical burns require careful removal of contaminated clothing using protective gear.9 To prevent further complications, any items that could restrict circulation (e.g., jewelry, belts) should be removed, and the environment should be kept warm, as burns impair thermoregulation.9
Cooling the burn with running water (46.4°F to 77°F) for at least 20 minutes, ideally within 30 minutes but effective up to three hours post-burn, reduces burn depth and accelerates healing.9 However, ice should not be used,
as it can cause further damage.9 Cleaning with tap water is sufficient to prevent infection, and sterile or antiseptic agents are unnecessary.9
Superficial burns typically do not require dressings, though wet gauze may reduce pain.9 Maintaining a moist environment is crucial for superficial partial-thickness burns to promote healing and prevent complications. Blister management, particularly in partial-thickness burns, is debated.9 Large or joint-area blisters may require debridement to reduce infection risk and improve healing, though recent evidence suggests aspiration may be equally effective.9
There are two common approaches to dressing partial-thickness burns. One involves applying a topical antimicrobial agent with regular dressing changes to monitor progress. Silver sulfadiazine is a popular choice, though it has been shown to delay healing and may increase infection risk, with studies suggesting it impairs immune function and wound recovery.9 Topical agents are described in Table 10.9
Table 10 Topical Treatments9
| Agent | Description | Advantages | Disadvantages |
Bacitracin |
Antimicrobial ointment | Inexpensive and painless; can be used on the face and near mucous membranes | Narrow microbial coverage, frequent dressing changes, does not penetrate eschar |
Impregnated nonadherent gauze |
Semiocclusive, non-absorptive dressing | Nonadherent barrier helps maintain a moist environment, clings to the body | No antimicrobial activity |
Mafenide acetate | Water-based cream; bacteriostatic against gram- positive and gram- negative bacteria | Pseudomonal coverage, penetrates eschar, can be used for deep burns or on the face | Pain with application, may delay wound healing, associated with metabolic acidosis |
| Agent | Description | Advantages | Disadvantages |
Medical grade honey | Variety of preparations, including honey- based hydrogel dressings | Inhibits growth of common burn pathogens, reduces healing time for partial- thickness burns | Low-quality evidence |
Mupirocin |
Ointment; inhibits bacterial protein and RNA synthesis | Good gram- positive antimicrobial coverage, effective against MRSA, painless, may be used on the face | Frequent dressing changes, expensive |
Silver sulfadiazine | Water-based cream; interferes with bacterial DNA synthesis | Painless, long shelf life, broad antimicrobial coverage | Delays wound healing, frequent dressing changes, contraindicated in certain populations |
Severe Burns
Initial care for burns in the prehospital setting includes providing oxygen for smoke inhalation, extinguishing ongoing burning, and removing hot or smoldering material.2 For chemical burns, extensive flushing with water is essential.2 Partial-thickness and full-thickness burns covering more than 10% of the total body surface area (TBSA) require intravenous (IV) fluids based on the Parkland formula to address fluid loss and prevent shock.2
Wound care involves cleansing, dressing, and ongoing assessment.2 Small blisters may be left intact, while ruptured ones are debrided. Antimicrobial ointments, silver dressings, or biosynthetic coverings may be applied to protect the wound.2 If burns exceed 20% TBSA or if the patient is malnourished, nutritional support is initiated.2 For larger or complex burns, specialized care in burn centers is often necessary.2 Surgery, including escharotomy, excision, and grafting, is required for deep partial-thickness and full-thickness burns, often within three days of injury, to prevent sepsis and promote healing.2
Infections are managed without routine prophylactic antibiotics; infections presenting after five days require broad-spectrum antibiotics, which are tailored based on culture results.2 Physical and occupational therapy are crucial to maintain mobility and prevent contractures.2 Outpatient treatment, where feasible, involves daily dressing changes and maintaining cleanliness, elevation, and compression.2
Preventing Burn Injuries
Burns are largely preventable, and high-income countries have made significant strides in reducing burn-related deaths by implementing comprehensive prevention strategies and improving care for burn victims.5 Effective prevention requires a multidimensional, interprofessional approach, as emphasized by the IPEC competencies. Collaboration across disciplines ensures that prevention efforts target specific hazards, educate vulnerable populations, and equip communities with the skills and resources needed to minimize risks. A successful prevention plan should be multidimensional, focusing on improving awareness, creating and enforcing effective policies, identifying risk factors, setting research priorities, promoting interventions, providing prevention programs, and strengthening burn care and capacity.5
Several specific measures can help reduce burn risks at individual, community, and public health levels. These include enclosing fires and controlling open flame heights in homes, promoting safer stoves and fuels. Housing regulations should encourage fire-safe design and materials, while stove designs should prioritize stability and child safety.5 Lowering hot water tap temperatures, promoting fire safety education, and encouraging smoke detectors, fire sprinklers, and fire-escape systems are crucial.5 Compliance with industrial safety regulations, use of fire-retardant fabrics for children's sleepwear, and avoiding smoking in bed are also vital steps.5
Summary
Burn injuries, which can range from mild to severe, present a unique and complex challenge for healthcare professionals, requiring prompt and
effective treatment to prevent complications and promote healing. While minor burns can often be managed on an outpatient basis, severe burns require intensive treatment and have the potential to create long-lasting impacts on patients.
Burn injuries occur when the skin comes into contact with a damaging agent, including radiation, chemicals, high temperatures, electricity, or friction. Burns can be distinguished based on several characteristics, including their etiology, their depth, and the percentage of body surface area impacted by the burn.
Burn assessment requires the combined expertise of an interprofessional team to evaluate depth, extent, and complications. Clear communication, shared decision-making, and role delineation are crucial. The management of burn injuries benefits significantly from the application of the Interprofessional Education Collaborative (IPEC) competencies, which emphasize team-based care and collaboration.
Burns can result in local and widespread systemic effects for patients. The care team should recognize both types of effects to anticipate possible outcomes and devise treatment strategies. Criteria may be present for referring patients to burn centers.
Course Test
Which layer of the skin is affected by a superficial burn?
Dermis
Subcutaneous layer
Epidermis
Muscle
Which of the following is classified as a partial thickness burn that extends into the deeper dermis with a high risk of hypertrophic scarring?
Superficial partial-thickness burn
Deep partial-thickness burn
Superficial burn
Full-thickness burn
Which of the following best describes the classification of burns by depth?
Superficial, partial-thickness, and full-thickness
Minor, moderate, and severe
Acute, chronic, and systemic
First, second, and third degrees only
Which of the following steps should be taken first for a minor burn?
Immediate application of ice
Cooling with running water
Debridement of all blisters
Application of silver sulfadiazine
Which of the following topical agents is associated with delayed wound healing in minor burns?
Bacitracin
Mupirocin
Silver sulfadiazine
Honey-based dressings
Hypovolemia in burn patients is primarily due to which of the following?
Poor nutritional intake
Direct fluid loss and fluid shifts to interstitial spaces
Increased metabolic rate
Decreased cardiac output
Which of the following is a common cause of sepsis in burn patients?
Viral infection
Overuse of antibiotics
Bacterial colonization in devitalized tissue
Hypothermia
Which of the following abnormalities is common in burn injuries?
Hypernatremia
Hypoalbuminemia
Hypochloremia
Hyperkalemia
Which principle of teamwork is most critical to fostering effective interprofessional collaboration in caring for burn injury patients?
Each team member independently deciding their patient care role
Regular interdisciplinary team meetings to review and adjust care plans
Relying solely on the nurse for care coordination and follow-up
Prioritizing efficiency over patient-centered care during treatment discussions
Which of the following principles best supports teamwork in the care of burn injury patients?
Unilateral decision-making by the attending physician
Active engagement and mutual respect among team members
Delegating all patient interaction to a single team member
Frequent interruptions to ensure immediate feedback.
References
Żwierełło W, Piorun K, Skórka-Majewicz M, Maruszewska A, Antoniewski J, Gutowska I. Burns: Classification, Pathophysiology, and Treatment: A Review. Int J Mol Sci. 2023;24(4):3749. Published 2023 Feb 13. doi:10.3390/ijms24043749
Carter, D. Burns. Merck Manual. September 2024. Accessed November 2024. https://www.merckmanuals.com/professional/injuries- poisoning/burns/burns
Wikimedia Commons. Burn Degree Diagram. Accessed November 2024. https://commons.wikimedia.org/wiki/File:Burn_Degree_Diagram.png
Burn Incidence Fact Sheet. The American Burn Association. Accessed November 2024. https://ameriburn.org/resources/burn-incidence-fact- sheet/
Kamolz LP, Parvizi D, Giretzlehner M, et al: Burn surface area calculation: What do we need in future. Burns 40(1):171-172, 2014. doi: 10.1016/j.burns.2013.07
Wall S, Perumal-Pillay VA. Burning Questions: What Should the Pharmacist Know about Managing Minor Burns?. Pharmacy (Basel). 2022;10(4):100. Published 2022 Aug 22.
doi:10.3390/pharmacy10040100
Radiation Emergency Medical Management. U.S. Health and Human Services. November 13, 2024. Accessed December 2, 2024. https://remm.hhs.gov/burns.htm
Lanham JS, Nelson NK, Hendren B, Jordan TS. Outpatient Burn Care: Prevention and Treatment. Am Fam Physician. 2020;101(8):463-470.
Interprofessional Education Collaborative. IPEC Core Competencies for Interprofessional Collaborative Practice: Version 3. November 20, 2023. Washington, DC: Interprofessional Education Collaborative.
Al-Mousawi AM, Mecott-Rivera GA, Jeschke MG, Herndon DN. Burn teams and burn centers: the importance of a comprehensive team approach to burn care. Clin Plast Surg. 2009;36(4):547-54. doi: 10.1016/j.cps.2009.05.015
Shoham DA, Harris JK, Mundt M, McGaghie W. A network model of communication in an interprofessional team of healthcare professionals: A cross-sectional study of a burn unit. J Interprof Care.
2016;30(5):661-667. doi:10.1080/13561820.2016.1203296
DISCLAIMER
The information provided in this course is general in nature, and it is solely designed to provide participants with continuing education credit(s). This course and materials are not meant to substitute for the independent, professional judgment of any participant regarding that
participant’s professional practice, including but not limited to patient assessment, diagnosis, treatment, and/or health management. Medical and pharmacy practices, rules, and laws vary from state to state, and this course does not cover the laws of each state; therefore, participants must consult the laws of their state as they relate to their professional practice.
Healthcare professionals, including pharmacists and pharmacy technicians, must consult with their employer, healthcare facility, hospital, or other organization, for guidelines, protocols, and procedures they are to follow. The information provided in this course does not replace those guidelines, protocols, and procedures but is for academic purposes only, and this course’s limited purpose is for the completion of continuing education credits.
Participants are advised and acknowledge that information related to medications, their administration, dosing, contraindications, adverse reactions, interactions, warnings, precautions, or accepted uses are constantly changing, and any person taking this course understands that such person must make an independent review of medication information prior to any patient assessment, diagnosis, treatment and/or health management. Any discussion of off-label use of any medication, device, or procedure is informational only, and such uses are not endorsed hereby.
Nothing contained in this course represents the opinions, views, judgments, or conclusions of RxCe.com LLC. RxCe.com LLC is not liable or responsible to any person for any inaccuracy, error, or omission with respect to this course, or course material.
© RxCe.com LLC 2024: All rights reserved. No reproduction of all or part of any content herein is allowed without the prior, written permission of RxCe.com LLC.
