LUPUS: A COMPLEX AUTOIMMUNE DISEASE
SALAM KADHIM, PhD
Salam Kadhim is a pharmaceutical scientist with experience in drug discovery and development of small molecule compounds, biologics, siRNA, and cannabinoids in the areas of oncology, HBV, cardiovascular, ocular, and neurodegenerative disorders.
Topic Overview
Systemic lupus erythematosus (SLE), or lupus, is a chronic, progressive autoimmune disorder in which the immune system attacks its own healthy tissues, causing widespread inflammation and tissue damage to multiple organ systems. Due to its heterogeneity, it has a significant impact on many dimensions of patients’ well-being, causing marked impairment in health- related quality of life. This course provides insights into the definition and types of lupus, clinical manifestations, laboratory screen measures for diagnosis as well as the currently available medications with their associated adverse effects. Furthermore, a gap analysis of the current treatment practices will be compared to the best practice to identify areas of improvement. Special topics in managing flares, during pregnancy, in pediatrics, risk factors, and patient counseling are also reviewed.
Accreditation Statement:

RxCe.com LLC is accredited by the Accreditation Council for Pharmacy Education (ACPE) as a provider of continuing pharmacy education.
Universal Activity Number (UAN): The ACPE Universal Activity Number assigned to this activity is
Pharmacist 0669-0000-23-079-H01-P
Pharmacy Technician 0669-0000-23-080-H01-T
Credits: 2 hours of continuing education credit
Type of Activity: Knowledge
Media: Internet/Home study Fee Information: $6.99
Estimated time to complete activity: 2 hours, including Course Test and course evaluation.
Release Date: June 10, 2023 Expiration Date: June 10, 2026
Target Audience: This educational activity is for pharmacists.
How to Earn Credit: From June 10, 2023, through June 10, 2026, participants must:
Read the “learning objectives” and “author and planning team disclosures;”
Study the section entitled “educational activity;” and
Complete the Course Test and Evaluation form. The Course Test will be graded automatically. Following successful completion of the Course Test with a score of 70% or higher, a statement of participation will be made available immediately. (No partial credit will be given.)
Credit for this course will be uploaded to CPE Monitor®.
Learning Objectives: Upon completing this educational activity, participants should be able to:
Provide insights into the definition and different types of lupus.
Describe clinical manifestations comprising systemic and specific symptoms of organ-system dysfunction associated with lupus.
Describe laboratory screen tests for diagnosis and classification criteria of lupus.
Describe current treatments in the management of lupus.
Discuss the current challenges and future directions in lupus treatment and management.
Disclosures
The following individuals were involved in developing this activity: Salam Kadhim, PhD, and Pamela Sardo, PharmD, BS. Salam Kadhim, PhD, was a senior scientist at Inmed Pharmaceuticals until July 1, 2022. Pamela Sardo, PharmD, BS, was an employee of Rhythm Pharmaceuticals until March 2022. There are no financial relationships relevant to this activity to report or disclose by any of the individuals involved in the development of this activity.
© RxCe.com LLC 2023: All rights reserved. No reproduction of all or part of any content herein is allowed without the prior, written permission of RxCe.com LLC.
Introduction
Systemic lupus erythematosus is a chronic, complex autoimmune disease. It is the most common type of lupus. Lupus can develop in individuals from all population groups, but it is most prevalent among women. Lupus treatment is highly individualized and depends on symptom manifestations, organ involvement, disease severity, and patient response. These include pharmacological and nonpharmacological treatments and counseling for the lupus patient. An approach that treats the condition early, with sustained symptom management, can prevent organ damage, and the patient’s quality of life and long-term survival can be improved.
Overview of Lupus
Systemic lupus erythematosus (SLE) is a chronic multisystem autoimmune disease that manifests itself when the immune system attacks its own healthy tissues.1 This attack causes widespread inflammation and tissue damage affecting skin, joints, heart, lungs, kidneys, and blood vessels.1 Systemic lupus erythematosus is not curable so treatments will involve the management of symptoms and protection from organ injury.1,2
The prevalence of SLE has been estimated to be 30–50 per 100,000, equating to approximately 500,000 patients in Europe and 250,000 in the USA.2,3 The incidence and prevalence are higher in African Americans, Native American, Asian, and Hispanic/Latino patients who develop more severe disease with higher mortality than Caucasian patients.4–6 Systemic lupus erythematosus has a prominent female predominance, especially in women of childbearing age. The female-to-male ratio is as high as 13:1. It is only at 2:1 in children and the elderly.7,8 African-American women are about 3 times more likely to have lupus and suffer greater mortality compared to Caucasian women.9 Systemic lupus erythematosus often follows a characteristic pattern of relapse and remissions and typically develops over an extended period of time.10,11 The exact etiology of the disease is unknown; however, it is associated with a complex and multifactorial interaction of genetic, environmental, immunological, and hormonal factors.12,13
Definition and Pathogenesis of Lupus
Systemic lupus erythematosus is an inadequately defined chronic autoimmune disease involving multiple organs and biological processes. It displays a pleomorphic clinical course with a poorly understood pathogenesis.14,15 Lupus may be divided into different types:16
Systemic Lupus Erythematosus is the most common form of lupus.
Cutaneous lupus is a form of lupus that is limited to the skin.
Drug-induced lupus is a lupus-like disease caused by certain prescription drugs.
Neonatal lupus is a rare condition that affects infants of women who have lupus.
“Childhood lupus” in children affects the body in the same manner as adult lupus. Boys have a higher prevalence of lupus than males in adulthood. Childhood lupus affects certain organs, such as the kidneys, to a greater extent.
Autoantibody production is a central immunological disorder and one of the main contributing factors in the development of SLE. A wide spectrum of autoantibodies directed at self-antigens in the nucleus, cytoplasm, and cell membrane are characteristically present in more than 95% of patients with SLE.17 Anti-double stranded DNA (ds-DNA) and anti-Smith (anti-Sm) autoantibodies are unique to patients with SLE.17,18 Anti-dsDNA antibodies bind to a conserved nucleic acid determinant widely present on DNA, whereas, anti-Sm antibodies react with small nuclear ribonucleoprotein (snRNP).17 Anti- DNA antibodies show preferential deposition in the kidneys, indicating that these autoantibody-immune complexes are the main mediators of inflammation.19 The most remarkable feature of anti-DNA antibodies is their association with glomerulonephritis (inflammation and damage of the glomeruli, the filtration units of kidneys).20
Defective immune regulation of innate and adaptive arms of the immune system in SLE results in the loss of immune tolerance to self-antigens.21 Several abnormalities of the immune system contribute to the disease and
involve defective B cell suppression, excess T cell help, impaired phagocytic function, induction of polyclonal B cell activation, increased number of antibody-producing cells, hypergammaglobulinemia, autoantibody production, and immune complex formation.15 B cell activation is abnormal in patients with SLE, and their number is increased in peripheral blood at all stages of activation.17,22 T-cells are defective, and their aberration is evident by increased apoptosis and decreased number in peripheral blood of SLE patients.23,24 Excessive and uncontrolled T cell help plays a central role in differentiation and activation of autoantibody forming B cells and is the final common pathway.25 Furthermore, strong induction of proinflammatory type 1 Interferon pathway is recognized as the pivotal role of the innate immune system in lupus.26,27
Genome-wide association studies (GWAS) have confirmed the importance of genetic susceptibility to SLE associated with the immune response, endothelial function, and tissue response to injury.28,29 Linkage analyses using SLE multiplex families provided several chromosomal regions of susceptibility genes significantly linked to SLE.30,31 Genetic predisposition to lupus is indicated by the 11–50% monozygotic twin concordance and increased family risk.32 Several genes encoding immune components such as HLA, IRF5, ITGAM, STAT4, BLK and CTLA4 among others have been associated with predisposition to lupus.32,33 The human leucocyte antigen (HLA) class II gene has been associated with the presence of autoantibodies such as anti- Sm, anti-Ro, anti-La, anti-nRNP, and anti-dsDNA.34 Inherited complement deficiencies in HLA class III genes - particularly encoding complement components C2, C4, and C1q - are also implicated in SLE’s pathogenesis.35
Apoptosis plays a pivotal role in the pathogenesis of lupus. Apoptotic cells such as UV-light exposed keratinocytes release blebs rich in surface autoantigens, including Ro, La, and RNP.36,37 These autoantigens combined with antibodies form large aggregates of immune complexes that circulate in the bloodstream, overwhelming clearance mechanisms by phagocytic cells.38 The immune complexes are ultimately deposited in various tissues and organs, leading to acute and chronic inflammation and consequent organ damage.29
Hormonal milieu involving endogenous sex hormones at the hypothalamo–pituitary–adrenal (HPA) axis is implicated in predisposition to SLE and modulates its clinical expression.17,39 Abnormal estrogen metabolism has been demonstrated in patients with SLE of both sexes, with an increase in 16a hydroxylation of estrone, resulting in significantly raised 16a hydroxyestrone concentrations.40 Women with SLE also have low plasma androgens, including testosterone, dihydrotestosterone, dehydroepiandrosterone (DHEA), and dehydroepiandrosterone sulfate.41,42
Figure: Pathogenesis of SLE
| Environmental Triggers | Multiple Genes | Neuro - Endocrine System | Sex and Sex Hormones Milieu |

Immune Dysregulation
DNA
Apoptotic
Defective Clearance Mechanisms
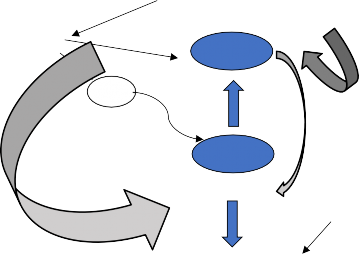
Loss of Suppressor
Mechanisms
B Cells
APC
Excess T-Cell Help Cytokines
T Cells Autoantibodies
Defective Clearance
Immune Complexes Complement Activation

Tissue Damage
Diagnosis of Lupus
Systemic lupus erythematosus diagnosis is based on classification criteria established by the American College of Rheumatology (ACR).43 A minimum of 4 out of 11 ACR criteria should be met for accurate diagnosis. The 11 ACR criteria are the following:
Discoid rash: a rash that appears as red, raised, disk-shaped patches.
Hematologic disorder: hemolytic anemia, leukopenia, lymphopenia, or thrombocytopenia.
Immunologic disorder: anti-DNA, anti-Smith antibodies, lupus anticoagulant or positive antiphospholipid antibodies on testing.
Malar rash: a butterfly-shaped rash over the nose and cheeks; can be flat or raised.
Neurological disorder: seizures or psychosis in the absence of offending drugs or known metabolic conditions.
Nonerosive arthritis: joint pain and swelling of two or more joints.
Oral ulcers: sores, usually painless, appearing in the mouth or nasopharynx.
Photosensitivity: an unusual reaction to sun or light that causes a rash to appear.
Positive antinuclear antibody at any point in time in the absence of medications/drugs.
Renal disorder: persistent protein (>0.5 gram/day) or any cellular casts.
Serositis: pleuritis (inflammation around the lungs) or pericarditis (inflammation around the heart).
Systemic Lupus Erythematosus Disease Activity Index (SLEDAI) and its modification SLEDAI-2K have been developed and validated as a reliable clinical index for measuring disease activity in SLE. It reflects persistent activity in a rash, mucous membranes, alopecia, and proteinuria and is suitable for use as a scoring system in clinical trials and studies of prognosis in SLE.44
Laboratory Tests
The most important laboratory screening measure for SLE is the blood test for antinuclear antibodies, which is highly specific, with a positive result in >95% of SLE patients.45,46 However, antinuclear antibodies are also found in conditions other than SLE; therefore, more specific tests for the detection of anti-dsDNA, anti-Sm, and antiphospholipid antibodies are required to confirm SLE diagnosis.43 The anti-dsDNA antibody test is positive in 60% of SLE patients and is considered the best biomarker for disease activity, with a specificity of almost 100%, except in elderly patients who have a lower prevalence of anti-dsDNA.47 Anti-Ro or SSA antibodies with anti-La (SSB) occur in 20% to 30% of patients. Anti-Ro antibodies are associated with subcutaneous lesions and sicca syndrome, and SSB with malar rash, subcutaneous lesions, photosensitivity, arthritis, serositis, and thrombosis. Anti-U1-snRNP occurs in 13% of patients, and anti-Sm antibodies occur in 10% of patients, especially those with oral ulcers and myositis.48 In addition to laboratory tests, renal biopsy is required for patients with renal complications.49 Recently, monitoring specific B-cell subsets as biomarkers of disease activity are also utilized.50
Clinical Manifestations
Clinical manifestations of SLE can comprise systemic symptoms and specific signs of organ-system dysfunction.10 Common presenting systemic symptoms are severe fatigue, malaise, fever, anorexia, weight loss, and lymphadenopathy.51 Patients may present with signs of systemic infection often because of their disease or side effects of treatments.11 They can also present with frequent flares resulting in inflammation-driven irreversible damage.52 Ninety percent of patients have organ-specific manifestations, including thrombocytopenia, joint inflammation such as arthralgia, arthritis, tendinitis, or stiffness in the knees, wrists, and hands.53 Joint inflammation in SLE patients is distinguished from rheumatoid arthritis by its lack of joint destruction.10,11 Myalgias and muscle weakness are common, and up to 90% of patients with SLE present with symmetrical joint pain, which is typically a migratory polyarthropathy.51 Thirty-five percent of patients will have some form of glomerulonephritis or nephrotic syndrome symptoms and signs
predicting a worse outcome.54 Lupus nephritis (LN) is a major cause of morbidity and increased mortality, with a life-long risk for severe nephritis at approximately 20%.55 The SLE patients may also present with several dermatologic findings, including discoid and malar lesions, photosensitivity, alopecia, periungual erythema, nailfold infarcts, and splinter hemorrhages.10,11 Oral mucosal ulceration occurring in 50% of all cases is also a common feature in SLE.45
Risk Factors for Lupus
Multiple environmental triggers, heritability, and co-segregation with other autoimmune diseases create a predisposition toward the development of SLE. 13,17,52 The main environmental risk factors include:
Chemical/physical factors that can cause inflammation, induce cellular apoptosis, and tissue damage.
Aromatic amines
Hydrazines
Tobacco smoke
Hair dyes
Ultraviolet light
Toxins/drugs that can modify cellular responsiveness and immunogenicity of self-antigens.
Toxins (silica, mercury)
Drugs (procainamide, hydralazine, chlorpromazine, isoniazid, phenytoin, penicillamine)
Dietary factors, select prescription medications, and supplements that affect the production of inflammatory mediators.
L-canavanine (alfalfa sprouts)
High intake of saturated fats
Echinacea
Spirulina
Vitamin E
Trimethoprim/sulfamethoxazole
Infectious agents may induce specific responses by molecular mimicry and disturb immunoregulation. These include the following:
L-Bacterial DNA / Endotoxins
RNA viruses (Retroviruses)
DNA viruses (Cytomegalovirus and Epstein-Barr virus)
Hormones and environmental estrogen.
Hormonal replacement therapy
Oral contraceptive pills
Prenatal exposure to estrogens
Psychological Stress.
Trauma
Post-traumatic stress disorder
Vaccination.
Medicines for the treatment of lupus affecting immunization.
Inability of the immune system to produce protective antibodies.
Special Populations
Pregnancy
Since SLE onset is often in young adulthood, pregnancy is common and is usually successful. However, pregnancy in SLE is considered a high-risk factor in which maternal and fetal mortalities are significantly increased.56–59 Pregnant women with active SLE have more than twice the cumulative rate of adverse pregnancy outcomes (APOs) than healthy pregnant women.60–63 These APOs include preeclampsia, preterm delivery, pregnancy loss, intrauterine growth restriction (IUGR), and other problems such as thrombosis and infection.64,65 The predictors of APO involve active maternal disease, nephritis, proteinuria, hypertension, thrombocytopenia, and the presence of antiphospholipid antibodies (aPLs), particularly lupus anticoagulant.66–68 Pregnant women with SLE, especially the ones with associated antiphospholipid syndrome (APS), have repeated miscarriages and fetal loss.69
Risk of SLE flare is also higher during pregnancy with variable flare rates between 25% to 65% depending on patient populations.70 Moreover, pregnancy may carry a very high maternal risk in a subset of patients with SLE and should be avoided in women with the following conditions:58
Severe pulmonary hypertension (systolic pulmonary artery pressure
>50 mm Hg)
Severe restrictive lung disease (forced vital capacity <1 L)
Advanced renal insufficiency (creatinine level >2.8 mg/dL)
Advanced heart failure
Previous severe preeclampsia or HELLP (hemolysis, elevated liver enzyme levels, low platelet count) despite therapy
Stroke within the previous 6 months
Severe disease flare within last 6 months
Despite the adverse factors women with SLE can nevertheless have successful pregnancies provided there is an optimal timing of conception and close monitoring to risk stratify and plan management strategy for each pregnancy.
Pediatric Patients
Pediatric SLE most frequently occurs between the ages of 12 and 18 years and represents ∼15–20% of all SLE patients. While presentation, clinical symptoms, and immunological findings are like those of adult SLE in many respects, pediatric SLE is different.71,72 Children typically have a more severe disease at the onset with more frequent discoid rash, higher rates of organ involvement, and a more aggressive clinical course.73,74 However, damage to certain organs, like the kidneys, can appear more often in childhood lupus.16
Although pediatric SLE patients have a higher incidence of major organ involvement, the mortality rate is low.75 Manifestations frequently begin with renal, neurological, hematological, and atypical (abdominal) complications.76 The incidence of LN is more common in the childhood-onset form of SLE.77,78 Ethnicity also influences SLE manifestations, with Hispanic and African
American children having higher incidence, greater prevalence, and severity of renal and CNS involvement.78,79 Serologically, anti-DNA, anti-Sm, anti-RNP antibodies, and low C3 are also found more frequently in the younger SLE patients.80
Treatments for Managing Lupus
Treatment of SLE is highly individualized and depends on symptom manifestations, organ involvement, disease severity, and the patient’s response.2,44 Childhood lupus usually requires more aggressive treatments than adult lupus; however, clinicians must guard against the risk posed by some long-term medications (e.g., prednisone).16
Nonpharmacological Treatments
Patient education and psychosocial support are important aspects of SLE nonpharmacological management and are recommended by both EULAR and ACR guidelines.2,44 All patients with SLE are counseled on lifestyle modifications and guided to:
Avoid direct exposure to sunlight and use sunscreen blockers of both UVA and UVB rays.
Cease smoking.
Maintain proper nutrition and weight control.
Maintain adequate intake of calcium and vitamin D.
Ensure adequate exercise.
Alleviate depression and anxiety.
Screen for bone loss.
Pharmacological Treatments
Nonsteroidal anti-inflammatory drugs (NSAIDs)
Drugs such as celecoxib, piroxicam, and ketorolac are commonly used to relieve arthralgia, inflammation, serositis, and fever in SLE. The
maximum celecoxib dose is 200 mg twice daily. The maximum dose of piroxicam is 20 mg daily in adults.81 These can be used with or without low doses of steroids or antimalarial agents.2,82 When taking NSAIDs, it is important to use the lowest dose that is effective and take it for the shortest time. Adverse events are common, especially gastrointestinal bleeding, including upper and lower gastrointestinal tract complications.83 NSAIDs may worsen kidney function or contribute to fluid retention, so monitoring should occur.84 Refer to the full prescribing information of each prescribed agent for comprehensive safety and efficacy.
Low-dose aspirin is also prescribed in some individuals suffering from lupus.85 It has pain-reducing, anti-inflammatory, and anticoagulant properties.
Antimalarials
Drugs such as hydroxychloroquine and chloroquine are non- immunosuppressive agents that are used to reduce flares, prevent organ damage, and is particularly useful for arthralgias and cutaneous SLE.86,87 Hydroxychloroquine, is frequently used as a first-line treatment to prevent the occurrence of mild SLE manifestations.88 It has been shown to maintain remission, protect against vascular and thrombotic events, and improve lipid levels.89,90 It can also be used during pregnancy.2 Hydroxychloroquine is dosed as 200 mg once daily or 400 mg once daily (or in two divided doses) in adults.91 Chloroquine is not FDA-approved for lupus. The common side effects are gastrointestinal upset, dermatologic reactions, headache, and light-headedness. Retinal toxicity and macular damage can occur over time due to drug accumulation in the ocular tissue.45,51
Glucocorticoids
Drugs such as prednisone and prednisolone affect all components of the immune system and are used at low doses for mild SLE or treatment of
cutaneous and musculoskeletal symptoms not responding to other therapies.86 Higher doses given systemically are used for patients with significant organ involvement or refractory symptoms.82 Generally, less than 7.5 mg/day of prednisone is considered a low dose, and more than 30 mg/day is considered a high dose.92 Long-term complications with glucocorticoids include myopathy, osteoporosis, hypertension, diabetes, atherosclerotic vascular disease, and infections.45
Cytotoxic/immunosuppressive agents
Cyclophosphamide is a highly toxic alkylating agent that depletes T and B cells and suppresses antibody production.93 It is available as 25 mg and 50 mg tablets and as an injection.94 In the past, it was widely used for LN and severe lupus in the central nervous system.95,96 However, currently, it has been replaced by less toxic immunosuppressive medications such as mycophenolate mofetil, calcineurin inhibitors, and azathioprine. Cyclophosphamide is associated with premature ovarian failure, hemorrhagic cystitis, increased risk of bladder and other malignancies, along with leukopenia an increased risk of infections.97
Mycophenolate mofetil (MMF) has similar efficacy as cyclophosphamide but with a better safety profile. It is available as 250 mg capsules and 500 mg tablets, 35 mg powder for oral suspension (200 mg/ml when reconstituted), and injection.98 It preferentially depletes guanoside nucleotides in T and B cells, inhibiting proliferation and suppressing lymphocyte and monocyte recruitment to the inflamed tissue.99 Mycophenolate mofetil is effective for the induction and maintenance of LN nephritis and is superior to azathioprine in preventing nephritis relapses.13,100
Azathioprine (AZA) is a purine analog that inhibits DNA and RNA synthesis, preventing lymphocyte proliferation in the immune system. It is used as a steroid-sparing agent in moderate to severe lupus and in the maintenance phase of LN.82,88 Azathioprine is a safe immunosuppressant to control renal and extrarenal disease during pregnancy since its prodrug 6-MMP is associated with hepatotoxicity and
myelotoxicity is not generated in the fetus.58,101 Azathioprine can be dosed as 2 mg/kg/day.102
Methotrexate (MTX) is an antifolate metabolite that interferes with DNA synthesis, repair, and replication.103 Methotrexate is commonly used as an anti-inflammatory agent to treat rheumatoid arthritis. It has been dosed as 15-20 mg/week (preferably subcutaneously).104 In lupus, the drug reduces disease activity, acts as a corticosteroid-sparing agent, has efficacy for joint and skin disease, and lowers anti-dsDNA and complement levels.105 Side effects include nausea, mouth sores, blood problems, liver damage, and moderate hair loss. Prolonged treatment with methotrexate may also lead to folic acid deficiency.106
Calcineurin inhibitors such as tacrolimus target T cells by blocking the inhibition of calcineurin, which results in a reduction of inflammatory cytokines IL-1b, IFN-γ, IL-6, and IL-10. B cell activation is also impaired along with class switching and immunoglobulin production.107 Combination of tacrolimus and mycophenolate is an effective therapy for refractory LN, maintenance LN, and pure membranous LN with a significant antiproteinuric effect.97,108,109 Voclosporin is a newly approved calcineurin inhibitor that has greater pharmacological potency in active LN with a higher complete remission rate than mycophenolate.110 Before initiating it, an accurate baseline estimated glomerular filtration rate (eGFR) should be established, and blood pressure (BP) checked. Voclosporin must be swallowed whole on an empty stomach. It is administered as close to a 12-hour schedule as possible, and with at least 8 hours between doses. Grapefruit or grapefruit juice should be avoided. It is available as a 7.9 mg dose. The recommended starting dose is 23.7 mg orally, twice a day. It is used in combination with mycophenolate mofetil (MMF) and corticosteroids. Reduced dosing is recommended for hepatic or renal insufficiency.111
Biologics and small molecules
Belimumab is a human monoclonal antibody with a unique mechanism of action that blocks the biologic activity of B-lymphocyte stimulator (BLyS/BAFF). This decreases the antibody levels in the body, leading to a reduction of the autoimmune activity of SLE.112 Belimumab is the first FDA-approved drug for active lupus and LN in adults and children (age
5 and above) and for patients with autoantibody-positive SLE receiving standard therapy.113 In clinical trials, it demonstrated a steroid-sparing effect, decreased rate of flares, and good safety profile.114 The intravenous dosage for adult and pediatric patients with SLE or LN is 10 mg/kg at 2-week intervals for the first 3 doses and at 4-week intervals thereafter. It is reconstituted, diluted, and administered as an intravenous infusion over a period of 1 hour. The subcutaneous (subq) dosage for adults with SLE is 200 mg once weekly. The subq dosage for adults with LN is 400 mg (two 200-mg injections) once weekly for 4 doses, then 200 mg once weekly thereafter.
Rituximab is a humanized chimeric mouse/human monoclonal antibody that targets B-cell-specific antigen CD20. It leads to peripheral B-cell depletion of autoreactive B-cells in the circulation of patients with SLE. Although not approved by the FDA, it is often used off-label for severe refractory SLE.115 Several observational studies showed benefits in renal and non-renal lupus.116,117
Anifrolumab is a monoclonal antibody that inhibits excess interferon activation by blocking type I IFN-α/β/ω receptor (IFNAR). The effect is greater in SLE patients with high interferon signature at baseline.118 Treatment is associated with decreased anti-dsDNA titers and higher C3 levels. However, common adverse events are present such as upper respiratory and urinary infections as well as shingles.119 Anifrolumab has been recently approved by FDA for the treatment of patients with moderate-to-severe SLE.120 The recommended dosage is 300 mg as an intravenous infusion over a 30-minute period every 4 weeks. Patients are informed that they should not receive live or live-attenuated vaccines while receiving anifrolumab.121
Ustekinumab is a fully human monoclonal antibody that inhibits p40 subunit of Interleukin (IL)-12 and IL-23. Results of Phase II open-label study in patients with active SLE demonstrated clinical benefit in global and organ-specific measures with no adverse safety findings.122 Subgroup analysis showed significant improvement in skin and joint scores, improved C3, and reduced anti-dsDNA levels.122 However, more recent data from Phase III randomized, placebo-controlled study did not demonstrate superiority over placebo in adults with active SLE.123
Baricitinib is an orally administered, small-molecule, Janus-associated kinase (JAK) inhibitor. JAK1 and JAK2 mediate signaling for type 1 interferons, IFN-γ, IL-6, IL-12, and IL-23, among several other cytokines. Baricitinib is currently approved for the treatment of rheumatoid arthritis. In SLE results of a 24-week Phase II in patients receiving baricitinib at 4 mg showed significant improvement in SLE activity. Recent data from a 52-week Phase III clinical trial, however, indicates that despite meeting the primary endpoints, treatment with baricitinib at 4 mg did not meet secondary endpoints and was associated with serious adverse events.124
Atacicept is a TACI-Ig fusion protein that inhibits B cells by dual inhibition of APRIL and BAFF, the two key factors produced by a variety of cells, including monocytes, dendritic cells, and T cells that help to regulate B cell maturation. A Phase II/III randomized clinical trial in patients with active LN on immunosuppressive therapy failed to evaluate the efficacy and safety of atacicept due to an unexpected decline in serum IgG and serious infections.125
Management of Flares
Relapses or flares are frequently observed in 27–66% of patients with SLE. Management of flares involves mitigation of risk factors that may trigger flare-ups such as environmental, hormonal, or medication-related toxic effects. Effective therapy targeting low-disease activity or remission has the potential to decrease the frequency and severity of lupus flares.52 Typically, patients stable on treatment experiencing lupus flare, are temporarily given high-dose corticosteroids to reduce inflammation. Nephritic flares are common in patients with proliferative LN, and these are usually controlled with pulse immunosuppressive therapy.126 Mycophenolate mofetil and azathioprine treatment are effective for renal, proteinuric, and nephritic flares.127 Data from meta-analysis studies indicates that mycophenolate mofetil is superior to azathioprine in preventing LN flares during maintenance.128 Belimumab decreases severe SLE flares while reducing prednisone dependence.114 Reduced risk of cumulative damage and flares are also routinely mitigated with hydroxychloroquine.129 Tacrolimus is relatively safe and effective in treating lupus flares during pregnancy.130 In addition, intramuscular
triamcinolone, or a brief 1-week methylprednisolone is effective for the management of most mild to moderate flares.13
Management of Depression
The neuropsychological symptoms, including anxiety, psychiatric and mood disorders associated with depression, are frequent in 45–65% of patients with SLE.131 Lupus patients also have a higher risk of suicidal tendencies than the general population.132 Such symptoms are attributed to either the psychosocial impact of the disease or to the presence of lesions in the central nervous system.132 Management of depression in SLE depends on whether it is diagnosed as a neurological disease (e.g., inflammation of the brain, stroke, seizure, presence of autoantibodies, elevated cytokines) or as a psychological disorder where signs of neurological disease are absent. Behavioral interventions such as targeted referrals to patient educators, mental health professionals, and support organizations in adjunct to antidepressant treatment are used to manage the neuropsychological symptoms.133 Cognitive behavioral stress management techniques have resulted in short-term improvement in pain, psychological function, and perceived physical function in SLE.134
The neurological basis of depression in SLE is attributed to multiple factors involving alteration of neurotransmitters bioavailability, overstimulation of neural circuits, cytokines, modification of neuroplasticity, and neurogenesis; all these can cause mood swings and depression.135 SLE patients with neurological cases are treated with glucocorticoids, immunosuppressants, and antidepressants.136 Combination of celecoxib (anti- inflammatory) and fluoxetine (antidepressant) has been reported to have a greater effect than fluoxetine alone.137 Electroconvulsive therapy (ECT) can be used in severe cases of patients who do not respond to the maximum therapy.138 Overall, most SLE patients with depression recover within a year with the help of social support along with medical care.132
Counseling Patients with Lupus
Social workers and clinical practitioners play a central role in helping patients with SLE to cope with the diagnosis and manifestations of this complex and highly individualized disease. To develop effective counseling and intervention strategies, they must learn how lupus affects the physical, psychological, and social functioning of patients and their families. The most commonly reported problems in lupus include depressed feelings, reduced physical activity, stress, and changes in body image. These fall in the areas of
(i) emotional aspects, (ii) lack of information, (iii) lifestyle restrictions, and
(iv) lack of information regarding exercise and diet.139 These four factors are identified and used as specific educational themes in developing education programs for SLE patients. Along with medical management, practitioners working with SLE patients should consider approaches such as patient- centered narrative and strengths-based perspective.140 The counselor’s role is to assist individuals in learning positive ways of adapting to the realities of living with an ongoing disease with chronic symptoms. It is important for the social worker and the health care practitioner to help patients with lupus accept, adjust, and develop a plan for living for the future.
Pharmacy team members can support an interdisciplinary approach to care by creating a rapport with patients, fully explaining all medications, and emphasizing adherence. Patients should be encouraged to minimize direct exposure to the sun, use SPF 30 and higher sunscreen, and be aware of medications that increase sensitivity to the sun. Counseling on photosensitivity is also appropriate for patients with lupus who have skin of color, including African American, Hispanic, Asian, and Native American populations.141 Patients with lupus can be encouraged to seek interpersonal and social support. Patient counseling may include inquiring whether any daily activities contribute to fatigue and encouraging individuals to get enough sleep. Patients with nutrition-related lupus complications should be referred to a dietician for counseling.
Gap Analysis of Current Versus Best Practices for Management of SLE
The diverse nature of SLE poses great challenges to research and drug development efforts. Treatment of SLE is highly individualized and depends on a specific patient’s profile that considers diagnosis, disease activity, and prediction of disease course and flares. Autoantibodies and immune complex formation are the immunological hallmarks of lupus. Due to this, B cells have been targeted in SLE for many years with immunosuppressants such as cyclophosphamide and mycophenolate. Recent improvements in patient care and the use of immunosuppressives with corticosteroids have changed the course of SLE. Survival has improved dramatically over the past 5 decades from a 5-year survival of 50% to a 15-year survival of 85% with current medical regimens.142 Despite such advances, further improvement in survival has mostly stalled, and the rate of progression to renal failure has not improved.143 LN is the most common severe organ-threatening manifestation of SLE that causes high morbidity and mortality however, only 20-30% of LN patients achieve complete remission with the current treatment paradigm.144,145 During the past decade, novel combinations of immunosuppressive drugs and biologicals have been added to the therapeutic armamentarium, including anifrolumab for moderate to severe SLE and belimumab and voclosporin for active LN.110,113,120 Antimalarials are currently the basic treatment for every patient with SLE, whereas glucocorticoids are only used when acutely indicated.104 Adjunct treatment is almost as important as immunosuppression and is a comedication, which is determined by the comorbidity type (e.g., infection, arteriosclerosis, hypertension, dyslipidemia, diabetes, osteoporosis, avascular necrosis, and malignancy, among others).104
The emphasis in the management of lupus has shifted from individual drugs to a strategy that aims at early, sustained remission tailored to disease manifestations and severity with the lowest possible toxicity. Infections and accelerated atherosclerosis (attributed to both traditional and non-traditional risk factors) and thrombosis-related clinical events (including arterial, venous, and pregnancy loss) still represent a major challenge in the management of the disease. Treatment goals for SLE currently include long-term patient survival, prevention of organ damage, and optimization of health-related quality of life.
Future Approaches to Managing Lupus
Future perspectives for the management of SLE/lupus will be designed as individualized treatments depending on the presenting symptoms and disease progression of each patient. The goal is to develop a personalized plan geared to lessen the impact of the disease on a patient's life. Biologic compounds that target specific immunologic mechanisms offer a new paradigm in the treatment of SLE. At best, these could reverse the course of the disease and, at the very least, could provide new alternatives to reduce symptoms and limit tissue damage without contributing to overall morbidity and mortality. Strategies using genomics and proteomics will aid in identifying new biomarkers that can be used for early disease detection and treatment.
Summary
Systemic lupus erythematosus is a challenging and disabling autoimmune disease affecting many organs. Multiple biological mechanisms contribute to the development and progression of the disease. Clinical manifestations can be both systemic and organ-specific depending on the type of disease. Systemic lupus erythematosus is associated with frequent flares and relapses that are often triggered by risk factors. Special populations such as pregnant women and pediatric patients with SLE are particularly at risk of developing adverse effects. Advances in research and drug development have led to target-specific effective and less toxic therapeutics. The goal of SLE treatment is to achieve long-term remission, reduce morbidity/mortality and improve quality of life. This could be attained through broad efforts of basic, translational, and clinical scientists, clinicians, patient counselors, patients, and their families, and everyone engaged in the lupus community.
Course Test
What is a laboratory test utilized for the diagnosis of SLE?
blood test for antinuclear antibodies
radiographic X-ray, CT, and MRI
ophthalmic retina biopsy
PCR COVID test
Which of the following is not a drug that has been prescribed for the treatment of SLE?
Cyclophosphamide
Belimumab
Hydrazine
Hydroxychloroquine
Which of the following SLE patient populations is more at risk of developing a new diagnosis of SLE and adverse outcomes?
Pregnant women
80-year-old African American
3-year-old Hispanic/Latino
90-year-old Asian
Which of the following statements is correct?
A minimum of 6 out of 11 ACR criteria ought to be met for a diagnosis of SLE.
Positive antinuclear antibody is not an ACR criteria for diagnosis of SLE.
Systemic Lupus Erythematosus Disease Activity Index (SLEDAI) and SLEDAI-2K are the criteria.
Lupus is a chronic, progressive autoimmune disorder in which the immune system attacks its own healthy tissues.
Which of the following biologics is used to decrease severe SLE flares with an intravenous or subcutaneous dosing option?
Anifrolumab
Ustekinumab
Belimumab
Rituximab
Which of the following statements is correct?
Management of depression in SLE depends on whether it is diagnosed as a neurological disease or behavioral disorder.
The neuropsychological symptoms of SLE include anxiety, depression, psychiatric and mood disorders.
SLE patients with neurological cases are treated with glucocorticoids, immunosuppressants, and antidepressants.
All of the above
The most common side effect associated with the use of NSAIDs in SLE is:
Vascular thrombosis
Gastrointestinal bleeding
Immune tolerance
Renal toxicity
Which 2 of the following novel drugs has been recently approved for SLE by FDA?
Cyclosporine and erythromycin
Voclosporin and belimumab
Anifrolumab and methotrexate
Timolol and aspirin
Future approaches for the development of new SLE drugs could include
individualized treatment depending on the presenting symptoms and disease progression of each patient.
only achieve short-term remission with new autoantibodies.
new anti-inflammatory cytokines because all lupus cases appear suddenly.
new aromatic amines because only amines prevent all photosensitivity.
Which of the following risk factors creates a predisposition to SLE?
Environmental triggers
Heritability
Autoimmune diseases
All of the above
References
Systemic Lupus Erythematosus (Lupus). National Institute of Arthritis and Musculoskeletal and Skin Diseases. Published October 2022.https://www.niams.nih.gov/health-topics/lupus. Accessed May 25, 2023.
Bertsias G, Ioannidis JPA, Boletis J, et al. EULAR recommendations for the management of systemic lupus erythematosus. Report of a Task Force of the EULAR Standing Committee for International Clinical Studies Including Therapeutics. Ann Rheum Dis. 2008;67(2):195-205. doi:10.1136/ard.2007.070367
Sam Lim S, Drenkard C, McCune WJ, et al. Population-based lupus registries: Advancing our epidemiologic understanding. Arthritis Rheum. 2009;61(10):1462-1466. doi:10.1002/art.24835
Lewis MJ, Jawad AS. The effect of ethnicity and genetic ancestry on the epidemiology, clinical features and outcome of systemic lupus erythematosus. Rheumatology. Published online December 10, 2016:kew399. doi:10.1093/rheumatology/kew399
Pons-Estel BA, Bonfa E, Soriano ER, et al. First Latin American clinical practice guidelines for the treatment of systemic lupus erythematosus: Latin American Group for the Study of Lupus (GLADEL, Grupo Latino Americano de Estudio del Lupus )–Pan-American League of Associations of Rheumatology (PANLAR). Ann Rheum Dis. 2018;77(11):1549-1557. doi:10.1136/annrheumdis-2018-213512
Ferucci ED, Johnston JM, Gaddy JR, et al. Prevalence and Incidence of Systemic Lupus Erythematosus in a Population-Based Registry of American Indian and Alaska Native People, 2007-2009. Arthritis & Rheumatology. 2014;66(9):2494-2502. doi:10.1002/art.38720
Petri M. Epidemiology of systemic lupus erythematosus. Best Pract Res Clin Rheumatol. 2002;16(5):847-858. doi:10.1053/berh.2002.0259
Danchenko N, Satia JA, Anthony MS. Epidemiology of systemic lupus erythematosus: a comparison of worldwide disease burden. Lupus. 2006;15(5):308-318. doi:10.1191/0961203306lu2305xx
Krishnan E, Hubert HB. Ethnicity and mortality from systemic lupus erythematosus in the US. Ann Rheum Dis. 2006;65(11):1500-1505. doi:10.1136/ard.2005.040907
Porth C, Matfin G. Pathophysiology: Concepts of Altered Health States. 8th ed. (Pooler C, ed.). Wolters Kluwer Health/Lippincott Williams & Wilkins; 2009.
Schur P, Gladman DD. Overview of the Clinical Manifestations of Systemic Lupus Erythematosus in Adults. (Basow DS, ed.). UpToDate. Waltham, MA; 2012.
Tsokos GC, Lo MS, Reis PC, Sullivan KE. New insights into the immunopathogenesis of systemic lupus erythematosus. Nat Rev Rheumatol. 2016;12(12):716-730. doi:10.1038/nrrheum.2016.186
Fava A, Petri M. Systemic lupus erythematosus: Diagnosis and clinical management. J Autoimmun. 2019;96:1-13. doi:10.1016/j.jaut.2018.11.001
Rekvig OP, Van der Vlag J. The pathogenesis and diagnosis of systemic lupus erythematosus: still not resolved. Semin Immunopathol. 2014;36(3):301-311. doi:10.1007/s00281-014-0428-6
Rekvig OP. Systemic Lupus Erythematosus: Definitions, Contexts, Conflicts, Enigmas. Front Immunol. 2018;9. doi:10.3389/fimmu.2018.00387
Johns Hopkins Lupus Center. Types of Lupus. Undated. https://www.hopkinslupus.org/lupus-info/types-lupus/. Accessed June 10, 2023.
Mok CC. Pathogenesis of systemic lupus erythematosus. J Clin Pathol. 2003;56(7):481-490. doi:10.1136/jcp.56.7.481
Rekvig OP. The anti-DNA antibody: origin and impact, dogmas and controversies. Nat Rev Rheumatol. 2015;11(9):530-540. doi:10.1038/nrrheum.2015.69
Foster M, Cizman B, Madaio M. Nephritogenic autoantibodies in systemic lupus erythematosus: immunochemical properties, mechanisms of immune deposition, and genetic origins. Lab Invest. 1993;69(5):494-507. https://europepmc.org/article/med/8246442.
Accessed May 25, 2023.
Weening JJ, D’agati VD, Schwartz MM, et al. The classification of glomerulonephritis in systemic lupus erythematosus revisited. Kidney Int. 2004;65(2):521-530. doi:10.1111/j.1523-1755.2004.00443.x
La Cava A. Lupus and T Cells. Lupus. 2009;18(3):196-201. doi:10.1177/0961203308098191
Nashi E, Wang Y, Diamond B. The role of B cells in lupus pathogenesis. Int J Biochem Cell Biol. 2010;42(4):543-550. doi:10.1016/j.biocel.2009.10.011
Dhir V, Singh A, Aggarwal A, Naik S, Misra R. Increased T-lymphocyte apoptosis in lupus correlates with disease activity and may be responsible for reduced T-cell frequency: a cross-sectional and longitudinal study. Lupus. 2009;18(9):785-791. doi:10.1177/0961203309103152
Bakke AC, Kirkland PA, Kitridou RC, et al. T Lymphocyte Subsets in Systemic Lupus Erythematosus. Arthritis Rheum. 1983;26(6):745-750. doi:10.1002/art.1780260607
Katsuyama T, Tsokos GC, Moulton VR. Aberrant T Cell Signaling and Subsets in Systemic Lupus Erythematosus. Front Immunol. 2018;9. doi:10.3389/fimmu.2018.01088
Baechler EC, Batliwalla FM, Karypis G, et al. Interferon-inducible gene expression signature in peripheral blood cells of patients with severe lupus. Proceedings of the National Academy of Sciences. 2003;100(5):2610-2615. doi:10.1073/pnas.0337679100
Bennett L, Palucka AK, Arce E, et al. Interferon and Granulopoiesis Signatures in Systemic Lupus Erythematosus Blood. Journal of Experimental Medicine. 2003;197(6):711-723. doi:10.1084/jem.20021553
Langefeld CD, Ainsworth HC, Graham DSC, et al. Transancestral mapping and genetic load in systemic lupus erythematosus. Nat Commun. 2017;8(1):16021. doi:10.1038/ncomms16021
Kwon, Chun, Kim, Mak. Update on the Genetics of Systemic Lupus Erythematosus: Genome-Wide Association Studies and Beyond. Cells. 2019;8(10):1180. doi:10.3390/cells8101180
Tsao BP. An update on genetic studies of systemic lupus erythematosus. Curr Rheumatol Rep. 2002;4(4):359-367. doi:10.1007/s11926-002-0046-5
Gray-McGuire C, Moser KL, Gaffney PM, et al. Genome Scan of Human Systemic Lupus Erythematosus by Regression Modeling: Evidence of Linkage and Epistasis at 4p16-15.2. The American Journal of Human Genetics. 2000;67(6):1460-1469. doi:10.1086/316891
Generali E, Ceribelli A, Stazi MA, Selmi C. Lessons learned from twins in autoimmune and chronic inflammatory diseases. J Autoimmun. 2017;83:51-61. doi:10.1016/j.jaut.2017.04.005
Ghodke-Puranik Y, Niewold TB. Immunogenetics of systemic lupus erythematosus: A comprehensive review. J Autoimmun. 2015;64:125-
136. doi:10.1016/j.jaut.2015.08.004
Schur PH. Review: Genetics of systemic lupus erythematosus. Lupus. 1995;4(6):425-437. doi:10.1177/096120339500400603
Pickering MC, Walport MJ. Links between complement abnormalities and systemic lupus erythematosus. Rheumatology. 2000;39(2):133-141. doi:10.1093/rheumatology/39.2.133
Casciola-Rosen LA, Anhalt G, Rosen A. Autoantigens targeted in systemic lupus erythematosus are clustered in two populations of surface structures on apoptotic keratinocytes. Journal of Experimental Medicine. 1994;179(4):1317-1330. doi:10.1084/jem.179.4.1317
Casciola-Rosen L, Rosen A, Petri M, Schlissel M. Surface blebs on apoptotic cells are sites of enhanced procoagulant activity: implications for coagulation events and antigenic spread in systemic lupus erythematosus. Proceedings of the National Academy of Sciences. 1996;93(4):1624-1629. doi:10.1073/pnas.93.4.1624
Salmon JE, Millard S, Schachter LA, et al. Fc gamma RIIA alleles are heritable risk factors for lupus nephritis in African Americans. Journal of Clinical Investigation. 1996;97(5):1348-1354. doi:10.1172/JCI118552
Kim JW, Kim HA, Suh CH, Jung JY. Sex hormones affect the pathogenesis and clinical characteristics of systemic lupus erythematosus. Front Med (Lausanne). 2022;9. doi:10.3389/fmed.2022.906475
Lahita RG, Leon Bradlow H, Kunkel HG, Fishman J. Alterations of estrogen metabolism in systemic lupus erythematosus. Arthritis Rheum. 1979;22(11):1195-1198. doi:10.1002/art.1780221106
Jungers P, Nahoul K, Pelissier C, Dougados M, Tron F, Bach JF. Low plasma androgens in women with active or quiescent systemic lupus erythematosus. Arthritis Rheum. 1982;25(4):454-457. doi:10.1002/art.1780250415
Lahita RG, Bradlow HL, Ginzler E, Pang S, New M. Low plasma androgens in women with systemic lupus erythematosus. Arthritis Rheum. 1987;30(3):241-248. doi:10.1002/art.1780300301
Smith EL, Shmerling RH. The American College of Rheumatology criteria for the classification of systemic lupus erythematosus: Strengths, weaknesses, and opportunities for improvement. Lupus.
1999;8(8):586-595. doi:10.1191/096120399680411317
Gladman D, Ibanez D, Urowitz M. Systemic Lupus Erythematosus Disease Activity Index 2000. J Rheumatology. 2002;2:288-291. https://pubmed.ncbi.nlm.nih.gov/11838846/. Accessed May 26, 2023.
Bernknopf A, Rowley K, Bailey T. A review of systemic lupus erythematosus and current treatment options. Formulary. 2011;46(5):178-194.
Egner W. The use of laboratory tests in the diagnosis of SLE. J Clin Pathol. 2000;53(6):424-432. doi:10.1136/jcp.53.6.424
Lazaro D. Elderly-Onset Systemic Lupus Erythematosus. Drugs Aging. 2007;24(9):701-715. doi:10.2165/00002512-200724090-00001
Jiménez S, Cervera R, Font J, Ingelmo M. The Epidemiology of Systemic Lupus Erythematosus. Clin Rev Allergy Immunol. 2003;25(1):3-12. doi:10.1385/CRIAI:25:1:3
Weening JJ, D’agati VD, Schwartz MM, et al. The classification of glomerulonephritis in systemic lupus erythematosus revisited. Kidney Int. 2004;65(2):521-530. doi:10.1111/j.1523-1755.2004.00443.x
Xiong H, Tang Z, Xu Y, et al. CD19+CD24highCD27+ B cell and interleukin 35 as potential biomarkers of disease activity in systemic lupus erythematosus patients. Advances in Rheumatology. 2022;62(1):48. doi:10.1186/s42358-022-00279-8
Gurevitz SL, Snyder JA, Wessel EK, Frey J, Williamson BA. Systemic Lupus Erythematosus: A Review of the Disease and Treatment Options. The Consultant Pharmacist. 2013;28(2):110-121. doi:10.4140/TCP.n.2013.110
Fanouriakis A, Tziolos N, Bertsias G, Boumpas DT. Update οn the diagnosis and management of systemic lupus erythematosus. Ann Rheum Dis. 2021;80(1):14-25. doi:10.1136/annrheumdis-2020-218272
Amissah A, Maame B, Gordon C. GPS Have Key Role in Shared Care of Patients with SLE. Vol 253. Gale Academic OneFile; 2009.
Gordon C, Jayne D, Pusey C, et al. European consensus statement on the terminology used in the management of lupus glomerulonephritis. Lupus. 2009;18(3):257-263. doi:10.1177/0961203308100481
Fanouriakis A, Kostopoulou M, Cheema K, et al. 2019 Update of the Joint European League Against Rheumatism and European Renal Association–European Dialysis and Transplant Association (EULAR/ERA– EDTA) recommendations for the management of lupus nephritis. Ann Rheum Dis. 2020;79(6):713-723. doi:10.1136/annrheumdis-2020- 216924
Clowse MEB, Jamison M, Myers E, James AH. A national study of the complications of lupus in pregnancy. Am J Obstet Gynecol. 2008;199(2):127.e1-127.e6. doi:10.1016/j.ajog.2008.03.012
Chakravarty EF, Nelson L, Krishnan E. Obstetric hospitalizations in the United States for women with systemic lupus erythematosus and rheumatoid arthritis. Arthritis Rheum. 2006;54(3):899-907. doi:10.1002/art.21663
Lateef A, Petri M. Systemic Lupus Erythematosus and Pregnancy. Rheumatic Disease Clinics of North America. 2017;43(2):215-226. doi:10.1016/j.rdc.2016.12.009
Petri M. Pregnancy and Systemic Lupus Erythematosus. Best Pract Res Clin Obstet Gynaecol. 2020;64:24-30. doi:10.1016/j.bpobgyn.2019.09.002
Moroni G, Doria A, Giglio E, et al. Maternal outcome in pregnant women with lupus nephritis. A prospective multicenter study. J Autoimmun. 2016;74:194-200. doi:10.1016/j.jaut.2016.06.012
Moroni G, Doria A, Giglio E, et al. Fetal outcome and recommendations of pregnancies in lupus nephritis in the 21st century. A prospective multicenter study. J Autoimmun. 2016;74:6-12. doi:10.1016/j.jaut.2016.07.010
Nahal SK, Selmi C, Gershwin ME. Safety issues and recommendations for successful pregnancy outcome in systemic lupus erythematosus. J Autoimmun. 2018;93:16-23. doi:10.1016/j.jaut.2018.07.016
Wu J, Ma J, Zhang W, Di W. Management and outcomes of pregnancy with or without lupus nephritis: a systematic review and meta-analysis. Ther Clin Risk Manag. 2018;Volume 14:885-901. doi:10.2147/TCRM.S160760
Moroni G, Ponticelli C. Pregnancy in women with systemic lupus erythematosus (SLE). Eur J Intern Med. 2016;32:7-12. doi:10.1016/j.ejim.2016.04.005
Smyth A, Oliveira GHM, Lahr BD, Bailey KR, Norby SM, Garovic VD. A Systematic Review and Meta-Analysis of Pregnancy Outcomes in Patients with Systemic Lupus Erythematosus and Lupus Nephritis. Clinical Journal of the American Society of Nephrology. 2010;5(11):2060-2068. doi:10.2215/CJN.00240110
Buyon JP, Kim MY, Salmon JE. Predictors of Pregnancy Outcomes in Patients With Lupus. Ann Intern Med. 2016;164(2):131. doi:10.7326/L15-0500
Jara LJ, Medina G, Cruz-Dominguez P, Navarro C, Vera-Lastra O, Saavedra MA. Risk factors of systemic lupus erythematosus flares during pregnancy. Immunol Res. 2014;60(2-3):184-192. doi:10.1007/s12026-014-8577-1
Yelnik CM, Laskin CA, Porter TF, et al. Lupus anticoagulant is the main predictor of adverse pregnancy outcomes in aPL-positive patients: validation of PROMISSE study results. Lupus Sci Med. 2016;3(1):e000131. doi:10.1136/lupus-2015-000131
Tincani A, Bazzani C, Zingarelli S, Lojacono A. Lupus and the Antiphospholipid Syndrome in Pregnancy and Obstetrics: Clinical Characteristics, Diagnosis, Pathogenesis, and Treatment. Semin Thromb Hemost. 2008;34(03):267-273. doi:10.1055/s-0028-1082270
Cortes-Hernandez J. Clinical predictors of fetal and maternal outcome in systemic lupus erythematosus: a prospective study of 103 pregnancies. Rheumatology. 2002;41(6):643-650. doi:10.1093/rheumatology/41.6.643
Papadimitraki ED, Isenberg DA. Childhood- and adult-onset lupus: an update of similarities and differences. Expert Rev Clin Immunol. 2009;5(4):391-403. doi:10.1586/eci.09.29
Mina R, Brunner HI. Update on differences between childhood-onset and adult-onset systemic lupus erythematosus. Arthritis Res Ther. 2013;15(4):218. doi:10.1186/ar4256
Pradhan V, Patwardhan M, Rajadhyaksha A, Ghosh K. Clinical and immunological profile of systemic lupus erythematosus. Indian Pediatr. 2013;50(4):405-407. doi:10.1007/s13312-013-0115-z
Brunner HI, Silverman ED, To T, Bombardier C, Feldman BM. Risk factors for damage in childhood-onset systemic lupus erythematosus: Cumulative disease activity and medication use predict disease damage. Arthritis Rheum. 2002;46(2):436-444. doi:10.1002/art.10072
Hiraki LT, Benseler SM, Tyrrell PN, Hebert D, Harvey E, Silverman ED. Clinical and Laboratory Characteristics and Long-Term Outcome of Pediatric Systemic Lupus Erythematosus: A Longitudinal Study. J Pediatr. 2008;152(4):550-556. doi:10.1016/j.jpeds.2007.09.019
Bader-Meunier B, Armengaud JB, Haddad E, et al. Initial presentation of childhood-onset systemic lupus erythematosus: A French multicenter
study. J Pediatr. 2005;146(5):648-653. doi:10.1016/j.jpeds.2004.12.045
Brunner HI, Gladman DD, Ibañez D, Urowitz MD, Silverman ED. Difference in disease features between childhood-onset and adult-onset systemic lupus erythematosus. Arthritis Rheum. 2008;58(2):556-562. doi:10.1002/art.23204
Vyas S, Hidalgo G, Baqi N, Von Gizyki H, Singh A. Outcome in African- American children of neuropsychiatric lupus and lupus nephritis. Pediatric Nephrology. 2002;17(1):45-49. doi:10.1007/s004670200008
Stichweh D, Arce E, Pascual V. Update on pediatric systemic lupus erythematosus. Curr Opin Rheumatol. 2004;16(5):577-587. doi:10.1097/01.bor.0000137852.42270.0f
TUCKER LB, MENON S, SCHALLER JG, ISENBERG DA. ADULT- AND CHILDHOOD-ONSET SYSTEMIC LUPUS ERYTHEMATOSUS: A COMPARISON OF ONSET, CLINICAL FEATURES, SEROLOGY, AND OUTCOME. Rheumatology. 1995;34(9):866-872.
doi:10.1093/rheumatology/34.9.866
FELDENE® (piroxicam) [Prescribing Information]. Pfizer Laboratories. Published November 2022. https://labeling.pfizer.com/showlabeling.aspx?format=PDF&id=569. Accessed June 5, 2023.
Amissah-Arthur MB, Gordon C. Contemporary treatment of systemic lupus erythematosus: an update for clinicians. Ther Adv Chronic Dis. 2010;1(4):163-175. doi:10.1177/2040622310380100
Sostres C, Gargallo CJ, Arroyo MT, Lanas A. Adverse effects of non- steroidal anti-inflammatory drugs (NSAIDs, aspirin and coxibs) on upper gastrointestinal tract. Best Pract Res Clin Gastroenterol. 2010;24(2):121-132. doi:10.1016/j.bpg.2009.11.005
CELEBREX® (celecoxib) [Prescribing Information]. Pfizer Laboratories. Published April 2021. https://dailymed.nlm.nih.gov/dailymed/fda/fdaDrugXsl.cfm?setid=8d52 185d-421f-4e34-8db7-f7676db2a226&type=display. Accessed June 5, 2023.
Andreoli L, Bertsias GK, Agmon-Levin N, et al. EULAR recommendations for women’s health and the management of family planning, assisted reproduction, pregnancy and menopause in patients with systemic lupus erythematosus and/or antiphospholipid syndrome. Ann Rheum Dis. 2017;76(3):476-485. doi:10.1136/annrheumdis-2016-209770
Gladman D. Guidelines for referral and management of systemic lupus erythematosus in adults. Arthritis & Rheum. 1999;42:1785-1796.
Fessler BJ, Alarcón GS, McGwin G, et al. Systemic lupus erythematosus in three ethnic groups: XVI. Association of hydroxychloroquine use with reduced risk of damage accrual. Arthritis Rheum. 2005;52(5):1473- 1480. doi:10.1002/art.21039
Yildirim-Toruner C, Diamond B. Current and novel therapeutics in the treatment of systemic lupus erythematosus. Journal of Allergy and Clinical Immunology. 2011;127(2):303-312. doi:10.1016/j.jaci.2010.12.1087
Alarcon GS, McGwin G, Bertoli AM, et al. Effect of hydroxychloroquine on the survival of patients with systemic lupus erythematosus: data from LUMINA, a multiethnic US cohort (LUMINA L). Ann Rheum Dis. 2007;66(9):1168-1172. doi:10.1136/ard.2006.068676
Ruiz-Irastorza G, Egurbide MV, Pijoan JI, et al. Effect of antimalarials on thrombosis and survival in patients with systemic lupus erythematosus. Lupus. 2006;15(9):577-583. doi:10.1177/0961203306071872
PLAQUENIL (hydroxychloroquine sulfate) [Prescribing Information]. Concordia Pharmaceuticals. Published May 2021. https://www.accessdata.fda.gov/drugsatfda_docs/label/2021/009768s0 53lbl.pdf. Accessed June 5, 2023.
medications/steroids/. Accessed June 5, 2023.
Frangou EA, Bertsias G, Boumpas DT. Cytotoxic-Immunosuppressive Drug Treatment. In: Systemic Lupus Erythematosus. Elsevier; 2016:533-541. doi:10.1016/B978-0-12-801917-7.00062-0
CYCLOPHOSPHAMIDE [Prescribing Information]. Baxter Healthcare. Published August 2020. https://www.baxterpi.com/pi- pdf/Cyclophosphamide%20Tablets%20PI%20HA-30-01- 863%20Aug%202020.pdf. Accessed June 5, 2023.
Austin HA, Klippel JH, Balow JE, et al. Therapy of Lupus Nephritis. New England Journal of Medicine. 1986;314(10):614-619. doi:10.1056/NEJM198603063141004
McCune WJ, Golbus J, Zeldes W, Bohlke P, Dunne R, Fox DA. Clinical and Immunologic Effects of Monthly Administration of Intravenous Cyclophosphamide in Severe Systemic Lupus Erythematosus. New England Journal of Medicine. 1988;318(22):1423-1431. doi:10.1056/NEJM198806023182203
Mok CC, Ying KY, Yim CW, et al. Tacrolimus versus mycophenolate mofetil for induction therapy of lupus nephritis: a randomised controlled trial and long-term follow-up. Ann Rheum Dis. 2016;75(1):30-36. doi:10.1136/annrheumdis-2014-206456
CELLCEPT® (mycophenolate mofetil) [Prescribing Information]. Genentech (A Member of the Roche Group). Published August 2022. https://www.gene.com/download/pdf/cellcept_prescribing.pdf. Accessed June 5, 2023.
Allison A. Mechanisms of action of mycophenolate mofetil. Lupus. 2005;14(3_suppl):2-8. doi:10.1191/0961203305LU2109OA
Houssiau FA, D’Cruz D, Sangle S, et al. Azathioprine versus mycophenolate mofetil for long-term immunosuppression in lupus nephritis: results from the MAINTAIN Nephritis Trial. Ann Rheum Dis. 2010;69(12):2083-2089. doi:10.1136/ard.2010.131995
de Boer NKH, Jarbandhan SVA, de Graaf P, Mulder CJJ, van Elburg RM, van Bodegraven AA. Azathioprine Use During Pregnancy: Unexpected Intrauterine Exposure to Metabolites. Am J Gastroenterol. 2006;101(6):1390-1392. doi:10.1111/j.1572-0241.2006.00538.x
Fischer-Betz R, Specker C, Brinks R, Aringer M, Schneider M. Low risk of renal flares and negative outcomes in women with lupus nephritis conceiving after switching from mycophenolate mofetil to azathioprine. Rheumatology. 2013;52(6):1070-1076. doi:10.1093/rheumatology/kes425
Brown PM, Pratt AG, Isaacs JD. Mechanism of action of methotrexate in rheumatoid arthritis, and the search for biomarkers. Nat Rev Rheumatol. 2016;12(12):731-742. doi:10.1038/nrrheum.2016.175
Kuhn A, Bonsmann G, Anders HJ, Herzer P, Tenbrock K, Schneider M. The Diagnosis and Treatment of Systemic Lupus Erythematosus. Dtsch Arztebl Int. Published online June 19, 2015. doi:10.3238/arztebl.2015.0423
MIESCHER PA, RIETHMUELLER D. DIAGNOSIS AND TREATMENT OF SYSTEMIC LUPUS ERYTHEMATOSUS. Semin Hematol. 1965;2:1-28.
Lupus Medications. Lupus Canada. https://www.lupuscanada.org/resources/fact-sheets/lupus- medications/#:~:text=Methotrexate%20is%20convenient%20in%20th at,lead%20to%20folic%20acid%20deficiency. Accessed May 27, 2023.
Mok CC. Calcineurin inhibitors in systemic lupus erythematosus. Best Pract Res Clin Rheumatol. 2017;31(3):429-438. doi:10.1016/j.berh.2017.09.010
Chen W, Liu Q, Chen W, et al. Outcomes of maintenance therapy with tacrolimus versus azathioprine for active lupus nephritis: a multicenter randomized clinical trial. Lupus. 2012;21(9):944-952. doi:10.1177/0961203312442259
Lanata C, Mahmood T, Fine D, Petri M. Combination therapy of mycophenolate mofetil and tacrolimus in lupus nephritis. Lupus. 2010;19(8):935-940. doi:10.1177/0961203310365714
Rovin BH, Solomons N, Pendergraft WF, et al. A randomized, controlled double-blind study comparing the efficacy and safety of dose-ranging voclosporin with placebo in achieving remission in patients with active lupus nephritis. Kidney Int. 2019;95(1):219-231. doi:10.1016/j.kint.2018.08.025
LUPKYNIS (voclosporin) [Prescribing Information]. Aurinia Pharmaceuticals. Published January 2021.
https://d1io3yog0oux5.cloudfront.net/auriniapharma/files/pages/lupkyn
is-prescribing-information/FPI-0011+Approved+USPI++MG.pdf. Accessed June 5, 2023.
Kalunian K, Joan TM. New directions in the treatment of systemic lupus erythematosus. Curr Med Res Opin. 2009;25(6):1501-1514. doi:10.1185/03007990902929104
Benlysta® [prescribing information]. Human Genome Sciences, Inc. Published March 29, 2011. https://www.accessdata.fda.gov/drugsatfda_docs/label/2012/125370s0 16lbl.pdf. Accessed May 28, 2023.
Navarra S V, Guzmán RM, Gallacher AE, et al. Efficacy and safety of belimumab in patients with active systemic lupus erythematosus: a randomised, placebo-controlled, phase 3 trial. The Lancet. 2011;377(9767):721-731. doi:10.1016/S0140-6736(10)61354-2
Wise LM, Stohl W. Belimumab and Rituximab in Systemic Lupus Erythematosus: A Tale of Two B Cell-Targeting Agents. Front Med (Lausanne). 2020;7. doi:10.3389/fmed.2020.00303
Cobo-Ibáñez T, Loza-Santamaría E, Pego-Reigosa JM, et al. Efficacy and safety of rituximab in the treatment of non-renal systemic lupus erythematosus: A systematic review. Semin Arthritis Rheum. 2014;44(2):175-185. doi:10.1016/j.semarthrit.2014.04.002
Lan L, Han F, Chen J hua. Efficacy and safety of rituximab therapy for systemic lupus erythematosus: a systematic review and meta-analysis. J Zhejiang Univ Sci B. 2012;13(9):731-744. doi:10.1631/jzus.B1200057
Felten R, Scher F, Sagez F, Chasset F, Arnaud L. <p>Spotlight on anifrolumab and its potential for the treatment of moderate-to-severe systemic lupus erythematosus: evidence to date</p>. Drug Des Devel Ther. 2019;Volume 13:1535-1543. doi:10.2147/DDDT.S170969
Ahmed AA, Osman N, Furie R. An evaluation of anifrolumab for use in adults with systemic lupus erythematosus. Expert Rev Clin Immunol. 2022;18(11):1095-1106. doi:10.1080/1744666X.2022.2123793
Burki TK. FDA approval for anifrolumab in patients with lupus. Lancet Rheumatol. 2021;3(10):e689. doi:10.1016/S2665-9913(21)00291-5
SAPHNELO (anifrolumab-fnia) [Prescribing Information]. AstraZeneca. Published September 2022. https://den8dhaj6zs0e.cloudfront.net/50fd68b9-106b-4550-b5d0- 12b045f8b184/44b6985c-8268-46b1-ba3e-2bb43bfd4d4c/44b6985c- 8268-46b1-ba3e-2bb43bfd4d4c_viewable_rendition v.pdf. Accessed June 5, 2023.
van Vollenhoven RF, Hahn BH, Tsokos GC, et al. Efficacy and Safety of Ustekinumab in Patients With Active Systemic Lupus Erythematosus: Results of a Phase II Open-label Extension Study. J Rheumatol. 2022;49(4):380-387. doi:10.3899/jrheum.210805
van Vollenhoven RF, Kalunian KC, Dörner T, et al. Phase 3, multicentre, randomised, placebo-controlled study evaluating the efficacy and safety of ustekinumab in patients with systemic lupus erythematosus. Ann Rheum Dis. 2022;81(11):1556-1563. doi:10.1136/ard-2022-222858
Morand EF, Vital EM, Petri M, et al. Baricitinib for systemic lupus erythematosus: a double-blind, randomised, placebo-controlled, phase 3 trial (SLE-BRAVE-I). The Lancet. 2023;401(10381):1001-1010. doi:10.1016/S0140-6736(22)02607-1
Ginzler EM, Wax S, Rajeswaran A, et al. Atacicept in combination with MMF and corticosteroids in lupus nephritis: results of a prematurely terminated trial. Arthritis Res Ther. 2012;14(1):R33. doi:10.1186/ar3738
Illei GG, Takada K, Parkin D, et al. Renal flares are common in patients with severe proliferative lupus nephritis treated with pulse immunosuppressive therapy: Long-term followup of a cohort of 145 patients participating in randomized controlled studies. Arthritis Rheum. 2002;46(4):995-1002. doi:10.1002/art.10142
Tamirou F, D’Cruz D, Sangle S, et al. Long-term follow-up of the MAINTAIN Nephritis Trial, comparing azathioprine and mycophenolate mofetil as maintenance therapy of lupus nephritis. Ann Rheum Dis. 2016;75(3):526-531. doi:10.1136/annrheumdis-2014-206897
Singh JA, Hossain A, Kotb A, Wells GA. Comparative effectiveness of immunosuppressive drugs and corticosteroids for lupus nephritis: a systematic review and network meta-analysis. Syst Rev. 2016;5(1):155. doi:10.1186/s13643-016-0328-z
Akhavan PS, Su J, Lou W, Gladman DD, Urowitz MB, Fortin PR. The Early Protective Effect of Hydroxychloroquine on the Risk of Cumulative Damage in Patients with Systemic Lupus Erythematosus. J Rheumatol. 2013;40(6):831-841. doi:10.3899/jrheum.120572
Mok CC. Biological and targeted therapies of systemic lupus erythematosus: evidence and the state of the art. Expert Rev Clin Immunol. 2017;13(7):677-692. doi:10.1080/1744666X.2017.1323635
Hanly JG, Su L, Urowitz MB, et al. Mood Disorders in Systemic Lupus Erythematosus: Results From an International Inception Cohort Study. Arthritis & Rheumatology. 2015;67(7):1837-1847. doi:10.1002/art.39111
Gupta M. Depression in systemic lupus erythematosus: A systematic review. Int J Students Res. 2015;5(2):21–27. doi: 10.4103/2321- 6662.210493
Danoff-Burg S, Friedberg F. Unmet Needs of Patients with Systemic Lupus Erythematosus. Behavioral Medicine. 2009;35(1):5-13. doi:10.3200/BMED.35.1.5-13
Greco CM, Rudy TE, Manzi S. Effects of a stress-reduction program on psychological function, pain, and physical function of systemic lupus
erythematosus patients: A randomized controlled trial. Arthritis Care Res (Hoboken). 2004;51(4):625-634. doi:10.1002/art.20533
Braga J, Campar A. Biological causes of depression in Systemic Lupus Erythematosus. Acta Reumatol Port. 2014;39(3):218-226. https://europepmc.org/article/med/25326402. Accessed May 28, 2023.
Bertsias GK, Ioannidis JPA, Aringer M, et al. EULAR recommendations for the management of systemic lupus erythematosus with neuropsychiatric manifestations: report of a task force of the EULAR standing committee for clinical affairs. Ann Rheum Dis. 2010;69(12):2074-2082. doi:10.1136/ard.2010.130476
Akhondzadeh S, Jafari S, Raisi F, et al. Clinical trial of adjunctive celecoxib treatment in patients with major depression: a double blind and placebo controlled trial. Depress Anxiety. 2009;26(7):607-611. doi:10.1002/da.20589
Tan LPL, Tan LES. Electroconvulsive Therapy for Severe Neuropsychiatric Lupus With Psychosis. J ECT. 2013;29(3):243-246. doi:10.1097/YCT.0b013e3182809c01
Bauman A, Barnes C, Schrieber L, Dunsmore J, Brooks P. The unmet needs of patients with systemic lupus erythematosus: Planning for patient education. Patient Educ Couns. 1989;14(3):235-242. doi:10.1016/0738-3991(89)90036-0
Giffords ED. Understanding and Managing Systemic Lupus Erythematosus (SLE). Soc Work Health Care. 2003;37(4):57-72. doi:10.1300/J010v37n04_04
Tsai J, Chien AL. Photoprotection for Skin of Color. Am J Clin Dermatol. 2022;23(2):195-205. doi:10.1007/s40257-021-00670-z
Mak A, Cheung MWL, Chiew HJ, Liu Y, Ho RC man. Global Trend of Survival and Damage of Systemic Lupus Erythematosus: Meta-Analysis and Meta-Regression of Observational Studies from the 1950s to 2000s. Semin Arthritis Rheum. 2012;41(6):830-839. doi:10.1016/j.semarthrit.2011.11.002
Yavuz S, Lipsky PE. Current Status of the Evaluation and Management of Lupus Patients and Future Prospects. Front Med (Lausanne). 2021;8. doi:10.3389/fmed.2021.682544
Montigny PM, Houssiau FA. New Treatment Options in Lupus Nephritis. Arch Immunol Ther Exp (Warsz). 2022;70(1):11. doi:10.1007/s00005- 022-00647-8
Hanly JG, O’Keeffe AG, Su L, et al. The frequency and outcome of lupus nephritis: results from an international inception cohort study. Rheumatology. 2016;55(2):252-262. doi:10.1093/rheumatology/kev311
DISCLAIMER
The information provided in this course is general in nature, and it is solely designed to provide participants with continuing education credit(s). This course and materials are not meant to substitute for the independent, professional judgment of any participant regarding that participant’s professional practice, including but not limited to patient assessment, diagnosis, treatment, and/or health management. Medical and pharmacy practices, rules, and laws vary from state to state, and this course does not cover the laws of each state; therefore, participants must consult the laws of their state as they relate to their professional practice.
Healthcare professionals, including pharmacists and pharmacy technicians, must consult with their employer, healthcare facility, hospital, or other organization, for guidelines, protocols, and procedures they are to follow. The information provided in this course does not replace those guidelines, protocols, and procedures but is for academic purposes only, and this course’s limited purpose is for the completion of continuing education credits.
Participants are advised and acknowledge that information related to medications, their administration, dosing, contraindications, adverse reactions, interactions, warnings, precautions, or accepted uses are constantly changing, and any person taking this course understands that such person must make an independent review of medication information prior to any patient assessment, diagnosis, treatment and/or health management. Any discussion of off-label use of any medication, device, or procedure is informational only, and such uses are not endorsed hereby.
Nothing contained in this course represents the opinions, views, judgments, or conclusions of RxCe.com LLC. RxCe.com LLC is not liable or responsible to any person for any inaccuracy, error, or omission with respect to this course, or course material.
ⓒ RxCe.com LLC 2022: All rights reserved. No reproduction of all or part of any content herein is allowed without the prior, written permission of RxCe.com LLC.
